Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.


|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected. No texting or chat messages, please. Ordinary e-mails are welcome.
 I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles that you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
 Describe the following anatomic defects, how they arise, and what may
happen as a result:
Describe the following anatomic defects, how they arise, and what may
happen as a result:Hypospadias
Epispadias
Phimosis
Paraphimosis
Peyronie's
Pearly papules
Hydrocele
Varicocele
Spermatocele
Distinguish priapism from a normal erection, explain why it can be serious, and mention some illnesses and how they cause priapism.
Describe how infectious urethritis occurs, and briefly describe reactive arthritis. ("Reiter's").
Describe the range of HPV-induced and syphilis-induced pathology in the male. Give an account of squamous cell carcinoma of the penis, and its various precursor lesions.
Tell what a general physician needs to know about cryptorchidism, epididymitis, orchitis, and torsion.
Recognize each of the common germ cell tumors microscopically, and describe their gross appearances, frequencies, known risk factors, markers, and behavior. Recognize and describe Leydig cell adenomas and testicular lymphomas.
Tell what can cause pain in the prostate. Give accounts of bacterial and nonbacterial prostatitis.
Tell what we know about the etiology, pathogenesis, pathophysiology, anatomic pathology, and consequences of prostatic hyperplasia.
Describe adenocarcinoma of the prostate in terms of its etiology, pathogenesis, markers, anatomic pathology, patterns of growth and spread, and clinical diagnosis, including the use of the lab. Read a prostate needle biopsy, distinguishing cancer from the other common lesions, and do simple grading of adenocarcinoma.
Use your pathology knowledge, along with your knowledge from other lectures in this unit, to help answer common individual patient questions in the primary care setting.
![]() KCUMB Students
KCUMB Students
"Big Robbins" -- Lower Urinary / Male
Lectures follow Textbook
QUIZBANK
Men's problems (all)
I used to pray, "Lord, give me chastity, but not yet!"
-- St. Augustine, Confessions
A man should definitely get married. If it's a good marriage, he will be happy. If it's a bad marriage, he will become philosophical.
-- Socrates
Iron John. Iron John. What MY wife wants is iron-ING John!.
-- Anonymous man
{47692} index identifies this as "human male"
{10268} prostate, normal gross section
{11762} prostate, normal histology
{11763} prostate, normal histology
{17008} prostate, normal histology
{15027} prostate, normal histology, with concretion
{00083} testis, normal histology
{20941} testis, normal histology, good Leydig cell
{15016} epididymis, normal histology, with sperms
{15026} seminal vesicles, normal histology
{25832} sperms, Pap stain; note two-headed sperm in center (not too unusual)
![]() Testis, epididymis, penis
Testis, epididymis, penis
"Pathology Outlines"
Nat Pernick MD
Even where there is no mensch, strive to be a mensch.
-- Rabbi Hillel
While you are away, movie stars are taking your women. Robert Redford is dating your girlfriend. Tom Selleck is kissing your lady. Bart Simpson is making love to your wife.
--"Baghdad Betty", Iraqi disk jockey, during the first Gulf War
Love, who is fairest among the immortal gods,
loosener of limbs, by whom all gods and all men
find their thoughts and wise counsels overcome in their hearts.
--Hesiod
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
HYPOSPADIAS (Urol. Clin. N.A. 37: 159 & 167, 2010): Abnormal opening of the urethra onto the ventral surface of the penis or scrotum.
This results from failure of fusion of the urethral folds, i.e., it is a minimal form of feminization.
* And of course there are a host of statistical differences in other hormonal levels between these youngsters and their normal counterparts, including high-levels of mullerian inhibiting substance (J. Urol. 168: 1784, 2002).
* A Danish study showing no link between Mom eating non-organic food during pregnancy and Junior having hypospadias (J. Urol. 189: 1077, 2013) got reported accurated in the lay press. A supposed link to Mom currently eating non-organic butter and cheese looks like recall bias to me.
Usually, wherever the opening occurs, a fibrous band (chordee) distal to it will cause ventral curvature of the erect penis.
There is often associated cryptorchidism, ureterovesical reflux, inguinal hernia, and/or other developmental problems (J. Postgrad. Med. 37: 140, 1991). A massive review of the anatomy: J. Urol. 160: 1108, 1998.
* In the late 1990's, a "green" claim was presented to the public to the effect that hypospadias had doubled in frequency during the previous twenty years, and the cause is chemical pollutants acting as "endocrine disruptors", after an initial CDC report seemed to spot a trend (Pediatrics 100: 831, 1997). There was a huge hoopla and a bunch of studies. All confirmed there's no increase in either incidence or repair rates (Urology 57: 151, 2001; Env. Health Perspect. 108: 463, 2000; Pediatrics 115: e495, 2005; Arch. Dis. Child. Fetal-Neo. 89: F149, 2004). In the old days, many children with the birth defect were simply not placed in registries as they are today. The "green" claim that DDT is the cause also fails under examination: Env. Health. Perspect. 113: 220, 2005. Even Greenpeace finally dropped these claims from their website in 2008. The "pop" wisdom of a link to pesticides is under continual study; the latest article found no link with most pesticides, dubious links with a few (Pediatrics 132: e1216, 2013).
EPISPADIAS: Abnormal opening of the urethra on the dorsal surface of the penis.
Epispadias is actually a form of exstrophy of the urinary bladder. There is usually an associated separation of the pubic bones and inadequacy of the urinary sphincters. Incontinence and bladder infections are usual. There are many variants (J. Urol. 141: 903, 1989).
Epispadias is much less common than hypospadias and more difficult to correct surgically.
* There are varying degrees of severity, and adequate folic acid intake around the time of conception seems to help prevent the worst cases (J. Ped. 159: 825, 2011). It now appears that boys conceived through reproductive technology are at greater risk for epispadias, though whether this reflects the technology or the subfertility problems of a parent is unknown (J. Urol. 189: 1524, 2013).
PHIMOSIS: Present when the prepuce cannot be retracted over the corona.
Phimosis may be congenital, the orifice of the prepuce being too small.
![]() Congenital phimosis
Congenital phimosis
Wikimedia Commons
More often, phimosis is due to poor hygiene ("acquired phimosis"), resulting in chronic inflammation and scar contracting, which sets up a vicious cycle requiring circumcision.
Such an ongoing infection of the glans and prepuce is called BALANOPOSTHITIS. Many organisms may participate. All about it: Urol. Clin. N.A. 19: 143, 1992.
{24987} balanitis
PARAPHIMOSIS results when a tight foreskin is forcibly retracted, and edema of the glans prevents its replacement. This can quickly lead to acute urinary retention and even gangrene of the glans.
PRIAPISM: A persistent, non-pleasurable erection (Mayo Clin. Proc. 72: 350, 1997; Urol. Clin. N.A. 28: 391, 2001).
* "Priapus" was the classical-era Greek god of erections, but priapism is no joke.
Most cases of priapism are probably due to obstruction of the deep dorsal vein of the penis. Typically the corpus spongiosum is uninvolved (i.e., the urethra and glans stay limp).
Causes include sickle cell disease (J. Urol. 145: 65, 1991), black widow spider bite (famous; Pediatrics 114: e128, 2004), the Brazilian wandering "Viagra" spider (no, not pleasant), leukemia, metastatic cancer, papaverine treatment of impotence (rare), and trauma (J. Urol. 148: 380, 1992); many cases are "idiopathic" (i.e., something is causing abnormal thrombosis).
URETHRITIS
GONORRHEA and "NON-GONOCOCCAL URETHRITIS" ("urethral syndrome", due to
chlamydia![]() ,
mycoplasma, others), are important sexually-transmitted diseases.
,
mycoplasma, others), are important sexually-transmitted diseases.
We can see and culture gonorrhea, and do probes for it and chlamydia. Researchers trying to figure out what's causing "the drip" this year check first-stream urine for DNA from a host of known pathogens. One group checked for gonorrhea, Chlamydia trachomatis, Mycoplasma genitalium, Ureaplasma parvum and urealyticum, herpes 1 and 2, adenovirus, and Gardnerella -- but for some reason not for trichomonas (known to be an important cause -- J. Inf. Dis. 188: 465, 2003). There's plenty of urethritis due to each bug in the study. Men tend to get herpes 1 and adenovirus from oral sex (especially from other men), and most of the others from unprotected vaginal sex with women. And there's at least one unknown entity transmitted by oral sex. Update on all this in J. Inf. Dis. 193: 336, 2006.
|
|
REACTIVE ARTHRITIS (formerly "Reiter's syndrome"): the enigmatic triad of (1) arthritis involving many joints, (2) conjunctivitis, and (3) urethritis (for this handout, anyway) following a bacterial infection. It's most familiar as a man's disease following sexually-transmitted urethritis, and lasts for several months. Update Am. Fam. Phys. 60: 499, 1999.
The urethritis is usually
chlamydia![]() ,
and there is now substantial support for the idea that chlamydia
do indeed infest the
synovium (Arth. Rheum. 35: 521, 1992 was the first paper).
If the initial episode of urethritis is treated appropriately,
reactive arthritis is much less likely to ensue (Arth. Rheum. 35: 190, 1992).
Gonorrhea may also produce reactive arthritis.
,
and there is now substantial support for the idea that chlamydia
do indeed infest the
synovium (Arth. Rheum. 35: 521, 1992 was the first paper).
If the initial episode of urethritis is treated appropriately,
reactive arthritis is much less likely to ensue (Arth. Rheum. 35: 190, 1992).
Gonorrhea may also produce reactive arthritis.
When triggered by a gut infection, it's often salmonella, shigella, campylobacter, or yersinia.
There's an impressive proliferation of T-cells specific for chlamydia (when it's the cause) within the affected joints (Arth. Rheum. 34: 588, 1991).
Most patients are positive for HLA-B27.
Patients with reactive arthritis syndrome are likely to have circinate balanitis (red filagree rash on the glans), keratoderma blennorrhagica (hard bumps) on the soles, ulcers of the mouth, iritis, or even ankylosing spondylitis ("poker-back").
Before assuring a guy his urethritis "must be due to chlamydia" (because his gonococcal culture came back negative), ask whether he eats lots of those little Mexican peppers. The hot chemical in these can and does cause a urethritis.
There are a host of other reactive arthritis syndromes. With more effective treatment for chlamydial urethritis, discussions of reactive arthritis secondary to urethritis (classic reactive arthritis) are becoming few.
* Christopher Columbus's arthritis-and-red-eyes was likely due to reactive arthritis: Am. J. Med. Sci. 332: 123, 2006.
* Hans Reiter described "Reiter's" in 1916 as reactive arthritis following diarrhea rather than urethritis; his wasn't the first description. He went on to become one of the Buchenwald concentration camp "experimenters". This is one of the few eponyms your lecturer prefers not to use.
PEYRONIE'S DISEASE ("penile induration"): Proliferation of dense fibrous tissue involving a portion of the fascia. This leads to curvature of erection and some discomfort. Most cases are mild but some can be disabling. * Other names: "painful erection in the wrong direction", "squint of the cock" (Osler).
This is one of several abnormal hyperplasias of fibrous tissue that are sometimes called "fibromatoses": another common one is palmar fibromatosis (Dupuytren's contracture of the hand) which often occurs along with Peyronie's disease. Photomicrographs: J. Urol. 157: 282, 1997.
* Metaplastic ossification and calcification are common.
The etiology is completely obscure. Trauma as a possible cause: Yes (J. Urol. 158: 1388, 1997); no (J. Urol. 172: 186, 2004).
Treatment for Peyronie's disease is not very satisfactory, and many patients eventually require a penile prosthesis. New procedures: J. Urol. 167: 2066, 2002. Natural history of Peyronie's: J. Urol. 144: 1376, 1990.
{25287} Peyronie's, histology
WARTS: There are two common "warts" involving the penis:
CONDYLOMA ACUMINATUM ("pointed knob"): a papillary, keratinizing lesion caused by the sexually-transmitted "human papilloma virus" (usually strain 6). In males, it commonly occurs in the urethral meatus, which is perhaps the worst possible location (why?)
To spot HPV involvement, wet the man's external genitalia with acetic acid ("* sheep dip") and involved areas show white ("acetowhite", as on the uterine cervix). It's now called "androscopy" (J.F.P. 29(3): 286, 1989). See J. Urol. 143: 920, 1990 for a discussion on criteria for diagnosing HPV histologically on biopsies of acetowhite areas. All about the histopathology of HPV, warts and men: Arch. Derm. 128: 495, 1992.
We have lots of ways of dealing with these warts, ranging from electrocautery and lasers to interferon and fluorouracil (Postgrad. Med. 86: 197, 1989, by my friend Dr. Ila Peterson). It's important to treat both partners, since this reduces reinfection.
{24460} condyloma, gross
{25098} condyloma, histology; note HPV-effect (shrunken, wrinkled nuclei, perinuclear halo)
![]() Warts
Warts
Male patient photos
Health Awareness Connection
CONDYLOMA LATUM ("flat knob"): groups of flat-topped lesions that
may ooze serous fluid; caused
by secondary syphilis![]() . Typically occur in skin folds.
. Typically occur in skin folds.
GENITAL HERPES ![]() is familiar to you.
is familiar to you.

PEARLY PENILE PAPULES ("PPP on the pee-pee") aren't warts at all, but little bumps, sometimes hairy, which pop up in young adults, especially on the corona. Each is a single big dermal papilla. No need to treat. About one man in 100 has spectacular ones, and I get a very large number of questions from visitors to my site. I point out they can be considered a "plus". They may be removed using today's lasers (JAMA Derm 149: 748, 2013).
|
|
|
|
![]() Pearly penile papules
Pearly penile papules
Classic look
Wikimedia Commons
CANCER OF THE PENIS: Almost all are variations on squamous cell carcinoma. Review Urol. Clin. N.A. 37: 343, 2010.
This is a disease of older men, and it originates on glans and prepuce.
Only 1% of cancers among American men begin on the penis; the figure is as high as 18% in the Orient. In the US, there are just around 1200 cases of invasive cancer each year, and around 300 deaths.
Risk factors include phimosis, smegma, and balanoposthitis. However, by far the strongest risk is infection with HPV, notably HPV-16, for which a large majority of affected men are positive. The other risk factors seem to create the fertile soil where Nowell's Law can operate.
* The genetic markers are just being worked out. Tumors positive for phTOR, pelF4E and p53 are more aggressive; pERK and p4E-BP1 with less aggressive tumors, pmTOR and p53 with non-HPV-expressing tumors.
Good reading: Cancer of the penis is the second most-common male cancer, and cancer of the cervix the most common female cancer, on the island of Bali, where the men are uncircumcised and unhygienic, and both cancers are strongly HPV-linked (Cancer 64: 559, 1989).
Males circumcised as infants almost never get cancer of the penis. The incidence is much lower in those circumcised at a later age than among the uncircumcised.
About 50% are classic squamous carcinomas, the rest variants on squamous cell carcinomas.
* The basaloid variant (very little cytoplasm), which usually arises on the glans, is quite anaplastic and very aggressive.
* The "verruciform" variants are markedly exophytic. Among these the verrucous variant (very little anaplasia, no fibrovascular cores, no perinuclear clearing, lower border is pushing) has very little propensity to metastasize (J. Urol. 176: 1431, 2006.) The papillary (fibrovascular cores, no perinuclear clearing) and condylomatous (upper portion with fibrovascular cores and perinuclear clearing, lower portion a squamous cancer) are also rather tame. Pathologists have difficulty sorting the three verrucous variants out.
Today's patient is likely to be offered laser therapy instead of surgery (J. Urol. 169: 2118, 2003). Mohs' microsurgery seems effective: J. Urol. 178: 1980, 2007.
Carcinoma of the penis spreads to the inguinal lymph nodes. The majority of patients are cured, but more or less mutilated.
{46450} squamous cancer of the penis, metastatic to the head
{46451} squamous cancer of the penis, with inguinal node metastasis
![]()
![]() Cancer of the Penis
Cancer of the Penis
Dino Laporte's PathosWeb
PREMALIGNANT LESIONS OF THE PENIS
ERYTHROPLASIA OF QUEYRAT: A raised, velvety plaque on the uncircumcised glans or prepuce.
Histologic study shows dysplasia of the squamous epithelium.
The term "erythroplasia of Queyrat" seems to be passing out of use. Historically, it's been used for not-very-anaplastic squamous carcinomas in situ on the glans, while Bowen's includes the more outrageously anapastic ones located anywhere (penis or elsewhere). We treat them the same.
* Treatment has historically been with topical 5-fluorouracil, whether patients are HPV-positive or negative (lately most seem to be negative Dermatology 223: 52, 2011). Imiquimod (the immune-modulator widely used nowadays in dermatology) also seems to work (J. Am. Acad. Derm. 55: 901, 2006).
A minority of cases (5-30%, estimates vary) develop into squamous cell carcinoma if not removed.
{25095} erythroplasia of Queyrat, gross
{25096} erythroplasia of Queyrat, histology
BOWEN'S DISEASE: Carcinoma in situ of the skin, most often on the penis or scrotum in men. Look for individual very weird cells with lots of mitoses.
Some cases (maybe 10%) develop into invasive squamous cell carcinoma.
* There is a popular claim that the appearance of Bowen's disease on the skin heralds the growth of another malignancy internally. I am not aware of any reason to believe this is true.
BOWENOID PAPULOSIS: Multifocal intraepithelial neoplasia, caused by HPV-16. The atypia is mild and this often regresses on its own.
* Future pathologists: Bowenoid papulosis tends to spare the hairs and involve the sweat glands. Bowen's disease tends to spare the sweat glands and involve the hairs.
* Other dysplastic lesions are being classified. As in the vulva, a keratinizing dysplasia can be spotted by its dense keratin, even if the cells are only mildly anaplastic.
Giant condyloma of Buscké-Lowenstein, that some say is just a mild verrucoud carcinoma: Another HPV-related, very ugly cauliflower-like lesion. (See Arch. Derm. 126: 1208, 1990; J. Urol. 141: 950, 1989). Invasive cancer can breed here.
{25101} verrucous carcinoma, gross
{25102} verrucous carcinoma, histology
A standing army is like a standing member. It's an excellent assurance of domestic tranquility, but a dangerous temptation to foreign adventure.
-- Elbridge Gerry, Constitutional Convention 1787
|
|
|
|
|
MALE INFERTILITY
Leave the pathology of these problems to specialists. Male infertility (i.e., she's fertile, and they've
been trying without success for a year) has a variety of causes, known (Down's, Klinefelter's, old
torsion, old mumps![]() ,
cryptorchidism, some cases of old age, after radiation, after some kinds of
chemotherapy -- all will give a "Sertoli-only" histology) and unknown.
,
cryptorchidism, some cases of old age, after radiation, after some kinds of
chemotherapy -- all will give a "Sertoli-only" histology) and unknown.
Spermatogenesis can be temporarily diminished or even stopped by a host of factors ranging from heavy drinking to anabolic steroid abuse to bicycling.
Obstruction of the sperm passages (can you think of etiologies?) may be more amenable than the above to surgical help. Or a sperm can be obtained by aspiration from the testis in order to fertilize an egg.
Many men without obstruction have maturation arrest of spermatogenesis; especially when this is uniform, the man is likely to harbor a genetic abnormality (often a microdeletion on the Y-chromosome), and is unlikely to be a father by any means (J. Urol. 178: 608, 2007). A common infertility gene is hemizygosity for mutant TEX11 on the X-chromosome(NEJM 372: 2097, 2015).
The pesticides DBCP (dibromodichloropropane, "Nemagon") and chlordecone do cause infertility in men, by preventing the sperms from differentiating. This has been known since the 1950's, and the fact that companies still used them overseas after they were rightly banned in the US is all-too-typical. The rat model, and an easy way to restore their fertility: Tox. Sci. 76: 418, 2003.
{00086} testicular atrophy, no sperms
{25154} testicular feminization (no sperms, hyperplasia of useless Leydig cells, why?)
* Some guys ("fertile eunuchs", a misnomer) just don't make LH, and may or may not make FSH. They become fertile if you replace the gonadotropins.
* Evaluation of the azoospermic patient, by Jon Jarow MD, a lifetime friend of your lecturer: J. Urol. 142: 62, 1989. He's also reviewed anabolic-steroid induced hypogonadotropic hypogonadism: Am. J. Sports Med. 18: 429, 1990.
Slow-learner guy with large testes: Fragile X!
CRYPTORCHIDISM (cryptorchism): Incomplete descent of the testis into the scrotal sac. Review Am. Fam. Phys. 62: 2037, 2000.
Unilateral or bilateral cryptorchidism occurs in around 4% of prepubertal boys. (Maybe 1 boy in 10 is born with at least one not fully descended, but the majority do descend in the first year.) Cryptorchid testes may be found anywhere along the normal route of descent (abdomen, inguinal canal, prepubic). Occasionally a testis that is present in the scrotum at birth may retract back into the abdomen (or have the cord fail to grow as the boy does: J. Urol. 157: 1892, 1997); this is also cryptorchidism and has the same associated risks and basically the same histology: J. Urol. 162: 878, 1999.
The epididymis is likely to be malformed or at least elongated. See J. Urol. 143: 340, 1990.
Some centers biopsy each testis at the time of surgery, and administer gonadotropin releasing hormone if the histology shows very few germ cells per tubule (read about it J. Urol. 169: 659, 2003). It turns out that biopsy at surgery is a poor predictor of whether he'll be fertile as an adult (J. Urol. 188(4S): 1429, 2012.)
ECTOPIC TESTIS is less common; it may stray into the superficial inguinal region, penis, or femoral sheath.
VANISHING TESTIS -- among boys with cryptorchidism, the testis (testes) cannot be found by palpation, though Junior is a normal male otherwise. A tiny fibrous nubbin, maybe with some Sertoli cells (Am. J. Clin. Path. 136: 872, 2011). These probably don't turn malignant.
Failure of the testes to descend into the scrotum causes problems:
In 1989, 300 brave Danish men who had been treated for cryptorchidism consented to needle biopsy; 5 had carcinoma in situ and 2 other had already been treated for testicular cancer (J. Urol. 142: 998, 1989).
Most cryptorchidism is idiopathic. It may be accompanied by other developmental abnormalities, diethyl-stilbestrol exposure, and poorly-understood anatomic and hormonal problems.
EPIDIDYMITIS AND ORCHITIS: Ouch!
|
|
NONSPECIFIC INFECTIONS of the contents of the scrotum are usually complications of urinary tract infection, instrumentation (for example, clean-intermittent catheterization: Eur. Ur. 22: 53, 1992), or prostate biopsy / surgery.
GONORRHEA: the infection often spreads to the epididymis, less often the testis.
{40116} abscess of the epididymis, gonococcal I'd bet; the tan structure with the white rim is a cross-section of testis
|
|
|
|
* The one tumor of the epididymis that's at all common is a papillary cystadenoma seen in von Hippel-Lindau (Arch. Path. Lab. Med. 134: 630, 2010; some say it arises in the rete).
MUMPS![]() :
orchitis is common in adolescents and adults unfortunate to catch
mumps in this day and age. It usually follows the onset of parotitis by a
week or so, and may cause atrophy of the germinal epithelium and infertility. The Leydig cells are
spared.
:
orchitis is common in adolescents and adults unfortunate to catch
mumps in this day and age. It usually follows the onset of parotitis by a
week or so, and may cause atrophy of the germinal epithelium and infertility. The Leydig cells are
spared.
TUBERCULOSIS![]() : granulomas involving the epididymis; may spread to the testis.
: granulomas involving the epididymis; may spread to the testis.
{25221} tuberculosis of epididymis
TORSION OF SPERMATIC CORD ("torsion of the testis"): Am. Fam. Phys. 74: 1739, 2006
Twisting of the spermatic cord is likely to result in venous infarction and gangrene in a few hours. This is quite common, especially in children and adolescents.
Spasm of the cremaster muscle keeps the process going (pain-spasm-pain cycle). The involved testis is painful and elevated; the cord is typically twisted 540 degrees.
There may or may not be a history of trauma (often minor, as in baseball or break dancing; see JAMA 256: 3366, 1984).
The underlying problem may be abnormal fixation of the testis or cryptorchidism. Ask a urologist about the "bell clapper" deformity, with the tunica vaginalis running too high up the spermatic cord. This supposedly results in torsion after intermittent episodes of testicular pain (J. Urol. 148: 134, 1992). Of course, once the process starts, spasm of the cremaster muscle still plays a role.
You, the physician, may be able to untwist the cord manually. If not, emergency surgical intervention is indicated. You'll learn about the diagnostic pitfalls (imaging studies can be unreliable, etc.) on rotations.
An old infarcted (hyalinized) testis is a common surprise finding in autopsy series -- suggesting that the diagnosis of torsion is often missed.
More seriously, unilateral spermatic cord torsion can somehow damage the opposite testis. Nobody knows how this happens (J. Urol. 144: 366, 1990); reflex vasoconstriction? autoimmunity?
Torsion of the appendices of the testis and epididymis are painful but not so serious.
A person can also suffer loss of one testis by catching it in a hernia. (There's no room here to talk about hernias!)
* As noted above, after unilateral torsion of a testis, there is some increase in risk of infertility even though there was never physical damage to the other testis. No one understands the reason; a group of men who had survived torsion underwent contralateral biopsy and all had some increase in apoptosis of the germinal cells (J. Urol. 160: 1158, 1998).
The schoolyard pranks "wedgies" and "sack tapping" have resulted in a number of cases of testicular injury.
{10892} torsion, gross
{25208} torsion, gross
{10898} testes: normal vs. "atrophic" (could have been old torsion, old mumps, or whatever)
Scrotal squamous cell carcinoma is the subject of the famous chimney sweep story. FOURNIER'S GANGRENE is a synergistic bacterial infection that produces the dreaded "black sack disease" (no joke; most common in debilitated individuals; huge review Br. J. Surg. 87: 718, 2000; vacuum dressings Am. J. Surg. 197: 168, 2009).
![]() Fournier's gangrene
Fournier's gangrene
Synergistic gangrene
Photo from surgical-tutor.org.uk
![]() Fournier's gangrene
Fournier's gangrene
Synergistic gangrene
From a Vietnamese site
Many older men get a few angiokeratomas (hemangiomas with each dermal papilla stretched wide by a single ectatic blood vessel), especially on their scrotums, and this doesn't mean Fabry's.
| GERM CELL TUMORS (cancer of the testis): Cancer of the germinal epithelium. These tumors are the commonest solid cancers of men in their 20's and 30's. In 2006, there were around 8250 cses and 370 deaths in the US. Pathologists see Arch. Path. Lab. Med. 131: 1267, 2007; J. Clin. Path. 61: 20, 2008; Arch. Path. Lab. Med. 136: 435, 2012. Clinicians see Lancet 367: 754, 2006. |  |
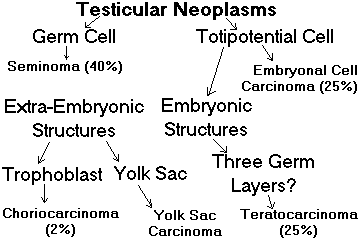
About 95% of tumors of the testis are malignant germ cell tumors.
It is now clear that the cells of origin of the "germ cell tumors" really are the germ cells.
In adults (but not in children, and not in spermatocytic seminoma), the in situ lesion INTRATUBULAR GERM CELL NEOPLASIA, UNCLASSIFIED (IGCNU) can usually be identified in nearby seminiferous tubules (Arch. Pathol. Lab. Med. 109: 555, 1985 for the original pictures).
The in-situ precursor is now easy to spot.
* IGCNU cells usually stain with placental alkaline phosphatase (PLAP), cKit/CD117, p53, and OCT3/4 (the latter a seminoma / embryonal cell carcinoma nuclear marker.) The newest entries are UTF1, a seminoma-embryonal cell marker (Am. J. Clin. Path. 134: 604, 2010) and TCL1 (Am. J. Clin. Path. 133: 762, 2010).
Embryonal carcinoma in situ: Arch. Path. Lab. Med. 126: 48, 2002. Microinvasive carcinoma: Cancer 70: 659, 1992.
We believe that most or all IGCNU will turn invasive if left alone, half within five years. The tendency now is to remove an affected testis.
A German group examined sections from all males coming to autopsy, and found that the prevalence of carcinoma in situ of the testis (6 out of 1388) was good match for lifetime risk, i.e., it usually starts in situ, and the in situ lesion usually turns invasive. (J. Urol. 173: 1577, 2005) See below.
Almost all germ cell tumors of the testis present as painless, non-tender masses in the testis. The primary may be occult, especially if it's a pure choriocarcinoma.
Many cause gynecomastia (after puberty) or precocious puberty (children.) Today, the diagnosis is usually obvious based on tumor markers and/or ultrasonography; only rarely is biopsy necessary before radical orchiectomy.
Urologists have special procedures for difficult cases, especially bilateral disease in the man wishing to preserve natural fertility. Sometimes the opposite testis is biopsied in a search for carcinoma in situ. These protocols will change by the time you are in practice.
Risk factors for this disease are poorly understood. They include cryptorchidism and some intersex / gonadal dysgenesis malformations (Arch. Path. Lab. Med. 114: 679, 1990). There are some familial cases (Mayo Clin. Proc. 65: 804, 1990) but if there is an anti-oncogene syndrome, it remains elusive.
Other risk factors are earlier puberty, and supposedly lack of exercise as a kid. Today's boys have both, compared to us men who are now middle-aged, and this is perhaps why cancer of the testis is becoming significantly more common around the world: Br. Med. J. 308: 1393, 1994; J. Urol. 170: 5, 2003; mostly seminomas in the US: Cancer 97: 63, 2003.
* Your lecturer is also unimpressed with a retrospective study in which a man with testicular cancer was 1.7x more likely to admit he had smoked marijuana (Cancer 115: 1215, 2009; Cancer 117: 848, 2011). It makes sense that "recall bias" would be operating -- young men upset about having cancer are more likely to 'fess up to smoking a joint from time to time.
* Old mumps orchitis is probably not a risk factor (Br. J. Cancer 106: 1331, 2012.)
Cancer in a testis confers approximately 50x increased risk of there being at least carcinoma in situ in the opposite testis. No one really knows what to do about this fact: J. Urol. 160: 1353, 1998.
* Anti-Ma2 is an autoantibody most often seen in testicular cancer patients that causes a brainstem and limbic encephalitis (can't move eyes, Parkinsonism, stop talking; Brain 127: 1831, 2004).
* Future pathologists: When you are handling a resected testis, please....
SEMINOMA: cancer that closely resembles young spermatocytes.
Grossly these tumors are homogeneously soft and yellowish.
Tumor cells have "fried egg" appearance (* glycogen-rich cytoplasm; nuclei are big because they are hypertriploid); arranged in masses separated by fibrous septa with a lymphocytic infiltrate, may have syncytiotrophoblast and/or granuloma formation.
* Tumors with more than 30 mitotic figures per 10 hpf have historically been considered more aggressive (the old "anaplastic seminoma") but since cure rates are so high nowadays, this is moot.
Chorionic gonadotropin (hCG) is a tumor marker for the 20% or so of seminomas that contain syncytiotrophoblast (i.e., the man has a positive pregnancy test).
* LDH is sometimes cited as a seminoma tumor marker but of course it's infamously nonspecific.
Seminomas typically metastasize to the retroperitoneal lymph nodes and then to the lungs.
Seminomas are remarkable for their good response to radiation or chemotherapy as appropriate, and even widespread disease can usually be treated with five-year survivals of 95% or better.
* The traditional wisdom is that two years following complete remission, the patient can probably consider himself cured. Later recurrence of seminoma is uncommon but does occur: Cancer 95: 520, 2002 (many of these are the people who had apparently benign teratomas left behind.)
Tumors with histology and response to therapy like testicular seminomas (or other germ cell tumors) also arise in other midline structures including the retroperitoneum, thymus, and pineal ("germinomas"), as well as in the ovary ("dysgerminoma").
* Watch the new tumor marker SALL4, which is reported to be very sensitive and specific for germ cell tumors. Especially if you run into a metastatic tumor of unknown primary, knowing this is of germ cell origin is a marker for curability (Cancer 115: 2640, 2009).
|
{25352} seminoma, gross
{25353} seminoma, histology {08863} seminoma, histology {40217} seminoma, histology (PAS stain for glycogen) {08862} seminoma in situ in the tubular epithelium {25355} spermatocytic seminoma, gross {25173} spermatocytic seminoma, histology |

|
![]() Testicular Seminoma
Testicular Seminoma
Text and photomicrographs. Nice.
Human Pathology Digital Image Gallery
|
|
| 
|
The cells (* usually a mix of large, medium and small, reflecting diploidy / tetraploidy) bear a typical nuclear chromatin pattern looking like the stuck-for-days-unwinding pattern of normal spermatocytes.
* Unlike true seminomas, staining for OCT3/4 and PLAP are negative. There's also usually no glycogen and no lymphocytes
It almost never metastasizes "as itself", but about 5% transform into some sort of sarcoma (Cancer 61: 409, 1988) and can metastasize as such.
EMBRYONAL CELL CARCINOMA: a very primitive cancer that arises in the testis.
Grossly these are grayish-white masses with hemorrhage and necrosis. Microscopically, the tumor cells grow in sheets, knobs, etc.
Future pathologists: distinguish from a seminoma by absent glycogen and positive staining for cytokeratin (seminomas are usually weak or negative). OCT4 is usually positive (as in seminomas, and unlike most other cancers), D2-40 is negative, PLAP is usually negative (distinguising from seminomas), and Ki-1/CD30 is usually positive in embryonal carcinomas but negative in other germ cell tumors.
* Future pathologists only: A cancer with epithelial cell organization but staining negative for EMA (epithelial membrane antigen) is -- if the setting is correct -- likely to be an embryonal cell carcinoma.
* If the tumor seems to be stage I, metastases are much more likely if there is vascular invasion seen in the primary; the pathologist will note this on the report.
|
{23954} embryonal cell carcinoma, lumen of some kind and some wilder stuff
|
 |
![]() Embryonal cell carcinoma
Embryonal cell carcinoma
WebPath Photo
Many embryonal cell carcinomas also contain differentiated structures of a teratoma. (Teratoma + embryonal cell carcinoma = TERATOCARCINOMA).
{25401} teratocarcinoma
{25402} teratocarcinoma
Tumor markers for common mixtures that include embryonal cell carcinoma include hCG (from trophoblast areas), α-fetoprotein (AFP, from yolk-sac areas), and * lactate dehydrogenase (LD, LDH, which is nonspecific and probably of no value).
Tumors with an embryonal cell carcinoma component metastasize to the retroperitoneum and everywhere else.
Embryonal cell carcinomas are radioresistant (unlike seminomas) but are very sensitive to chemotherapy (like seminomas).
Metastases very often mature into benign teratomas during treatment. It is now clear that these are usually (but not always) benign, and that persistently elevated tumor markers can be due to slow leakage from cyst fluid (J. Urol. 171: 168, 2004). Do not overtreat. However, maybe 1 in 5 of these men do eventually have the cancer recur (Cancer 115: 1310, 2009).
Or the cured metastases may turn into scar tissue, or just plain necrotic debris (J. Urol. 142: 1239, 1989).
The response to newer chemotherapy protocols is very good, with at least 85% cures even when metastatic disease is widespread (Cancer 56: 2411, 1985). Nowadays, it's good practice to resect even cannonball metastases to the lung and give additional chemotherapy; about 2/3 will get long-term cures (Ann. Thor. Surg. 91: 1085, 2011).
* Most protocols are now based on ifosfamide and platinum. They are highly successful, and the old retroperitoneal lymph node dissection procedure is now reserved for hard cases. The pathology specimens are often curious, with the tumors much altered by chemotherapy (Cancer 109: 528, 2007); any viable tumor in the specimen is ominous (Cancer 107: 1483 & 1503, 2006). The most infamous after-effect of the traditional retroperitoneal lymph node dissection was the loss of the ability to ejaculate (why?); see J. Urol. 142: 1487, 1989 and Cancer 64: 2399, 1989 for psychological well-being after testicular cancer. There's also a nerve-sparing retroperitoneal lymph node dissection technique that supposedly leave the ability to ejaculate intact (update J. Urol. 169: 1710, 2003); today's surgeons use a laparoscope for stage I non-seminomatous tumors with even less morbidity (Urol. Clin. N.A. 38: 451, 2011; J. Urol. 187: 487, 2012).
Again, a two-year disease-free survival generally indicates cure.
CHORIOCARCINOMA:
The bloodiest solid tumor in pathology; solid areas may be hard to find. It is famously fast-growing.
The malignant cells resemble placenta, and the pathologist must identify cytotrophoblast and syncytiotrophoblast. There are no villi.
HCG levels are always very elevated (serum, urine.)
Choriocarcinoma most often is a component in a teratocarcinoma, but may be pure or mixed with any other germ cell tumor components.
Until recently, choriocarcinoma arising in the testis was always lethal.
Today the prognosis is not much worse than for embryonal cell carcinoma, even if the tumor is "pure choriocarcinoma".
YOLK SAC TUMOR ("endodermal sinus tumor", "orchioblastoma", "infantile embryonal cell carcinoma"):
The commonest testicular tumor of children (but still quite rare), in whom it usually occurs "pure" rather than mixed with other germ cell tumor types.
It is composed of papillary structures (Schiller-Duval bodies) with extracellular globs of α-fetoprotein and α-1-protease inhibitor.
This carcinoma is also unusual because it metastasizes hematogenously.
Response to chemotherapy is very good in kids, and pretty good in adults.
DIFFUSE EMBRYOMA has a layer of yolk sac tumor surrounding an embryonal cell carcinoma, as if it were itself the amnion.
{25175} yolk sac cancer, gross
{11551} yolk sac cancer, histology
![]() Yolk sac carcinoma
Yolk sac carcinoma
Liver
Pittsburgh Pathology Cases
TERATOMAS:
Cystic teratoma of testis is rare (but common in ovary) and seldom contains hair. (Teratomas are the only testicular tumors that are often cystic.)
Solid teratomas are of two types:
Mature solid teratoma is benign, usually occurs in children.
Immature solid teratoma is malignant, usually contains embryonal cell carcinoma (TERATOCARCINOMA) or sometimes squamous cell carcinoma.
Even if an adult's teratoma appears altogether benign, there is likely to be nearby intratubular carcinoma in situ (Cancer 64: 715, 1989); and even if there isn't, it can still metastasize as testicular cancer. It's now generally accepted that "all testicular teratomas in adult men are best considered malignant", though of course the presence of obvious cancer is obviously more ominous.
* Just to confuse things, the WHO has decided that a dermoid cyst (i.e., mostly inside-out skin but with three germ layers) and NO IGCNU nearby is benign regardless of age. However, since these are almost entirely children's lesions (which are benign), and very few are reported from grown men, this seems questionable.
WARNING: Any tumor of germ cell origin may be mixed with any other tumor of germ cell origin.
![]() Mixed germ cell tumor of testis
Mixed germ cell tumor of testis
Great photos
Pittsburgh Pathology Cases
Further, any tumor of germ cell origin may metastasize as another histologic type of germ cell tumor (Am. J. Clin. Path. 97: 468, 1992).
MALIGNANT LYMPHOMA arises in the testes of older men with some frequency. Updates Arch. Path. Lab. Med. 131: 1040, 2007; Am. J. Med. Sci. 336: 336, 2008; Arch. Path. Lab. Med. 135: 1363, 2011. They are the commonest testicular tumor of older men, and tend to be very aggressive, recurring soon after initial treatment and proving refractory to further therapy.
ADENOMATOID TUMOR is a benign, hard spherical nubbin, usually in the head of the epididymis, derived from mesothelium (* positive for EMA, cytokeratin, calretinin was the final proof.) They are quite common.
* Let the pathology team worry about sarcomas of the spermatic cord. Childhood rhabdomyosarcomas are usually curable (Cancer 119: 3228, 2013); adult sarcomas less so.
Germ-cell tumors (seminomas, embryonal cell tumors, teratocarcinomas, choriocarcinomas, and the usual mixtures -- but not spermatocytic seminomas) can and do arise in the retroperitoneum, mediastinum, and pineal "because they are midline structures" (?!). Their behavior is similar to testicular tumors. Review Chest 103-S4: 331-S, 1993.
* Famous testicular cancer victims include funmaker Tom Green (non-seminoma), Olympic gold-medal swimmer Alex Baumann, Russian writer Alexander Solzhenitsyn ("Cancer Ward", had seminoma), cyclist Lance Armstrong (nonseminoma), figure skater Scott Hamilton (non-seminoma), Chinese dissident Chen Ziming, football player Brian Piccolo ("Brian's song"), runner Steve Scott, and more.
STROMAL TUMORS
LEYDIG CELL TUMORS: occur at any age, are usually benign (90%), can produce precocious puberty or gynecomastia. Update Arch. Path. Lab. Med. 131: 311, 2007.
The gross and microscopic appearances are typical for endocrine tumors. Sometimes, the pathologist can make the diagnosis easily by identifying a Reinke crystalloid!
* Criteria for malignancy are necrosis, mitotic figures, local invasion, and nuclear pleomorphism, just like you'd expect. MIB-1, the proliferation marker, seems to be a powerful predictor (Am. J. Surg. Path. 22: 1361, 1998).
The tendency today seems to take the tumor and leave the testis behind, as long as there's no suspicion of malignancy (J. Urol. 178: 507, 2007). A huge British study found NO sex-cord stromal (i.e., Sertoli / Leydig) tumor to have metastasized in recent history (J. Urol. 181: 2090, 2009), though the world literature contains references to this happening.
Kids with some variants of congenital adrenal hyperplasia often develop testicular tumors that mimic adrenal cortex, thought to derive from adrenal rests (J. Clin. Endo. Metab. 92: 612, 2007).
Sertoli cell tumors ("androblastomas"; Urology 25: 1985; Am. J. Clin. Path. 96: 717, 1991), are uncommon. Animal model Am. J. Path. 144: 454, 1994; Urol. Clin. N.A. 27: 529, 2000. Calcified sertolioma / bilateral sertoliomas: think Peutz-Jegher's or Carney's.
* Future pathologists: The tumor marker for Sertoli-Leydig differentiation is inhibin (Am. J. Surg. Path. 22: 615, 1998.) Ask an electron microscopist to show you the Charcot-Bottcher filaments.
![]() Leydig cell tumor
Leydig cell tumor
Pittsburgh Pathology Cases
HYDROCELE: Fluid in the tunica vaginalis. Usually idiopathic, a hydrocele may contain 100 cc or more of serous fluid.
They are common male newborns and these generally self-cure.
If ascites is present and the patient has a patent processus vaginalis, a hydrocele will appear and disappear as the patient changes position.
You can distinguish a hydrocele from a tumor mass by trans-illuminating it with a bright flashlight in a dark room.
* Today's man can choose between traditional surgery and sclerosing therapy.
{24589} hydrocele, gross
HEMATOCELE: Blood in the tunica vaginalis. May follow trauma (J. Urol. 127: 1195, 1982), or warn of an underlying testicular cancer.
{25191} hematocele (guy got kicked probably)
VARICOCELE: Varicosities of the pampiniform plexus, usually on the left side (why?)
This is common in young men, may cause fertility problems by warming the testes.
A new varicocele in an old man often indicates occlusion of the vein by renal cell carcinoma, especially if the veins do not collapse when the patient lies down.
SPERMATOCELE: a cystic lesion up to 1 cm or so in the area of the rete testis, filled with fluid and dead sperms.
|
|
|
|
|
|
|
|
|
PROSTATITIS
Pathologists distinguish three types of acini. The mucosal and submucosal are in the periurethral ("inner") zone, separated by smooth muscle from the external acini ("cortical" / "outer").
Acute and chronic prostatitis are uncomfortable problems, and are common in men who catch sexually-transmitted urethritis or lower urinary tract infections.
E. coli is the most common etiologic agent of both acute and chronic prostatitis.
The diagnosis depends on physical and lab exams.
In acute prostatitis the gland is exquisitely tender. You should probably not attempt to express fluid!
Gonorrhea is an important cause of acute prostatitis (secondary to urethritis; remember it can also cause epididymitis).
{25212} acute prostatitis, gross
{25213} acute prostatitis, histology
In chronic prostatitis the gland is somewhat tender and the prostatic fluid you express contains WBC's and grows bacteria.
If there are ten or more neutrophils / high power field in the urine voided right after prostate massage, probably there will be prostatitis on biopsy (J. Urol. 182: 564, 2009).
Treatment is very difficult because of problems getting antibiotics to the bacteria.
{25214} chronic prostatitis, histology
{25215} chronic prostatitis, histology
In "non-bacterial prostatitis", the findings are as in chronic prostatitis (expect
white cells in the semen), but no organisms grow.
(Probably chlamydia![]() cause some of these infections. See J. Urol. 141: 328 & 332, 1989.)
Trichomonas is another candidate (Am. Fam. Phys. 39: 177, Feb. 1989). Autoimmunity is yet
another: J. Urol. 152: 247, 1994). No longer a taboo subject:
heroic abstinence (no partner, no self-entertainment) makes this problem MUCH
worse (Int. J. Urol. 6: 130, 1999).
cause some of these infections. See J. Urol. 141: 328 & 332, 1989.)
Trichomonas is another candidate (Am. Fam. Phys. 39: 177, Feb. 1989). Autoimmunity is yet
another: J. Urol. 152: 247, 1994). No longer a taboo subject:
heroic abstinence (no partner, no self-entertainment) makes this problem MUCH
worse (Int. J. Urol. 6: 130, 1999).
"Prostatodynia" is a stress-related pain syndrome in which there are no WBC's in the prostatic fluid. Other exacerbating factors include constipation, smoking, coffee, and spices (all of which make an infected prostate hurt more, too. See Urology 26: 320, 1985.)
* "Prostatosis" is an old term for both non-bacterial prostatitis and prostatodynia.
Granulomatous prostatitis (fewer than 1% of prostate biopsies
with inflamation) may be due to TB![]() (hematogenous spread from the lungs), "idiopathic"
(no TB, no caseation, no clues as to the etiology) or * exotic (J. Urol. 143: 365, 1990). * The
histiocytes may resemble cancer cells.
(hematogenous spread from the lungs), "idiopathic"
(no TB, no caseation, no clues as to the etiology) or * exotic (J. Urol. 143: 365, 1990). * The
histiocytes may resemble cancer cells.
* For the truly hard-core, here's the NIH classification of prostatitis (Arch. Path. Lab. Med. 136: 721, 2012):
Type II: Chronic bacterial prostatitis -- chronic infection, many WBC in prostatic fluid but not urine, bacteria
Type IIIA: Chronic prostatitic / pelvic pain syndrome, inflammatory -- many WBC in prostatic fluid, no bacteria
Type IIIB: Chronic prostatitic / pelvic pain syndrome, noninflammatory (few or no WBC in prostatic fluid)
Type IV: Asymptomatic prostatitis. WBC found in the prostatic fluid / semen, or maybe it showed up on a prostate biopsy; if so, this has zero correlation with symptoms. Future pathologists: Don't report it unless it's really striking.
Prostate infarcts, which produce hematuria and a painful lump, usually result from instrumentation that causes arterial thrombosis.
* Squamous metaplasia in prostate epithelium occurs at the edges of infarcts, or in men treated with estrogens or finasteride.
{23968} granulomatous prostatitis
|
|
* A curious fact about prostate pathology is that benign cysts are common (and often seen on ultrasound), and may obstruct, but have never been seriously studied or subtyped by pathologists. See J. Urol. 181: 647, 2009.
PROSTATIC HYPERPLASIA ("benign prostatic hypertrophy or hyperplasia", "BPH"). Review: Disease-a-Month 41: 437, 1995; Urol. Clin. N.A. May 1995.
This is something that happens to most intact men over about age 50; 10% of men living to age 80 will need prostate surgery. Surprisingly, there is remarkably little work on its basic biology.
The normal prostate weighs around 20 gm. Old men's prostates enlarge to 60-200+ gm.
The increased tissue is nodular overgrowth of periurethral glands and stroma. The hyperplasia most often involves the lateral and median lobes.
Future pathologists: Look for expanded glands, often with papillary infoldings, and dense, stroma. The low-power view proves that the overall architecture of the gland is preserved. All about the histopathology: Urol. Clin. N.A. 17: 477, 1990.
There may be a preponderance of glandular hyperplasia, a preponderance of stromal hyperplasia, or some of both.
* "Sclerosing adenosis", a fooler for cancer, has true myoepithlium (S100 +, muscle-actin +), unlike cancer or common hyperplasia.
We actually don't think you should diagnose prostate hyperplasia on needle biopsy. There's no real correlation between what the pathologist sees and the patient's symptoms / signs (Hum. Path 33: 796, 2002).
The site where the hyperplasia arises ("the transition zone") is well-characterized (Urol. Clin. N.A. 17: 477, 1990).
By contrast, "the posterior lobe is the most common site for the development of prostatic adenocarcinoma". (* Do you think that this might simply reflect the fact that cancers here are easier to detect early?)
Median lobe hyperplasia by itself produces a "median bar" (today, a "midline dorsal nodule"), obstruction without an enlarged gland. Don't be fooled.
The etiology of prostatic hyperplasia is obscure. It clearly has something to do with sex hormones and their receptors. Remember that the stromal cells turn testosterone to the dehydro form that is what works on the secretory cells. The one clear risk factor is overweight / obesity (J. Urol. 189 S1: S102, 2013). Heroic abstinence (see above) is also a risk factor, although probably for everybody else there's little protection from more-frequent ejaculation (Urology 61: 348, 2003).
The most interesting work focuses on various proteins produced by the stroma that cause hyperlasia of glands, and proteins produced by glands that cause hyperplasia of the stroma. Long-studied, there are updates in J. Urol. 172: 1784, 2004 and Endocrinology 146: 13, 2005.
There's a mouse model -- a transgenic mouse with its int-2 proto-oncogene (fibroblast growth factor #3) revved up. It shows the same androgen dependency as do old men's prostates (J. Urol. 149: 633, 1993).
* Cell culture researchers talk about mysterious interactions between epithelium and stroma (J. Clin. End. Metab. 83: 206, 1998.
Prostatic hyperplasia causes many problems (collectively called "prostatism"), though most patients are asymptomatic.
The treatment is surgical -- one favorite procedure is trans-urethral resection (TURP), or try the laser approach (J. Urol. 154: 174, 1995; J. Urol. 184: 2023, 2010) or the newer cryosurgery or microwave techniques (pathology of cooked prostate: J. Urol. 171: 672, 2004; also J. Urol. 170: 12, 2003).
I still think I'd opt for surgery rather than some of the new hormonal manipulations. Patients treated with 5-alpha reductase inhibitors (i.e., finesteride) tend to get atrophy of the glands and some squamous metaplasia, but it is not spectacular. The much-promoted saw palmetto fails a controlled study miserably: J. Urol. 171: 284, 2004; another failure NEJM 354: 557, 2006; yet another JAMA 306: 1344, 2011; Cochrane Database 12:CD001423, 2012.
{10743} prostate hyperplasia, gross. Don't try this paper clip trick at home.
{17007} prostate hyperplasia, gross cut surface
{15382} prostate hyperplasia, gross; both gland and bladder have been opened anteriorly
{18766} prostate hyperplasia, gross
{24445} prostate hyperplasia, gross
{17458} prostate hyperplasia, good median bar
{08856} prostate hyperplasia, histology
{17457} prostate hyperplasia, histology
{17197} prostate hyperplasia, histology
{08857} prostate hyperplasia, histology
|
Australian Pathology Museum High-tech gross photos
|
|
|
| PROSTATE CANCER: Adenocarcinoma of the subcapsular glands. All about the pathology: Cancer 70(S1): 235, 1992; Cancer 71(S3): 906, 1993 (deja vu); changes after therapy Arch. Path. Lab. Med. 131: 360, 2007; review of the disease Br. Med. J. 308: 780, 1994; Sci. Am. 279(6): 74, Dec. 1998. |  Frank Zappa |
Prostate cancer is the commonest cancer in men, and the second leading cancer killer of men. There are around 233,000 new cases in the US yearly, and 29,480 deaths (i.e., it's now our most common men's cancer, but most of these men die of something else; see Lancet 1: 799, 1989).
This doesn't include LATENT PROSTATE CANCER (i.e., you found it only at autopsy, and it caused no problems), and probably not all cases of INCIDENTAL PROSTATE CANCER (i.e., you found it on the turp chips). OCCULT PROSTATE CANCER might pop up in bone marrow or lymph node prior to becoming symptomatic.
The tremendous increase in the incidence of prostate cancer during the 1990's (about 30%) reflects the improved screening. A man's lifetime risk of dying of the disease is actually decreasing.
On May 22, 2012, the US Preventive Services Task Force decided that the benefits of PSA prostate screening did not outweigh the harms; the urologists were outraged and most physicians are continuing screening (Lancet 379: 2024, 2012). The internists are now looking at higher decision levels (Ann. Int. Med. 158: 145, 2013); how the percentage of "free PSA" (high tends to mean benign) will impact this is also up for study.
The in-situ lesion (formerly "prostatic dysplasia", now "prostatic intra-epithelial neoplasia") was well-characterized during the early 1990's (J. Urol. 149: 170, 1993; Am. J. Cln. Path. 96: 628, 1991). There's always nuclear enlargement and crowding, there are usually nucleoli and some piling-up, and the nuclei are more hyperchromatic as the grade increases. But there is no invasion or architectural distortion. Low-grade "PIN" is common in young men (J. Clin. Path. 42: 383, 1989; J. Urol. 150: 379, 1993), and it probably takes decades to transform; most pathologists simply don't report it even if they see it, and today's wisdom is that this is the correct thing to do (J. Urol. 166: 402, 2001). The high-grade kind, distinguished by prominent nucleoli, is much wickeder: J. Urol. 158: 12, 1997.
* Much of the work on this lesion was done by former Mayo pathologist Dave Bostwick MD; I was his "path resident" when he was a med student in 1978. I'm proud of you, Dave!
Nobody knows yet exactly what to do when you discover PROSTATIC INTRAEPITHELIAL NEOPLASIA ("carcinoma in situ" or whatever; update Arch. Path. Lab. Med. 131: 1257, 2007; pathologists see also J. Clin. Path. 60: 856, 2007). Usually these lesions will involve part of a single sample. Nowadays, the feeling is that PIN3 requires re-biopsy. Of course, we are going to assume that we are not simply looking at an aggressive cancer spreading down the ducts, which can look identical. Here's how to make the call:
PIN3: As PIN2, but with prominent nucleoli and a papillary or cribriform pattern. Today, the tendency is to call any PIN with ugly nuclei "high-grade PIN" and merely subdivide into "tufting", "micropapillary", "cribriform", or "flat", or not bother subdividing.
Any: The basal cell layer is at least somewhat intact. (It is NEVER intact in true adenocarcinoma). Racemase / AMACR / P504S is very often (some say almost always) positive in PIN.
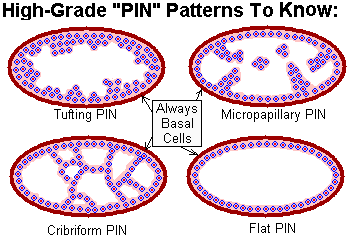
* Future pathologists beware: "Adenomatous hyperplasia" is an mass of crowded glands, but without any nuclear abnormalities. Best call it benign.
* Future pathologists only: Intraductal carcinoma of the prostate is very anaplastic carcinoma-in-situ; there's usually invasive anaplastic carcinoma nearby (Arch. Path. Lab. Med. 136: 418, 2012).
* Worth knowing: Gene stains are just appearing for prostate cancer to make the tough calls easier. Lighting up ERG, the gene often involved in rearrangements in prostate cancer, is very specific for invasive adenocarcinoma of prostate origin, and positive in 50%: Arch. Path. Lab. Med. 136: 935, 2012.
Prostate cancer is mostly a disease of men over age 50.
Prostate cancer is rare in Oriental folks in Asia, more common in Asian-Americans, common in U.S. whites, and most common in U.S. Blacks.
The majority, but not all, prostate cancers supposedly arise in the posterior lobe. Again, I wonder whether this merely reflects how much easier these are to detect on rectal exam.
In classic studies, serial sections of prostates at autopsy show little adenocarcinomas in 10% or so of US 50-year-old men and nearly 100% of 100-year-old men. The most recent stuff is about the same (1 in 3 of men in their sixties, about of half of men in their seventies: J. Urol. 179: 892, 2008). Most are "occult", however. Today, some urologists will do "active surveillance" (see below) for small, low-Gleason cancers. Update J. Urol. 178: 833, 2007).
Grade and volume determine metastatic potential. Surprised? Of course not. And if the gland is clinically benign, the rate of metastasis seems to be extremely low (or maybe even zero, Arch. Path. Lab. Med. 119: 731, 1995).
* How many turp chips should the pathologist check? Most pathologists probably submit all the chips if they weigh in aggregate 30 gm or less; at least one cassette for every 5 grams if more.
The etiology of prostate cancer is essentially unknown.
Androgens play some role; early castration prevents the development of adenocarcinoma (* not worth it, though....)
There is probably no link to infection or prostatic hyperplasia, or to frequency of of sexual activity. For some reason this was re-examined recently and the conventional wisdom stands. Frequency of ejaculation does not seem to have any impact (good or bad) on risk for prostate cancer (JAMA 291: 1578, 2004).
Industrial exposure to cadmium (i.e., battery factories) is supposedly linked to increased prostate cancer. (Everything bad about cadmium: Nature 361: 369, 1993.) The link strongly disputed: J. Tox. 6: 227, 2003; J. Occ. Env. Med. 43: 593, 2001; the animal model isn't striking Prostate 46: 11, 2001); today most regulatory agencies don't classify it as a carcinogen.
* A single major study links Agent Orange exposure in Vietnam to earlier and more aggressive prostate cancers. Watch this one: Cancer 113: 2464, 2008; Cancer 119: 2399, 2013 (still confusing). An earlier study showed no link (J. Urol. 166: 100, 2001).
* Your lecturer suspects the old alleged "link" between vasectomy and prostate cancer simply reflects the fact that men who get vasectomies go to the doctor more often, and get their prostates checked more often. (See JAMA 269: 913, 1993). Nothing more in the ensuing two decades.
The folks at the JAMA seem to consider the protective effects of tomatoes to be established (JAMA 300: 33, 2008; from Mizzou); the question is now, "which molecules(s)?" However, selenium and vitamin E, alone or in combination, totally flopped as prostate cancer prevention in an enormous study (JAMA 301: 39, 2009).
There is a decades-old hoopla over high-fat / meat diet as a very important risk factor for cancer of the prostate (already old-news Ann. Int. Med. 118: 793, 1993; update J. Urol. 171: S-19, 2004). Your lecturer does not believe it. You decide.
You remember the same claim about breast cancer in the 1980's; it was another claim that turned out to be clearly false.
A huge study about carotenes, lycopenoids, etc., etc. and prostate cancer turned up no correlation with overall risk with some possible weak favorable correlations suggesting protection against advanced disease (lots of warnings against inferring cause and effect: Am. J. Clin. Nutr. 86: 672, 2007).
* Not so long ago there was a flap about milk consumption as being a risk factor. The studies that followed were amazingly inconsistent (skim milk appears more dangerous than whole milk: Int. J. Cancer 73: 634, 1997; no no, it's the animal fat that's dangerous Br. J. Cancer 80: 107, 1999; no it's the calcium and the effect is very small: Am. J. Clin. Nutr. 74: 549, 2001; very weak link Int. J. Cancer 80: 704, 1999). I can't really take this seriously when there so many confounding variables, known and unknown. As you probably know, in 2000, PETA published a parody-ad of Rudolf Giuliani (who has prostate cancer) with a "milk moustache" and the legend "Got Cancer?" PETA was retaliating against Giuliani after losing a lawsuit against him and the City of New York when they forbade PETA to do street theater to protest Cow Parade. I am not making this up. I am bringing it to your attention because this is the rubbish that is shaping your patients' beliefs about health.
The link between new prostate cancers and smoking is weak if it exists at all (there's been basically nothing for well over a decade).
* Acute and chronic prostatitis seem to protect from prostate cancer -- if present on initial biopsy, the patient has less risk long-term. Or maybe people with prostatitis but no sign of prostate cancer just are more likely to get biopsied: Cancer 120: 190, 2014.
BRCA1 (maybe) and BRCA2 (probably) mutations increase a man's risk some (maybe 2x / or get it younger), though "Big Robbins's" claim of a 20-fold increase from BRCA2 is an error.
* The best-studied prostate cancer gene is HPC1 / RNASEL, where a single nucleotide substitution increases risk but apparently not aggressiveness (J. Urol. 179: 1344, 2008). There is another prostate-cancer-family gene: HPC2 / ELAC2; curiously, it gives only about double the normal risk. The same's true of each of five newly-identified loci (NEJM 358: 910, 2008); the one that you WILL hear about is ERG-fusion ("TMPRSS2-ERG fusion", present in a good majority of prostate cancers and a marker for aggressiveness. It is coming into use as a specific stain for invasive or almost-invasive prostate cancer -- discovered Am. J. Surg. Path. 31: 882, 2007; Mod. Pathol. 21: 67, 2008; Clin. Canc. Res. 14: 3380,2008; there are types A and C; checking little cancers for it is now commonplace J. Urol. 185: 489, 2011; the stain is highly sensitive and specific for the rearrangement Am. J. Clin. Path. 138: 803, 2012.
* Hypermethylatin of glutathions S-transferase (GSPT1) is a robust finding in many of these tumors (JNCI 93: 1671, 2001).
* Other molecular signatures that actually matter to the prognosis or easy diagnosis remain elusive (J. Clin. Path. 58: 67, 2005). The first to be dsicovered that is typcially overexpressed in prostate cancer regardless of grade, and not in benign prostate lesions, is PAX2 (J. Urol. 165: 2115, 2001). Expression of survivin, an apoptosis inhibitor, seems to predict poor prognosis: J. Urol. 171: 18855, 2004. HOXB13 has an uncommon germline mutation that produces an autosomal-dominant prostate cancer family syndrome (NEJM 366: 141, 2012). The tumor loses its androgen sensitivity when (Nowell's law!) the androgen receptor gene mutates (no surprise, NEJM 332: 1440, 1995).
* Mutations indicating a more aggressive prognosis are starting to be noticed but are not in use yet. See Am. J. Path. 181: 1585, 2012.
* Not surprisingly, the high-grade cancers tend to stain for telomerase and the low-grade ones don't (why?; Cancer 95: 2487, 2002).
* Let us worry about the uncommon types of prostate cancer A few prostate cancers are "ductal" (papillary with pseudostratified epithelium; formerly "endometrioid from the verumontanum") rather than the usual "acinar" type; not everyone believes in it. Update Mod. Path. 17: 316, 2004. Leave the diagnosis of prostatic stromal tumors (benign, malignant, and the infamous STUMP -- stromal tumor of uncertain malignant potential) up to us (Br. J. Rad. 84: e194, 2011; AJR 200: W571, 2013).
Cancer of the prostate presents as a painless lump in the gland.
These tumors are easier to feel than to see; they are firmer than hyperplastic nodules, poorly circumscribed, and yellowish.
Diagnosis is by biopsy or fine-needle aspiration. Or it may turn up in a routine prostatectomy specimen. (If you're going to operate for obstruction anyway, there's no reason to biopsy first.)
Future pathologists: With all these guys getting needle biopsies nowadays, you need to try to find tiny cancers. You must section several levels of the core biopsy (Am. J. Clin. Path. 107: 26, 1997; Arch. Path. Lab. Med. 122: 833, 1998).
The mere finding of a prostate cancer does not promise surgery. If the Gleason is 6 or less, PSA level less that 0.15 ng/mL, no more than two positive cores out of twelve, and no more than 50% involvement of any core -- we do "active surveillance" (i.e., nothing -- J. Urol. 186: 470, 2011; update J. Urol. 190: 2033, 2013) Probably these cancers (i.e., those without any pattern 4 or pattern 5) are incapable of metastasizing (Am. J. Surg. Path. 36: 1346, 2012). And while grade 9-10 is ominous, some of these people have good outcomes from surgery (J. Urol. 190: 2068, 2013).
Prostate biopsies are tiny. In around 5% of them, the pathologist is likely to ask for re-biopsy. Arch. Path. Lab. Med. 123: 687, 1995. Help with your tough calls: Arch. Path. Lab. Med. 124: 98, 2000. Recently, the trend has been to get lots of cores; ten is now commonplace and twenty may become standard (J. Urol. 179: 504, 2008). And by the way... the more prostate biopsies you get (at least if you're being followed for a known cancer by "active surveillance"), the more likely you are to get erectile dysfunction (J. Urol. 182: 2664, 2009; disputed J. Urol. 188: 1252, 2012). Plus, they hurt badly and are prone to get infected, especially in low-volume centers (BMJ 344: d7894, 2012).
"Vanishing carcinoma phenomenom": A biopsy shows cancer, the prostate gland is resected, and there's no cancer. The patient and surgeon are NOT happy. Most of the time, if you section the entire gland, you can find a tiny focus which makes everybody happy (Arch. Path. Lab. Med. 135: 1466, 2011).
When given a metastasis from a suspected primary, the pathologist stains for prostatic acid phosphatase and/or prostate-specific antigen -- both are highly sensitive and specific for prostatic origin.
Almost all are "prostate type" adenocarcinomas. (I find the traditional distinction between "large duct" and "small acinar" to be less-than-helpful.) To diagnose prostate cancer, you want to see one or more of the following:
* Nuclei with sharp angles, and cytoplasm with vacuoles, suggests that your "worrisome single-layered" acinus is benign basal cells, with the secretory cells gone from atrophy.
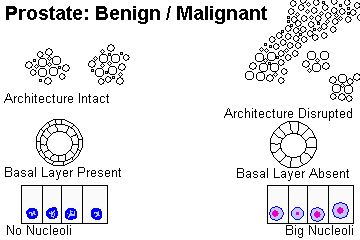
Some cases in which you see an isolated small acinus cannot be resolved and should probably be called "atypical small acinar proliferation suspicious for malignancy". This is NEVER a final diagnosis, but means, "We can't definitively say that the biopsy shows cancer." (There was maybe only one or two glands. It could be sclerosing adenosis. It could be high-grade PIN. It was really tiny and we think it's atrophy but we can't rule out the "atrophic" version of prostate cancer. It could inflammation with reactive change. Biopsy can produce artifact especially along the edges. We made a deeper cut to do immunochemistry and the little lesion was gone. Basal layer was gone but the cells looked benign. And so forth.) Nowadays, this diagnosis is followed, more often than not, by frank cancer (Arch. Path. Lab. Med. 130: 952, 2006 by Dave Bostwick; also Am. J. Clin. Path. 128: 648, 2007).
Update on "current prostate biopsy interpretation": Arch. Path. Lab. Med. 130: 835, 2006; the immunostains Am. J. Clin. Path. 123: 231, 2005; combining three Am. J. Clin. Path. 127: 248, 2007.
* ERG is a new stain for malignant prostate acini that's perhaps suitable as a bakcup: Arch. Path. Lab. Med. 136: 935, 2012.
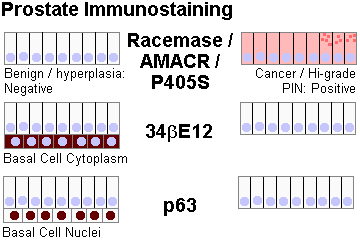
* On fine needle aspiration biopsy, pathologists pay special attention to the presence or absence of the basal layer, which conveniently will lie in its own plane of focus.
|
|
Grade correlates with stage and prognosis. Most prostate cancers, even the ones that have metastasized, are fairly well-differentiated adenocarcinomas.
Gleason sums 2, 3 & 4 usually don't produce palpable masses or raise PSA and are very uncommon on needle biopsies; usually they show up in prostate resected for benign disease.
* Biomarkers (microarray technology -- i.e., which genes are activated?): Nature 412: 822, 2001; Cancer 104: 209, 2005. Genetics update, especially about signature translocations (mostly involving ERG) plus androgen-dependence and its loss: Arch. Path. Lab. Med. 133: 1033, 2009. Amplified STAT5A/B: Am. J. Path. 182: 2264, 2013. The Sprouty2 / PTEN / PP2A pathway in animals and people: J. Clin. Inv. 123: 1157, 2013.
* One surprise (from Walter Reed) is that if there is a single focus of cancer in a prostatectomy specimen, the prognosis is worse than if there are several foci, all other things being equal. Think why that might be (J. Urol. 182: 2689, 2009).
* Staging of course also affects prognosis.
For the TNM system --
Tx: occult tumor
T1: not palpable, within prostate
T2: palpable, within prostate
T3: through the capsule
T4: fixed or invades something other than the seminal vesicles
Nx: nodes not assessed
N0: no nodes
N1: one positive node, 2 cm or less
N2: no node 5 cm or larger
N3: some node 5 cm or larger
Mx: metastases not assessed
M0: no distant metastases
M1: distant metastases
More familiar:
A1: well-differentiated carcinoma on 5 or fewer turp chips / fewer than 3 foci / fewer than 5% of the chip mass (rules vary).
A2: still occult, but on more than 5 chips or high-grade
B: palpable nodule
C: through the "capsule" or in the seminal vesicles
D: metastases
Before you decide you can tell benign from malignant reliably on physical exam, note that even a pathologist with the sectioned gland in his/her hand prior to microscopy is only 2/3 sensitive and 5/6 specific (Am. J. Clin. Path. 110: 38, 1998).
* Uncommon prostate adenocarcinomas include squamous and large-duct (the former "endometrioid"), plus adenoid-cystic, colloid, carcinosarcoma, signet-ring, oat-cell, carcinoid, and lymphoepithelioma. All but the most anaplastic express PSA. Again, let us worry about them.
Cancer of the prostate seldom causes problems (or is diagnosed) unless it spreads.
Rectal exam is still the most effective method of diagnosis (cost per life saved a mere $6300; see JAMA 252: 3261, 1984).
For more on "prostate specific antigen", see the upcoming lecture on cancer screening and monitoring. Nowadays, urologists are likely to do sextant biopsies on prostates of men with elevated PSA's and no palpable lump.
Prostate cancer is often indolent even when it has metastasized, but some prostate cancers are very aggressive.
* Mucin-producing prostate cancer is an aggressive lesion with its own molecular signature; it is probably a different disease (J. Urol. 54: 141, 1999).
* Finasteride has been offered for prostate cancer prophylaxis (NEJM 349: 205, 2003). On the plus side, there was a few percent fewer cases of low-grade prostate cancer. On the minus side, there was no change in the rate of high-grade prostate cancers or cancer deaths. You'll have to decide for yourself whether the effects of taking finasteride at these doses (fewer and softer erections, diminished seminal fluid volume, loss of chest hair, preservation of scalp hair) are good or bad. Follow-up: NEJM 369: 603, 2013 -- actually the finasteride folks got MORE of the high-grade cancers, but neither group did better than the other on mortality or morbidity.
You will care for many patients with metastatic prostate cancer.
Prostate cancer typically metastasizes to the axial skeleton (there's a direct connection between the prostate and the valveless venous plexus that surrounds the inside of the spinal column), eventually causing miserable bone pain. (Future radiologists: prostatic metastases are often osteoblastic.)
Prostate cancer seldom produces actual brain metastases, but is also infamous for metastasizing to the meninges.
{17012} prostate cancer in bone, x-ray
Serum acid phosphatase (* tartrate inhibited) is a classic tumor marker for prostate cancer (see JAMA 253: 665, 1985). The best new tests measure only the prostatic component.
Treating prostate cancer:
Surgery and/or radiation are useful for localized disease. Conventional chemotherapy is of limited usefulness in prostate cancer, but protocols do exist.
* Robotic-assisted prostatectomy: J. Urol. 186: 511, 2011.
* "Among men with localized prostate cancer detected during the early era of PSA testing, radical prostatectomy did not significantly reduce all-cause or prostate-cancer mortality, as compared with observation, through at least 12 years of follow-up. Absolute differences were less than 3 percentage points." NEJM 367: 203, 2012. I think most pathologists were not surprised.
Prostate cancer is usually quite responsive to endocrine manipulations.
Castration (orchiectomy -- still works well for patients willing to undergo it) and/or estrogen therapy (causes cardiovascular problems) were for many years the standard treatments for patients with symptomatic bony metastases. Now they are being replaced with newer agents.
One important new agent is leuprolide, a GnRH (gonadotropin releasing hormone) agonist.
* When large amounts of leuprolide are present for a while, the pituitary stops making GnRH receptors and thus stops making gonadotropins. (Seems paradoxical, doesn't it?) The patient soon has stopped making androgens, and the prostate cancer cells undergo apoptosis.
* The histopathology of leuprolide response is sufficiently distinctive to be recognizable by a good pathologist: Cancer 73: 1472, 1994.
* Another approach is the non-steroidal anti-androgen Flutamide, which shrinks prostate cancer supposedly "without causing impotence". Post-castration with recurrent or unresponsive disease, the androgen synthesis blocker abiraterone seems to help (NEJM 364: 1995, 2011). The anti-fungal agent ketoconazole blocks synthesis of androgens and has also proved useful as an anti-prostatic cancer drug.
* Future oncologists: Etidronate treatment for refractory bone pain -- it seems to work by preventing formation of new bone.
* Vitamin D3 supplementation (4000 IU/day) for low-risk prostate cancer is reported to reduce the number of positive cores on repeat biopsy; it just might be true (vitamin D deficiency is common & it's a steroid): J. Clin. Endo. Metab. 97: 2315, 2012. Mouse model too: Endocrinology 153: 2576, 2012.
* As far back as the 1990's, despite the focus on early detection, we knew that low-grade, low-stage prostate cancer, treated very conservatively, didn't seem to shorten life expectancy (JAMA 274: 626, 1995).
Nowadays, of course, you can follow the course of treated prostate cancer with serum prostate specific antigen, the same stuff as you use for screening: Mayo Clin. Proc. 69: 69, 1994.
To date, no one has produced any "evidence-based" support for any of a host of "alternative and complementary" remedies for prostate cancer (Urol. Clin. N.A. 33: 237, 2006).
|
|
LOOKING AT PROSTATE BIOPSIES:
| Benign | Malignant | |
| Low magnification? | Architecture intact | Architecture disrupted |
| Basal layer? | Present (at least discontinuously) in benign lesions and precancers | Usually absent |
| Nuclei? | Normal-size | Often big; hyperchromatic in high grades |
| Nucleoli? | Inconspicuous (prominent in some precancers) | Often big and red |
| Chromatin pattern? | Normal | Often marginated (i.e., mostly at edge of nucleus) |
| Secretion? | Pale, not basophilic | Often basophilic |
| Crystals in the lumens? | Almost never | Sometimes |
| Cribriform pattern ("swiss cheese")? | Certain areas of normal prostate and certain precancers | Gleason III cancers |
| Perineural "invasion"? | Almost never | May be present |
| Invasion? | No | Look for indian files |
| 34βE12 | Shows basal cells present Positive in tumor itself: Benign |
Shows basal cells absent or at least disrupted |
| P504S / AMACAR / racemase? | Cytoplasm negative | Cytoplasm often positive |
| Nuclear p63 stain / K903 stain | Often positive (basal layer) | Usually negative |
A FEW ADDITIONAL IDEAS:
There is no difference between a wise man and a fool when they fall in love.
-- Traditional
Despite "conventional wisdom", impotence is often organic, even in younger men without obvious disease. Ask the guy if he gets erections out of bed, or try the famous low-tech "postage-stamp coil" test. In Portugal, not known for being wild, the doctors have developed a "visual erotic stimulation test" that they concluded will give an erection to any guy not organically impotent (J. Urol. 157: 134, 1997). Even tiny prolactinomas are notorious anti-aphrodisiacs. See JAMA 249: 1736, 1983. Did you check for hemochromatosis? Injection therapy (phentolamine, prostaglandin E1, papaverine) for the guy to use when he wants an erection: Arch. Phys. Med. Rehab. 75: 276, 1994. Viagra: Too many articles to count, all in 1998. Watch for cabergoline therapy (anti-prolactin) to increase male libido. Blunt trauma to the shaft during masturbation or intercourse can crack the side of the dorsal vein, allowing blood to drain in easily and causing impotence. How to fix it: J. Urol. 148: 1171, 1992. Update on injuries during romance: J. Trauma 62: 1522, 2007.
For premature ejaculation, if the guy doesn't get good results from the squeeze technique (which is fun), try a selective serotonin reuptake inhibitor (Am. J. Psych. 151: 1377, 1994; dudes: these'll improve an anal-retentive outlook on life, too). Some men cannot ejaculate; for the electronic gadget that helps, see J. Urol. 152: 1034, 1994. Retrograde ejaculation results from failure of one of those little bands of muscle to relax; ask about whether he's taking thioridazine, or an anatomic cause (J. Urol. 151: 1017, 1994).
Viscerosomatic reflex: Very rapid overfilling of the prostate and seminal vesicles (i.e., prolonged arousal without ejaculation in a young male) results in pain referred to the testes that can be severe ("blue balls", "lovers' nuts", etc.) The cure is ejaculation by any means. Your instructor suspects the mechanism is pressure of the overfilled seminal vesicles on the genitofemoral nerves and maybe veins.
Junk science! Hey dudes, are we being un-masculinized by rampant estrogen pollution (diethylstilbestrol cattle-fattener, women's oral contraceptive pill components excreted unchanged, other substances)? In a widely-publicized paper, researchers presented evidence that the average sperm count has declined by half over the 1900's (Lancet 341: 1392, 1993, totally unconvincing graph Science 265: 308, 1994). This was based on a handful of determinations of "average sperm counts" from before 1970 compared to today. There has been no drop since 1970. There is exactly no evidence that male infertility is increasing: NEJM 332: 327, 1995. So far there's a single claim, from Finland (Br. Med. J. 314: 13, 1997) that testicular histology has changed. (Anybody noticed a decrease in testicular size? I don't think so....) The most recent studies have failed to show an effect, or shown the counts to be increasing with time, or shown how inaccurate sperm-counting must be (i.e., New Yorkers counted in the New York lab averaged exactly twice the counts for Angelinos counted in the L.A. lab; Br. Med. J. 312: 1183, 1996). And if un-masculinization were really at work, your lecturer believes we modern men would have less body hair, less baldness, less B.O., and less belligerence. Nuh-uh! Your lecturer thinks that modern-day dudes simply ejaculate more often (you can figure out why yourself, and this has been confirmed in interviews) and resorb less fluid between ejaculations, concentrating the sperms less. Alternatively, today's man stays excited longer beforehand, producing more fluid. Every teenaged guy knows about this stuff, but the authors of the original paper apparently didn't think of this; I called them on it immediately, and the NEJM article above thought that "duration of abstinence" was probably the explanation too. After this paper, there was a silly media hype, and an inflammatory best-seller ("Our Stolen Future"). A Greenpeace poster of a man with a tiny penis proclaiming "You're not half the man your father was" (the campaign is over and the claim has disappeared from the Greenpeace website by 2008, no "sorry about the mistake / sorry we lied" though). There was an even sillier discussion on the floor of the U.S. senate. The most obvious source of substantial xeno-estrogen exposure is soybeans. Have you heard of any "socially-conscious environmentalists" calling for a ban on tofu? Of course not.
* Some men have had accidents. See J. Emerg. Med. 8: 305, 1990 (caught in the zipper), Acta. Urol. Jap. 34: 514, 1988 abstract 88267069 (caught in a milk bottle for seventeen hours), J. Urol. 170: 2385, 2003 (hard-to-cut plastic bottle finally yields to a stryker cast saw); J. Urol. 147: 1265, 1992 (all about bites, come in early if it happens to you, dude, 'cause infections can be really bad), J. Urol. 133: 1046, 1985 (etiology of "sclerosing lipogranuloma", you would enjoy reading this one), guy electrocutes himself while attaching the second electrode to his penis (the first was in back -- AJFMP 19: 198, 1998); Plast. Rec. Surg. 91: 352, 1993 (review of sclerosing granuloma, with a case study of a guy who injected himself with transmission oil in the hopes of having a permanent erection; bad idea, fellow); J. Urol. 134: 274, 1985 & Br. J. Surg. 89: 555, 2002 (fractures of the erect penis), J. Trauma 56: 1138, 2004 (by far the most common cause of fracture is striking the female pubic bone too forcefully); Urology 24: 18, 1984 (rings), Plast. Rec. Surg. 87: 771, 1991 (electrical injury), J. Emerg. Med. 8: 419, 1990 (young skateboarder impales scrotum on a metal rod), Br. Med. J. 281: 26, 1980; Br. Med. J. 281: 591, 1980; JAMA 224: 630, 1973; Urology 25: 41, 1985 & Indiana Med. 81: 252, 1988 (vacuum cleaners; there are several other articles on the same subject), Urology 26: 12, 1985 (foreign bodies), Urology 26: 50, 1985 (pet rattlesnake), J. Urol. 153: 1929, 1995 (alligator, reconstructed after 20 years and it worked), Br. J. Urology 74: 121, 1994 (pig), Plast. Recon. Surg. 108: 805, 2001 (another pig), Urology 26: 81, 1985 (necklace), Am. J. For. Med. Path. 7: 254, 1986 ("Eddie Spaghetti"), Genit. Med. 68: 334, 1992 (penicillin bottle under an enormous foreskin), electric cable, paper clip, tweezers, etc., (Br. J. Urol. 68: 510, 1991), J. Roy. Soc. Med. 98: 122, 2005 (magnet and metal); Arch. Sex. Behav. 34: 469, 2005 (bottles); Int. Ur. Neph. 25: 77, 1993 (uses high-tech term "SFB" for self-inserted foreign body), guy self-injecting olive oil into his scrotum to make it bigger gets fat embolus (Chest 107: 875, 1995), romantic love between a man and his hydraulic tractor ends in death (J. For. Sci. 38: 359, 1993), Med. Asp. Hum. Sex. July 1991 (guy in love with a sander belt loses a testis and repairs himself on-the-job with his handy staple gun; much-photocopied). Two guys mutilate their genitals elaborately while high on amphetamines (Addiction 97: 1215, 2002); both said it was extremely pleasurable at the time and both continued the drug use and the self-mutilation. There's no figuring drug-users out. A man gets it caught in a bottle and eventually dies of gangrene because he is too embarrassed or whatever to tell anyone (Am. J. For. Med. Path. 32: 344, 2011). Huge review of gunshot wounds: J. Trauma 64: 1038, 2008. "Alcock syndrome" is insensitivity of the penis (lasting up to several weeks) resulting from pressure on the pudendal nerve (which runs through "Alcock's canal") during bicycling. Mishap with the laser: Urology 48: 155, 1996. Caught in the zipper? See Injury 25: 59, 1994 -- easy to manage. Complications of penis-piercing, now become popular in the US: Cutis 60: 237, 1997. A "cultural practice" in some Asian communities is attempting suicide by cutting off the penis and bleeding to death (Am. J. Psych. 150: 350, 1993). Even less amusing: In past wars, when a captured man was being tortured either for information or fun, mutilating the genitals was commonplace. This was fairly common as recently as the Vietnam era (both sides), and surfaced again in Bosnia. Sexual torture: Lancet 345: 1307, 1995. Injury to the vas deferens from torture: Br. J. Urol. 72: 515, 1993. In "the new South Africa", the phenomenon of "Muti killing" has emerged in which body parts are excised from victims while they are still alive in the belief that these can be used to cure diseases such as AIDS (Med. Sci. Law 46: 255, 2006); boys are likely to have the genitals cut off. Sexual abuse of a child in any form is one of the vilest and most disgusting things a person can do. We hear mostly about fondling (which does no physical damage but is supposed to lead to terrible lifelong emotional scarring). The GAO's 1996 review of whether children who get molested go on to become child molesters themselves and documented the difficulty of studying this scientifically -- the prospective studies would lead most readers to conclude that it really very seldom happens. However, boys who are abused sexually often have severe physical damage in addition / instead (burns, cuts, crush injuries; Arch. Dis. Child. 92: 328, 2007 acknowledges that nobody's paid attention -- the politics is so bizarre). Reconstructing a youngster's penis using microsurgery, so that it works: J. Urol. 149: 1521, 1993. A grown-up's amputated penis is re-attached and still works: J. Urol. 147: 1628, 1992. Another Arch. Sex. Behav. 19: 343, 1990. We await publication of the full details of John Wayne B....
A penis that, when stretched to its maximum flaccid length (which is pretty much the same as its fully-erect length), is shorter than 2 SD below the mean for the guy's age is an official "micropenis". For a grown man:
11 cm: 10th percentile
13 cm: 50th percentile
15 cm: 90th percentile.
Lots of guys have some curvature, most often upwards, often downwards, sometimes a little to one side or the other (J. Sex. Marit. Ther. 23: 195, 1997).
* Agenesis of the penis: J. Urol. 143: 338, 1990. Two of them (diphallus): J. Urol. 142: 356, 1989.
* Your lecturer predicts male circumcision will remain popular for newborns,
as well as a popular choice for older males.
It has long been politically incorrect
for pediatricians to recommend routine circumcision of newborns,
despite the obvious health benefits for some groups.
In 1999,
the American Academy of Pediatrics issued a new statement affirming that
there are real health benefits, but not enough to make the right
choice obvious, and of course asking
that an anesthetic be used (Pediatrics 103: 686, 1999).
Circumcision in infancy
prevents cancer of the penis very effectively, and it greatly (10 x, from 1 in 100 to 1 in 1000;
not "slightly",
as the AAP states) reduces urinary tract infections
in little boys (Pediatrics 83: 1011, 1989; good review, everything I've
seen since this
confirms this; most recent Lancet 352: 1813, 1998). Hygiene is much easier, the risk of catching
AIDS from a woman during normal lovemaking is much less (NEJM 319: 274, 1988,
Nat. Rev. Micro. 3: 914, 2005;
Urol. Clin. N.A. 22: 57, 1995, Sci. Am. 1996;
Lancet 369: 643, 2007;
Lancet 363: 1039, 2004 shows the risk is cut
by 5/6, though there's no comparable benefit for syphilis or gonorrhea),
the other common sexually transmitted
diseases are harder for him to catch (NEJM 322: 1308 & 1312, 1996;
STD's in general Pediatrics 118: 1917, 2006 -- curiously, no "political incorrectness" disclaimer;
HPV Lancet 369: 657, 2007; Br. Med. J. 334: 712, 2007;
prevents herpes 2, HPV and HIV but not syphilis NEJM 360: 1298, 2009;
dissenting prospective study J. Ped. 152: 383, 2008; today nobody seriously
doubts it protects from HIV transmission in the poor nations J. Urol. 183:
21, 2010), and what's more, many
people like it ("Mine looks streamlined, it's my pocket-rocket, yours looks dirty;" most women
prefer for that special man to be circumcised: Pediatrics 105: 620, 2000). An
uncircumcised man's glans is a bit more sensitive (i.e., more intense sensations, both pleasant and
unpleasant? less total time before ejaculation?; men who've been circumcised as adults have told me
about both).
In order to appease anti-circumcision militants, the AAP
included the unsubstantiated claim that circumcision reduces the man's pleasure
in its "Information for Parents." Of course the media spun the whole
position statement as "Circumcision is no longer recommended."
Opposition to circumcision deals with other issues
than physical health.
Opponents cite "unnatural", "a male's right to make the decisions affecting his own
body", "religious freedom", "problems of the uncircumcised are treatable" (except HIV and
gangrene, of course; the latter can happen to an unwashed little boy).
Sexuality is powerful, individual, and incomprehensible.
The truth is that any boy has a fair chance of growing up to be a man who
really likes having a foreskin and/or bitterly resents not having one.
And the latter's a real problem, much worse than having a few kidney scars
from an infection.
In the 1990's there was considerable
anti-circumcision activism among men across the Kinsey scale ("I will NEVER forgive my
parents for..."), though this is based on personal-freedom issues
rather than health issues.
Since we're comparing physical health and emotional satisfaction,
the right choice will never be "clear-cut" (ha ha).
Around the turn of the century, as it became more acceptable to criticize "indiginous practices",
the medical literature began to discuss
a terrible problem in the poor nations -- "traditional healers" who perform
circumcisions as a result
of which "not uncommonly, amputation occurs" (Ann.
Plast. Surg. 44: 311, 2000).
South Africa prosecutes one of these quacks for murder (Br. Med. J. 313:
647, 1996 -- "the [tribal] king complained that gross damage was being
done [by the prosecution] to a culture that was the pride of the nation.
His complaint was not upheld.").
Things do not seem to be improving in "The New South Africa": Curationis 27:
57, 2004; the "traditional society" is obviously subjecting the boys
to willful, cruel abuse -- continuing problem Soc. Sci. Med. 70: 729, 2010 (even
this far-left ultra-multiculturalist journal knows it's wrong).
The mohel may kiss the circumcision site (metzitzah b'peh) and transmit
herpes![]() (series
of eight cases from Israel; Pediatrics 114: e259, 2004; update MMWR 61: 405, 2012 -- two boys die in NYC alone
and there's a huge "religious freedom" hoopla; your lecturer believes that surgery is surgery
and the field needs to remain sterile).
By contrast, in the United States, the circumcision rate for newborns
has actually been increasing in all ethic groups except Native
Americans since 1988; it's around 70% in the Midwest
and Northeast, but less than 30% out West, and the more affluent and educated
the family, the more likely they are to have the son circumcised (J. Urol. 173:
978, 2005), even though third-parties are refusing to pay for it
(Urol. Clin. N.A. 31: 461, 2004; J. Urol. 170: 1533, 2003).
The fact that postnatal circumcision will be required for health reasons in almost
10% of boys, and is much more expensive, is now persuading third-party
payers to change their minds about neonatal circumcision (J. Urol. 175:
1111, 2006). The obvious protection that circumcision provides against acquiring and transmitting sexually-transmitted diseases
as an adult is leading to calls for the pediatrics organizations to reverse their politically-correct
decision not to recommend routine neonatal circumcision (Arch. Ped. Adol. Med. 164: 78, 2010).
Update on just how difficult it is to advise parents: Ped. Clin. M.A. 59: 977, 2012.
(series
of eight cases from Israel; Pediatrics 114: e259, 2004; update MMWR 61: 405, 2012 -- two boys die in NYC alone
and there's a huge "religious freedom" hoopla; your lecturer believes that surgery is surgery
and the field needs to remain sterile).
By contrast, in the United States, the circumcision rate for newborns
has actually been increasing in all ethic groups except Native
Americans since 1988; it's around 70% in the Midwest
and Northeast, but less than 30% out West, and the more affluent and educated
the family, the more likely they are to have the son circumcised (J. Urol. 173:
978, 2005), even though third-parties are refusing to pay for it
(Urol. Clin. N.A. 31: 461, 2004; J. Urol. 170: 1533, 2003).
The fact that postnatal circumcision will be required for health reasons in almost
10% of boys, and is much more expensive, is now persuading third-party
payers to change their minds about neonatal circumcision (J. Urol. 175:
1111, 2006). The obvious protection that circumcision provides against acquiring and transmitting sexually-transmitted diseases
as an adult is leading to calls for the pediatrics organizations to reverse their politically-correct
decision not to recommend routine neonatal circumcision (Arch. Ped. Adol. Med. 164: 78, 2010).
Update on just how difficult it is to advise parents: Ped. Clin. M.A. 59: 977, 2012.
* Men with endometriosis (I always believed in the coelomic metaplasia theory rather than the reverse menstruation theory, anyway): Eur. J. Surg. 158: 7, 1992; Am. J. Ob. Gyn. 165: 214, 1991, others.
* When men of my generation get old, we men might get hormone replacement, just as many women do. This is probably a good idea (NEJM 334: 707, 1996; Br. Med. J. 312: 859, 1996; Ann. NY Acad. Sci. 774: 128, 1995; update NEJM 350: 482, 2004; J. Clin. Endo. Metab. 96: 38, 2011.) DHEA (the miracle-claims "nutritional supplement" of 1997) flunks tests of its ability to produce psychological benefits: J. Clin. End. Metab. 82: 2363, 1997. No one knows how many men get hypogonadism as they get older, or what is physiological; many, probably most, men do not undergo "andropause" (BMJ 337: b352, 2009). Stay tuned on this. A study of the effects of testosterone supplementation on a selected group of low-testosterone men who were also loaded with coronary risk factors had to be stopped in 2010 because the test group had many more "coronary events" (NEJM 363: 109, 2010).
The British found no link between vasectomy and testicular cancer, prostate cancer, or any other of the common diseases for which they sought a connection: Br. Med. J. 304: 743, 1992. Surprised? Of course not. Full of disclaimers about insufficient duration, insufficient patient numbers, etc.

* Among adults, only ideologues won't recognize that sexual behavior (broadly defined) has many purposes (good, bad, indifferent) in addition to fertilization. As far as I know, all durable societies have decided that a stable, lifelong, committed, faithful relationship is by far the best setting for sex. (Margaret Mead was, of course, the victim of a hoax by some teenagers.) It is one thing to be compassionate and not get preachy with everybody who comes into your office. It is quite another to advocate attitudes and behaviors that will predictably lead people to harm themselves and others. (I see this as a problem today in the U.S.; you might disagree.) People think about sex a lot, and we know that making it a taboo subject or a big dreadful mystery is asking for trouble, just as having casual sex is always asking for trouble. The wise adult learns that setting limits is the key, and decides what limits to set. Not everyone does this. Further, it is easier (and better power-politics) to get up on a soap-box about sex than to try to understand it. As a physician you must at least do the latter. Male sexuality becomes a major concern for the pathologist when it leads to death (i.e., homicide, in which sex is usually a factor, suicide, in which sex is often a factor, and autoerotic asphyxia, which is not rare) or when it involves someone who does not, or cannot, consent. Almost every man realizes that to force himself on another person (employee, family member, date, stranger, child) is shameful, wrong, disgusting, and un-masculine. Most men also feel entitled to "get their loving", and for many men, self-esteem gets tied up with "getting it". Most bright men figure out early that self-control, though difficult, is muy macho. For some men, controlling the urge to act-out sexually (which can take various forms, some of them harmful for other people) is as hard as sticking to a weight-reduction diet (see especially Psych. Clin. N.A. 15: 675, 1992). Probably these men have a wiring problem, whatever else may have gone wrong, and a psychiatrist can help (swallow your pride, dude; major review Psych. Clin. N.A. 15: 703, 1992; clomipramine fixes up a compulsive flasher Am. J. Psych. 149: 843, 1992; fluoxetine cures a Peeping Tom: Am. J. Psych. 148: 950, 1991; naltrexone (the opioid antagonist popular for alcoholics, drug abusers, compulsive eaters, obsessive-compulsives, and impulse-control problems) now finds its use for sexual acting-out as well (J. Clin. Psych. 65: 982, 2004). there's behavioral ("beak the compulsion loop"), insight, and pharmacological ways of helping most problem guys, if they want to be helped, and for criminal-justice cases, there's now leuprolide, which works better than saltpeter). Perhaps the most interesting article on male sexuality that your lecturer has ever seen was a prison survey in which 23% of prisoners admitted to having been forcibly raped by a male bully, and those who could tell the interviewer about this without becoming visibly and acutely upset were almost all sex offenders. The conclusion is that at least a good number of sex offenders come to terms with what's happened to them by acting out "in a strange and cruel way" (Med. and Law 12: 181, 1993). There's gotta be a better way of making sense of what's happened to you; perhaps a family physician, talking sense and explaining "you're still a man", etc., etc. could have made all the difference. Since dominance relationships among humans are so complex, subtle, and important, all men and many women fantasize some about this being tied up with sexuality; this is part of the human condition, as much as we'd like all loving to be a full coming-together of equals. It is also very hard for a man to defend against a false accusation of rape (in spite of what you've been told by "women's advocates", this is all-too-common; remember the Bible tale of Potiphar's wife, Athens's Phaedra, Gail Crystal Mangum (Duke lacrosse case) or ask a cop, and the forensic pathologist / DNA work can make all the difference here. How the British police decide: Medicine Science & the Law 36: 135, 1996. Good police work and a sympathetic physician who remains kindly, helpful, and also totally objective can be a huge help in preventing situations in which everyone is a loser. A study at Purdue showed to my satisfaction that at least 40% of initial campus and community accusations are false (at least in their jurisdiction, Arch. Sex. Behav. 23: 81, 1994) -- women who are confused, being coerced by the real abuser ("To Kill a Mockingbird"), seeking revenge, or desperately in need of help with some other (often terrible) life situation. With over 300 convicted men (about 2/3 of them black) now exonerated by DNA evidence, this should prompt serious thinking before anyone is convicted solely on someone's word. The US Air Force, which is reality-based, gives a figure of 60% -- in this series, it was common for a woman who was upset to initially overstate things and admit it as things settled down. (Forensic Science Digest 11(4): 64, December 1985). That these women are often deeply troubled excites any decent person's pity without diminishing the injustice. Today, even the conservative Victoria Forensic Science Center considers "false sexual assault" to be a common diagnosis that the physician in the emergency room can often make just by examining the clothing (J. For. Sci. 45: 568, 2000). The "2% statistic" from the old politically-correct FBI Uniform crme report program, while dogma in many (most?) women's-protection circles, is clearly not true and even informed women's advocates say it needs to be abandoned (Violence Against Women 16: 1356, 2010). Neither gender has a monopoly on good and evil, but currently the law places men at certain disadvantages that puzzle me. For example, a woman's previous false accusations of rape, even if numerous, generally cannot be mentioned by a man in his own defense. During the early 1990's, coinciding with the "false memories" / "people forget things" fiasco, if a man passed a polygraph exam, and there was no physical evidence against him, and he appeared utterly sincere, and it was simply her word against his, the man got told that he was inded a rapist and "had forgotten" or was "in denial". If the physical evidence contradicted the accuser's story, the "child protection advocates" egregiously misused the scientific literature (notably Pediatrics 94: 310, 1996). I still see this. You can cite additional examples. However, guys -- you do NOT want to end up a defendant. It helps to obtain specific and verbal permission prior to each step of the lovemaking process (that's gentlemanly and fun). Dude: You text her ("I want you"), she texts back ("I want you") and you're safe. But the moment she seems even slightly uncomfortable, end the whole thing. Speaking of "links", in the one massive study comparing normal men, rapists, and child molesters, "frequency of adult use of sexually explicit material does not differ significantly among groups". This surprised me. Nor did the frequency of sex crimes increase in Sweden when they made the even the most dopiest-nastiest stuff as available as alcohol and tobacco. See J. Sex. Marit. Ther. 19: 77, 1993. Update: Scientific American July 22, 2011 ("no negative effects, and it may even deter sexual violence"). I'd like an easy scapegoat, too, Mr. Bundy and the rest of you, but the roots of your evil went much, much deeper. The pop claim is that x-rated stuff is naturally addictive (like tobacco or heroin) and leads to escalating tensions that must eventually be acted out. This may be true for individuals like the young Mr. Bundy, and probably specialist treatment would be wise for these men sooner rather than later. It's clearly not true for the vast majority of men, or the world would be a far different place. But we're into politics rather than science. And as politicians and "progressive thinkers" tell us over and over about the dangers of erotica, we still hear almost no complaints about the vile school of rap music with lyrics that degrade women and glorify sexual violence. The evidence that this causes to violence against young women in the underclass communities is overwhelming (Pediatrics 118: e430, 2006). Porn addiction melts away with a little naltrexone: Mayo Clin. Proc. 83: 226, 2008. Meds for Parkinson's trigger porn addiction: Parkinsonism 12: 392, 2006. The paraphilias: Psych. Clin. N.A. 15: 675, 1992. "A review of sexual behavior in the United States": Am. J. Psych. 151: 330, 1994. Natural selection obviously is much harsher on men than on women, and this is the case throughout nature. Is this why there's sex? Nature 411: 689 & 692, 2001.
* Heard that FSH is necessary for Sertoli cell development, spermatogenesis and fertility? Surprise -- it's not (though it helps; in mice or men, Nature Genetics 15: 201 & 205, 1997).
|
|
* SLICE OF LIFE REVIEW
{00083} testes, normal
{10268} prostate, normal
{10898} atrophy, testes with normal comparison
{11762} prostate, normal
{11763} prostate, normal
{15000} testis (tunica albuginea), normal
{15001} testis, normal
{15002} seminiferous tubule, normal
{15003} seminiferous tubule, normal
{15004} seminiferous tubule, normal
{15005} seminiferous tubule, normal
{15006} seminiferous tubule, normal
{15007} sertoli cell, normal
{15008} sertoli cell, normal
{15009} interstitial cells leydig, normal
{15010} interstitial cells leydig, normal
{15011} rete testis, normal
{15012} rete testis, normal
{15013} rete testis, normal
{15014} ductuli efferentes, normal
{15015} epididymis, normal
{15016} epididymis with spermatozoa, normal
{15017} epididymis with * spermatozoa, normal
{15018} epididymis with stereocilia, normal
{15019} epididymis with stereocilia, normal
{15020} ductus deferens, normal
{15021} ductus deferens, normal
{15022} ductus deferens, normal
{15023} ductus deferens, normal
{15024} seminal vesicle, normal
{15025} seminal vesicle, normal
{15026} seminal vesicle (secretory epithelium)
{15027} prostate with concretion, normal
{15028} prostate with concretion, normal
{15029} prostate epithelium, normal
{15030} prostate epithelium, normal
{15031} prostate epithelium and concretions, nor
{15032} urethra, normal
{15033} urethra, normal
{15125} prostate
{15127} prostate
{15128} prostate
{15129} prostate
{15304} prostate
{15330} seminal vesicle, normal
{15331} seminal vesicle, normal
{15332} testes, tunica albuginea
{15333} testes, tunica albuginea
{15577} testes, normal unfixed
{15578} testes, normal unfixed
{15579} testes, normal
{15580} testes, normal unfixed
{15587} bladder and prostate, normal unfixed
{15589} prostate, normal
{17008} prostate, normal
{20213} prostate, normal
{20652} leydig cell, testes
{20653} rete testis, normal
{20653} rete testis, normal
{20654} rete testis, normal
{20654} rete testis, normal
{20655} testis, normal
{20656} sertoli cell nucleus, testis
{20657} spermatogonia, testis
{20658} testis, normal
{20659} epididymis, normal
{20660} ductus deferens, normal
|
* When I was one-and-twenty
I heard a wise man say, "Give crowns and pounds and guineas But not your heart away; Give pearls away and rubies But keep your fancy free." But I was one-and-twenty, No use to talk to me. When I was one-and-twenty
-- A.E. Housman, "A Shropshire Lad" |
* When I was one-and-twenty,
My ills were in their prime, With aches and pains aplenty, And gout before my time; I had the pyorrhea, And fever turned me blue-- They said that I would be a Dead man at twenty-two. Now I am two-and-twenty,
Samuel Hoffenstein,
|
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about this topic in pathology to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
| New visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
