Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.

|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected. No texting or chat messages, please. Ordinary e-mails are welcome.
 I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles that you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
![]() KCUMB Students
KCUMB Students
"Big Robbins" -- Kidney
Lectures follow Textbook
LEARNING OBJECTIVES
What tests do you use to screen a patient for kidney disease? Who should you screen? How do you order the tests?
What kidney diseases can cause an elevated serum urea (BUN, etc.)? What else besides kidney disease can do this?
What kidney diseases can cause an elevated serum creatinine? What else besides kidney disease can do this? What does a creatinine clearance tell you?
What factors determine the specific gravity and sodium concentration in urine? How do you tell prerenal azotemia from acute tubular necrosis / "acute renal injury"?
What does an elevated serum uric acid tell you?
GENERAL
Kidney problems are very common in clinical medicine. Essentially all seriously sick patients will need their kidney function evaluated during the course of their illnesses.
After history and physical exam are complete, the initial steps in checking patients' kidneys are performing a (1) urinalysis and obtaining a (2) serum creatinine and/or (3) serum urea ("blood urea nitrogen", "BUN") level. Next, you may check (4) ability to concentrate urine.
Both creatinine and BUN are included on the common chemical profiles. You can check the ability to concentrate urine using a hygrometer, refractometer, or dipstick.
Indications for these tests:
Newly discovered high blood pressure or diabetes
Abnormal urinalysis (anything more than "trace protein" or "honeymoon cystitis")
Any medical problem serious enough to admit the patient to the hospital
Any life-threatening injury or illness
This section focuses on how to use blood tests to assess kidney function. Other units will introduce urine testing.
You should probably refer to a nephrologist when a man's creatinine exceeds 2.0 mg/dL, a woman's 1.5 mg/dL (NIH, 1993).
UREA ("BUN")
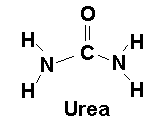 Urea, as you remember, is a relatively nontoxic substance made by the liver as a means of disposing
of ammonia from protein metabolism.
Urea, as you remember, is a relatively nontoxic substance made by the liver as a means of disposing
of ammonia from protein metabolism.
*Urea has MW 60, of which 28 comes from the two nitrogen atoms.
Clinical chemists used to measure only the nitrogen in urea, hence the "urea nitrogen" measurement on lab reports.
The real concentration of urea is BUN x (60/28), or BUN x 2.14. But everyone thinks in terms of BUN units.
Normal blood urea nitrogen is 8-25 mg/dL (2.9-8.9 mmol/L).
Urea is filtered by the glomerulus. If the glomerular filtrate is flowing slowly through the proximal tubule, urea tends to be passively reabsorbed and return to the bloodstream.
Blood urea levels are quite sensitive indicators of renal disease, becoming elevated when renal function drops to around 25-50% of normal (remember the kidney has great functional reserve). The interpretation of the BUN is usually straightforward, though there are a few things to remember.
Increased BUN is, by definition, azotemia. It is due either to increased protein catabolism or impaired kidney function.
Increased protein catabolism results from:
Impaired kidney function may be "prerenal", "renal", or "postrenal".
dehydration (lots of things, even contrast media, can cause this), hemorrhage, shock, congestive heart failure (review: NEJM 320: 397, 1989; but a poor guide to therapy, at least in kids: Ann. Emerg. Med. 18; 755, 1989); glomerulonephritis is likely also to be "prerenal" if mild, since it compromises renal blood flow more than tubular function.
* A mean arterial pressure below 80 mmHg for a few hours will result in prerenal azotemia.
acute tubular necrosis (ischemic, toxic), chronic interstitial nephritis, some glomerulonephritis, etc.; especially nowadays, remember ibuprofen / NSAIDS
prostate trouble, stones, surgical mishaps, tumors
See below for some ways to distinguish these causes of azotemia.
In acute renal failure, BUN increases around 20 mg/dL each day (*estimates vary; range of increase is 10-50 mg/dL daily).
Decreased BUN
Lack of protein (celiac disease, some patients with nephrotic syndrome)
Severe liver disease (end-stage cirrhosis, yellow atrophy, really bad hepatitis, halothane or acetaminophen toxicity, enzyme defects)
Overhydration (iatrogenic, psychogenic water-drinking)
CREATININE
This breakdown product of creatine phosphate is released from skeletal muscle at a steady rate. (Only a small amount comes from meat in the diet.) Serum creatine correlates quite well with the percent of the body that is skeletal muscle.
It is filtered by the glomerulus, and a small amount is also secreted into the glomerular filtrate by the proximal tubule (hence at low GFR's, the usual reciprocal relationship breaks down and creatinine tends to underestimate how low the GFR has gotten).
If the urine volume goes up, the serum creatinine does go down slightly.
Creatinine is generally considered a somewhat more sensitive and specific test of renal function than BUN (for example, Arch. Dis. Child. 67(10SN): 1146, 1992; a more sensitive formula for "Cr-GFR" that takes into account a kid's height: Arch. Dis. Child. 64: 1261, 1989).
* Bedside testing of serum creatinine using a reflectance meter: Br. J. Urol. 57: 510, 1985.
* Historically, creatinine assays by clinical labs have been problematic, with values being by up to 34%; since 2003, new methodologies have reduced the maximum error to about 10% (Arch. Path. Lab. Med. 137: 496, 2013).
The usual range for serum creatinine is 0.6-1.5 mg/dL (53-133 micromoles/L). Whenever I've screened medical students, most of the women fall in the 0.6-1.0 range, most of the men in the 0.9-1.3 range. See also J. Lab. Clin. Med. 116: 327, 1990.
Increased creatinine is due to any cause of impaired kidney function listed above, a lot of meat in the diet, or a very large muscle mass (bodybuilders, anabolic steroid users, giants and acromegaly patients).
In massive rhabdomyolysis / crush injury, there is so much creatine released that the creatinine will probably rise.
Athletes taking oral creatine may have slightly increases in serum creatinine levels for the next day or so, but the effect is slight and unlikely to take a person above the normal range (Br. J. Sports Med. 34: 284, 2000). An army study (yes, creatine does increase your ability to do push-ups) did find elevated serum creatinine that could be misinterreted (Military Medicine 172: 312, 2007).
Decreased creatinine has little significance.
Because of the steady rate of creatinine excretion, substances in the urine are conveniently measured "per gram of creatinine". This is a reasonable alternative to 24 hour urine collection when we're not concerned about something that's produced sporadically.
Creatinine clearance (Br. Med. J. 293: 1119, 1986) is widely used to approximate glomerular filtration rate (which it does pretty well; Clin. Chem 35: 312, 1989; Arthr. Rheum. 33: 277, 1990). You need a timed urine sample and a blood sample.
You remember that the clearance of a substance is the volume of plasma "cleared" of that substance per unit time.
Clearance=(conc. in urine)x(urine volume)/(conc. in plasma). Derive this.
In deciding how to "time" your collection, remember that you don't really need to collect urine for a full 24 hours (patients often don't collect it all anyway). One group got more reliable results by a controlled collection over 4 hours, monitoring body position (kept them lying down) and hydration (Am. J. Ob. Gyn. 169: 576, 1993).
Creatinine clearance is not a perfect measure of GFR, because some is not filtered and some is secreted into the proximal tubule. These fractions tend to cancel each other out in health, but when GFR drops below 30 mL/min, tubular secretion approaches or even exceeds the amount filtered at the glomerulus (Surg. Gyn. Ob. 173: 279, 1991.)
Reference range for creatinine clearance is 90-120 mL/min for young adults; values tend to fall by around 0.5 mL/year over age 20, worse for hypertensives (Nephron 47(S1): 62, 1987.
*Formulas to adjust "normal" for body surface area have been devised, etc. See Clin. Pharmacy 6: 399, 1987. For kids, a height/creatinine ratio of 2.1 or less is normal: Arch. Dis. Child. 64: 1261, 1989. GFR for adults can be estimated by various formulas; try 1.12xCrCl-20.6 (Clin. Pharm. Ther. 48: 503, 1990).
Whether or not "corrections" are applied, creatinine clearance is a pretty good estimate of glomerular filtration rate except at very low values, when tubular secretion of creatinine becomes proportionately greater. For these people, you can average creatinine clearance and urea clearance (remember urea tends to diffuse back through the tubules).
MDRD: eGRF (mL/min per 1.73 m2 = 186.3 x serum creatinine-1.154 x age in years -0.203 x 1.212 (if black) x 0.742 (if female)
Your lecturer has spent years answering people's questions, "The lab estimated my glomerular filtration rate from my creatinine and I was told I had chronic kidney disease; but the nephrologist said I did not." This nonsense has finally come to the attention of my fellow-physicians, who noted that 70% of referrals to nephrologists are bogus based on this nonsensical lab practice (JAMA 303: 1151 & 1201, 2010).
Your lecturer has decided that the eGFR is a product of Big Pharma, who want as many people as possible on pills, especially for diabetes, and have generated this silly formula to lead people to believe that their kidneys are going bad. I have other pathologist colleagues who agree.
* Cystatin C ("gamma-trace protein", produced at a pretty much constant rate by all nucleated cells) functions much as does creatinine as a way of estimating GFR in screening for renal disease. It's being used now for epidemiology (JAMA 305: 1545, 2011; NEJM 367: 20, 2012); it is unlikely to replace BUN / creatinine. The "estimated GFR's" obtained using cystatin C correlate much better than creatinine-based ones with people actually being sick / dying (NEJM 369: 932, 2013). It is supposed to be less dependent on muscularity, but body composition is still a factor. It's also superior to creatinine in the presence of congestive heart failure (Heart 98: 319, 2012).
At present, "chronic kidney disease" is defined, only for the purpose of epidemiologic studies, as creatinine-estimated GFR less than 60 mL / min / 1.73 m2 or urine albumin-to-creatinine ratio of 30 mg/gm or higher. Again, these numbers and formulas weren't meant for individuals
If you are really interested, epidemiologists take the estimated GFR and define five categories of chronic kidney disease. "1" is GFR above 90 /ml/min/1.73m2 and some reason to think the kidney is damaged, or protenuria. "2/mild" is GFR 60-89; "3/moderate" is 30-59; "4/severe" is GFR 15-29; "5/failure" is under 15 and you may or may not be on dialysis. "
PRERENAL VS. RENAL AZOTEMIA
A very common clinical problem is to distinguish prerenal azotemia (due to shock, dehydration, CHF -- also "hepatorenal syndrome") from renal azotemia (acute tubular necrosis, "acute renal injury", "renal shutdown".)
Either could be the cause when a patient has been hypotensive and now is azotemic and oliguric. The management is different.
One older technique is to calculate the BUN/creatinine ratio.
This is normally around 10.
Values over 10, especially over 20, suggest prerenal azotemia rather than acute tubular necrosis / "acute renal injury". (Why? Figure it out yourself.)
High values are also seen postrenal azotemia and upper GI bleeding.
In fact, a high BUN/creatinine ratio is a common finding, especially in the elderly, and a marker for ill-health (delirium study Ann. Int. Med. 119: 474, 1993).
Another approach is to measure sodium on a urine specimen.
In prerenal azotemia, urine sodium is low (the kidney responds to low blood flow by "trying to retain all the sodium it can.")
In acute tubular necrosis ("acuate renal injury"), urine sodium is higher (the renal tubules are unable to concentrate or dilute the glomerular filtrate effectively.)
Urinary sodium under 20 mEq/L suggests prerenal azotemia (or hepatorenal syndrome, etc.); urinary sodium over 40 mEq/L suggests acute tubular necrosis.
And of course you'll look at the urine osmolality. More than 500 mOsmol suggests prerenal azotemia, less than 350 mOsmol suggests acute tubular necrosis.
And of course you'll look at the urinary sediment for the casts of acute tubular necrosis.
*A further refinement is to measure the fractional excretion of filtered sodium, approximated by:
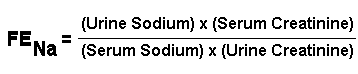
Values less than 1% indicate prerenal azotemia; values over 2% indicate acute tubular necrosis / "acute renal injury".
Several other factors can complicate the picture in such patients.
Diuretics will of course increase the excretion of filtered sodium, while secondary hyperaldosteronism (as in cirrhosis) will decrease sodium excretion.
In acute tubular necrosis due to myoglobinuria, sodium excretion is low (the tubules are plugged, not damaged.)
*Tip: If you obtain urine by squeezing a diaper or the absorptive balls you placed into the diaper, your estimate of urine creatinine will be low because these things absorb creatinine (Am. J. Clin. Nut. 55: 326, 1992).
Over a dozen variations on these bedside methods exist to tell you why your very-sick patient isn't making urine.
*Here are two popular ways of noting lab values in a patient's chart:

* LESS FAMILIAR RENAL FUNCTION TESTS
N-acetyl-beta-D-glucosaminidase ("glucosaminidase", NAG) is a lysosomal enzyme (MW 140,000) found in serum and urine. Urinary NAG is a proposed marker for tubular disease, especially subtle industrial poisoning, acute pyelonephritis, early acute tubular necrosis, and early transplant rejection. The use is looking for early acute tubular necrosis is now established as a research tool, and urinary L-type fatty acid-binding protein (L-FABP) (Ann. Thorac. Surg. 93: 577, 2012; Am. J. Path. 178: 1021, 2011) and neutrophil gelatinase-associated lipocalin (Am. J. Med. 125: 168, 2012; Am. J. Coll. Card. 59: 246, 2012) have also been explored. Toxicologists use several others (Clin. Tox. 49: 720, 2011).
Researchers still use beta-2 microglobulin for chronic tubular disease.
The long ammonium chloride test checks for renal tubular acidosis type I (i.e., inability of the distal tubule to excrete a load of fixed acid). Ammonium chloride is administered orally and a person with "RTA I" supposedly will not be able to acidify the urine as low as pH 5.4.
Adenosine Deaminase Binding Protein is an enzyme from the brush borders of the proximal tubule. Like NAG, its presence in urine indicates tubular disease.
Urinary alkaline phosphatase in urine comes from the proximal tubular brush border (Radiology `82: 419, 1992).
Beta-2 microglobulin (beta-2-m) is the short chain of the HLA class I proteins. In health, it is freely filtered by the glomerulus, and fully reabsorbed by the proximal tubule.
Serum beta-2-m has been suggested as a measure of glomerular filtration rate, similar to creatinine. Obviously this isn't a good idea for patients with tissue necrosis, lymphomas, etc.
Urine beta-2-m has found widespread acceptance as an research tool. It appears if levels in the serum and glomerular filtrate exceed what the proximal tubule can reabsorb (more than 4.5 mg/L) or if there is renal tubular disease. It is very sensitive as an indicator of the latter. Review: Kid. Int. 32: 635, 1987.
Tubular functions: Urinary amino acids and maximum concentrating ability are sensitive screens for tubular damage. Lithium clearance is a researcher's way of estimating delivery to the distal tubule. You'll also read about urinary transthyretin (retinol binding protein: Arch. Dis. Child. 64: 1264, 1989) and atrial natriuretic peptide challenge. Don't worry about these now!
Isotope scans exist to compare the function of the kidneys (J. Nuc. Med. 28: 829, 1987). These may prove a valuable supplement to the intravenous pyelogram. The color Doppler sonogram, which is cheap and portable, has proved even more useful than these scans in transplant patients: Surg. Gyn. Ob. 173: 279, 1991. There's a Tc99 scanner that monitors glomerular filtration minute by minute, suitable for the intensive care unit (J. Am. Soc. Neph. 4: 142, 1994, abstract 94214051).
Urinary alanine aminopeptidase may be used clinically to detect acute tubular necrosis (elevated). It is an old test that never really became popular.
Positron emission tomography is the latest way of measuring renal blood flow. See J. Urol. 150: 1064, 1993. Using the new scanners to calculate the glomerular filtration per unit volume of kidney: J. Urol. 165: 382, 2001.
SPECIFIC GRAVITY OF URINE
While not a "blood test", checking urine specific gravity provides very important information about tubular function and hydration.
People in our culture drink relatively little fluid. Thus "normal" people have fairly concentrated urine (SG greater than 1.010). Of course, the same is true of patients in prerenal azotemia (high urinary specific gravity and osmolality -- usually above 500 -- , low or zero urinary sodium).
Patients with tubular disease ("renal azotemia", i.e., acute tubular necrosis, really bad bilateral pyelonephritis or interstitial nephritis, or on diuretics, or with end-stage kidney) will have isosthenuria (SG 1.010 or so, osmolality not much more than plasma (280), perhaps 300-350 mOsm/kg(L).
Polyuria is present if there are more than 3 liters of water passed daily. If the osmolality of the urine is over 300 mOsm/L, there's a solute diuresis -- you must find why. If not, and the person's not drinking a huge amount of water, the workup for being unable to concentrate urine needs to take place.
Patients getting lots of fluid by IV, or with diabetes insipidus, or enthusiastic water-drinkers (asthmatics, crazies) will have low urine specific gravity.
To distinguish nephrogenic diabetes insipidus (the kidney cannot respond to hADH) from central diabetes insipidus (the patient cannot make hADH), we suggest a serum hADH. If there's still doubt, try a water deprivation test administering hADH / vasopressin and see if the patient is able to concentrate the urine.
URIC ACID
This breakdown product of purine metabolism is filtered by the glomeruli and both reabsorbed and secreted by the renal tubules. Serum levels are highly variable from day to day.
Indications for ordering this test include suspected gout and suspect uric acid nephropathy. However, it is generally measured as part of an automated chemistry profile.
Increased serum uric acid is often seen in:
Low uric acid levels are of no concern (Nephron 51: 13, 1989). Remember that the average man has a higher average serum uric acid than the average woman.
TO THINK ABOUT:
1. Why is a decreased BUN seldom a finding of great interest to clinicians?
2. What are advantages and disadvantages of measuring a urinary substance "per gram of creatinine"?
3. What are the two reasons that upper GI bleeders have increased BUN?
4. What is the pathophysiology behind the use of the BUN/creatinine ratio?
5. What is the pathophysiology behind the use of the fractional excretion of filtered sodium? How is the approximate formula derived?
6. Why is uric acid usually included on the routine chemical profile?
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about renal function testing to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
| New visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
