Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.

|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com No texting or chat messages, please. Ordinary e-mails are welcome. Your confidentiality is completely respected.
I am active in HealthTap, which provides free medical guidance from your cell phone. There is also a fee site at www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
123doc -- a major medical education site, especially for exam preparation
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles which you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
The student will describe the specificity of the common stains used in histopathology.
The student will correctly define the following terms as used in pathology, supply them (given a definition), and mention their significance:
amyloid
hemosiderosis
dystrophic calcification
jaundice
fatty change
lipophage
fatty ingrowth
metastatic calcification
ferruginous body
viral inclusions![]()
hemochromatosis
xanthoma
Given a photomicrograph or glass slide, plus any clinical or special-stain information that may be necessary, the student will recognize:
alcoholic hyaline
glycogen (liver cell nuclei)
cholesterol crystals ("needles")
metastatic calcification
dystrophic calcification
stromal infiltration of fat
fatty change in the liver
tophus of gout
Gaucher cells
viral inclusion (herpes![]() )
)
| The student will explain the origins of each of the important tissue pigments (bilirubin, carbon, hemosiderin, lipofuscin, melanin), and recognize each in tissue sections (given appropriate supplementary information when necessary). | 
|
The student will recognize the following "hyaline" substances, given the appropriate setting:
amyloid
basement membrane
hyalinized collagen (keloid)
fibrin
Mallory's hyaline (prekeratin)
fibrinoid (necrosis)
Russell body (immunoglobulin)
The student will recognize why liver cells accumulate fat during alcohol abuse, and list the classic causes of fatty change in the liver and heart respectively.
The student will describe and account for the accumulation of glycogen in cells in patients with diabetes, storage disease, and on IVs.
The student will recognize the major mechanisms of jaundice.
Given a yellow patient, the student will correctly distinguish carotenemia, jaundice, and uremia.
The student will describe typical sites and settings for dystrophic and metastatic calcification, myxoid change, and mitochondrial aberrations.
![]() KCUMB Students
KCUMB Students
"Big Robbins" -- Cell Injury
Lectures follow Textbook
QUIZBANK
Necrosis #'s 55-65, 69-70, 72
Minerals and pigments (all)
|
|
|
|
|
|
|
|
|
LEARN FIRST
Hematoxylin stains nucleic acids, bacteria, and calcium blue. Eosin stains arginine and lysine (i.e., protein molecules) pink. PAS stains insoluble carbohydrates magenta; d-PAS stain is used to prove something PAS-positive is, or is not, glycogen.
Acid-fast stains selectively stain mycobacteria.
Fatty change is too much fat in business cells that shouldn't ordinarily accumulate it; it's a sign that the cell is sick. Fatty ingrowth is extra adipocytes in an organ where they don't usually belong.
Hemosiderin is iron storage pigment. You distinguish it using the Prussian Blue stain.
Melanin is the familiar skin pigment. You distinguish it because it loses its color on being exposed to hair bleach.
Bilirubin (with a mix of biliverdin) pigment generally occurs with bile plugs or bile lakes in the liver.
Lipofuscin is an inert, wear-and-tear pigment. You distinguish it by its location, or by process of elimination.
Dystrophic calcification results from disease at the site of calcification. Metastatic calcification results from disease remote from the site of calcification that has caused elevated blood calcium or phosphate.
"Hyaline" is a generic term for amorphous masses of protein (usually a single protein).
Amyloid is beta-pleated anything. You identify it using Congo Red staining.
"Fibrinoid necrosis" of a vessel means the endothelium has been badly damaged, and fibrin and other proteins have precipitated in the wall.
INTRODUCTION
This unit will teach you to recognize some things that pop up again and again when we look at disease. You know much of this material already.
You will already have heard about some of these pathologic changes. This unit will emphasize how they look.
STAINS FOR MEDICAL STUDENTS
|
|
Tissue stains stain whatever is left in the embedded tissue after processing. (Standard processing of formalin-fixed tissue removes small non-protein molecules, especially lipids.)
Clinicians need to know only a little about stains used by pathologists in establishing diagnosis. The following will come in handy in understanding pathology slides and reports:
HEMATOXYLIN AND EOSIN (H&E) is the standard tissue stain.
The pedagogical explanation ("hematoxylin is basic and stains acids, eosin is acidic and stains bases") isn't true.
Hematoxylin (blue-purple) is a metal chelator. We usually use it with aluminum ions, which link it to fixed phosphate groups. Hematoxylin stains nucleic acids, calcium salts, and bacteria BLUE-PURPLE.
* If the staining solution is too acidic, the hematoxylin will instead stain the arginine in the nuclear histones red. Even the MGH slide-making lab does this sometimes.
 | * Hematoxylin comes from logwood, the exotic jungle tree. The blues and purples of the clothes of the baroque era were mostly hematoxylin. The logwood tree formed the basis of the economy, and drove the history, of Belize, where it appears on the flag and coat of arms. |  |
Eosin (red) binds to free amino groups and thus stains arginine and lysine PINK TO RED.
Air, water, fat, and carbohydrate end up unstained.
The Romanowsky stain family, including Wright and Giemsa, use a similar color scheme, though with somewhat different dyes and some nice metachromasia. You'll encounter these stains when we study blood and bone-marrow smears.
* Future pathologists: Diff-Quik, the fifteen-second Romanowsky dip especially popular for fine-needle aspirates, (1) fixes with methanol; (2) stains proteins with xanthene-azide; (3) stains nucleic acid with thiazine.
PERIODIC ACID-SCHIFF (PAS) is a stain based on the familiar periodic acid (H+IO4-) oxidation (cis-diols to aldehydes) and Schiff-base reactions.
Anything with a cis-dihydroxy group, i.e., insoluble sugar compounds such as ...
... gets stained MAGENTA.
DIASTASE-PAS ("PAS-D" / "D-PAS") is the PAS reaction performed on tissue previously digested by diastase, which removes glycogen.
The pathologist can buy diastase, or can spit on the slide before staining. If something is PAS-positive and d-PAS negative, you know it is glycogen.
RETICULIN stains the delicate fibers that surround small blood vessels and hold together liver, spleen, and lymph nodes.
PRUSSIAN BLUE uses a special solution of ferrocyanide.
By the familiar reaction (college chemistry, laundry bluing, old-fashioned blueprints), it stains all exposed ferric ions VERY BLUE.
CONGO RED is a special dye that fits tightly into beta-pleated proteins of all sorts.
Beta-pleated proteins in humans are abnormal and are called amyloids. Congo Red stains all amyloids BRICK RED, and everything else PINK. Because of the way beta-pleated sheets line up Congo Red, amyloids also acquire an APPLE GREEN BIREFRINGENCE when stained with Congo Red and then examined under polarized light.
|
{10880} congo red stain of amyloid, kidney
|
![]() Amyloidosis
Amyloidosis
Pittsburgh Illustrated Case
SUDAN / OIL RED O are oil-based stains that can only be used on thin slices ("frozen sections") of tissue from which fat has not been removed. (* Future pathologists: Phospholipids stain pink).
These stain only fat (usually BLACK or BRIGHT RED). The principle is of course hydrophobic bonding.
{17413} fat stain, atherosclerosis, oil red O
{38782} sudan stain, fatty liver
MUCICARMINE is a special dye that stains only epithelial mucin (usually RED). The actual chemistry remains mysterious. (It also light up cryptococcus walls for some reason.)
* ALCIAN BLUE stains certain mucoid substances (hyaluronic acid, sulfomucin, maybe carboxymucin depending on the recipe).
TRICHROME uses familiar aniline dyes to stain collagen (type I, also basement membranes) BLUE or GREEN and everything else some other color. The stain depends on the special way collagen is woven.
ACID-FAST STAINS (ZN / Ziehl-Neelsen, auramine O, others) stain certain waxes a permanent red (or some other color). This shows up mycobacteria (TB bugs) and certain other rare substances.
ARGENTAFFIN STAINS test the ability of cell structures to bind and reduce silver, while ARGYROPHIL STAINS demonstrate all sites of silver binding, whether or not reduction occurs. (Everything that is argentaffin is argyrophil, but not vice-versa.)
METHENAMINE SILVER is the most sensitive and specific common stain for fungi and pneumocystis. It stains them black.
ELASTIC STAINS (Verhoeff, Van Gieson) selectively stain elastic fibers (typically black).
METACHROMATIC STAINS take advantage of molecule-stacking. A single dye will impart a variety of hues to different structures. The most important metachromatic dyes are those use to stain blood and bone marrow smears (the various azures, notably methylene blue and toluidine blue.) For a thrilling account of how intercalated water molecules change the preferred (i.e., differently-colored) resonance hybrid of methylene blue, and thus the basis for metachromasia, see J. Biophys. Bioch. Cyto. 4: 433, 1958.
* LIGHT GREEN stains RNA green.
* ORANGE G stains disulfide bonds orange. Pathologists often add a bit of this to our eosin stain, as it gives keratin a more orange hue than most other proteins.
* PAPANICOLAOU'S STAIN is used for cytology (i.e., smears of cells on glass slides, "Pap" smears). It contains hematoxylin, eosin, light green, orange G, and sometimes Bismarck brown. which imparts a yellow metachromasia to some of the carbohydrates.
* METHYL GREEN PYRONINE stains RNA red and everything else green. It is of historic interest.
IMMUNOSTAINING (immunofluorescence, immunoperoxidase, a few less common) uses monoclonal antibodies to demonstrate specific antigens (i.e., specific proteins) in tissues.
Progesterone receptor: Helps determine the status of a known breast cancer. Stains
the nuclei, of course. Will light up many, but not all, mengingiomas, ovarian and endometrial
carcinomas, and some others.
Prolactin: The familiar molecule
Prostate-specific acid phosphatase: Demonstrates that a metastatic cancer is of prostatic origin. There's a story from my residency days -- ask me if you like.
Prostate-specific alkaline phosphatase: Demonstrates that a metastatic cancer is of prostatic origin
PSA (prostate specific antigen): Demonstrates that a metastatic cancer is of prostatic origin
RCC-Ma: Pretty specific for renal carcinoma cells
Rubella![]() antigen: Infectious agent
antigen: Infectious agent
S-100: Helps with the hard calls. Famously lights up melanomas.
Also cartilage, melanocytes, sweat gland, schwann cells, glia, dendritic macrophages ("histiocytosis X"), some lipoblasts,
renal cell carcinomas, some others, occasionally carcinomas from other sources
SALL4: Seminoma / germinoma, embryonal cell carcinoma, other germ cell tumors positive
Secretory component: Secretory epithelia, notably GI, airways, urothelium
Serotonin: Familiar molecule
SF1: Steroid producing cells
SM-Actin (SMA, smooth muscle actin): Stains smooth muscle and its tumors
Somatostatin: Familiar molecule
SOX10: Upcoming stain for melanoma.
Synaptophysin: Positive in pheochromocytoma, neuroblastoma, carcinoid, and
medullary carcinomas of the thyroid; also some adrenal cortical carcinomas. Usually negative in melanomas, other tumors.
Tamm-Horsfall Protein: Familiar molecule
TdT: A marker for normal immature T-cells; staining indicates that an acute lymphoblastic
leukemia is of T-cell lineage; blast crisis in CML may be TdT positive
Tenascin: An extracellular adhesion molecule, used to prognosticate tumors,
notably colon cancer, by how the stroma is reacting to the invasion
Thrombomodulin: Marker for the cytoplasm of mesothelium and mesothelially-derived tumors, also lights urothelium and its tumors
Thyroglobulin: Some thyroid cancers of follicular cell origin
Toxoplasma![]() : Infectious agent
: Infectious agent
Tryptase: Mast cells
Tyrosinase: Sometimes stains melanomas
TTF-1 ("thyroid transcription factor 1"): Stains nuclei of some cancers, especialy
those of lung origin (adenocarcinoma, oat-cell) and thyroid (follicular, C-cell) origin; also marks type II pneumocytes. Hepatocellular carcinomas
may show cytoplasmic staining. It is always negative in other GI tumors.
Ubiquitin: Lights up the senile plaques and neurofibrillary tangles of Alzheimer's, and the Lewy bodies of Parkinson's and Lewy body dementia
Ulex europaeus: Endothelium
Uroplakin III: Urothelium
Vimentin: Helps make a diagnosis in poorly-differentiated tumors; renal cell carcinomas, mesotheliomas, and mesechymally-derived tumors light up
VIP (vasoactive intestinal peptide):
vWF (von Willebrand's factor): Old marker for megakaryocytes and their leukemias ("M7")
WT1: Wilms' tumor gene product usually positive in serous ovarian cancer,
desmoplastic round cell sarcoma, mesothelioma, Wilms, some lung cancers, other tumors
XIIIa: Macrophage marker, likely to be positive in malignant fibrous histiocytoma
* Immunostaining, and studying how antigens can be lost and recovered, has clarified the mechanism of formalin fixation. Recoverable antigens involve cross-linking of a tyrosine and an amino-sidechain (usually arginine). Am. J. Clin. Path. 121: 190, 2004.
![]() Immunohistochemistry World
Immunohistochemistry World
Pictures and information
Nice
NUCLEIC ACID PROBES are now being introduced to stain particular genes and their RNA's. For example, a cancer cell that contains mRNA for albumin is surely of hepatocyte origin.
FATTY CHANGE ("fatty metamorphosis", "fatty degeneration", "steatosis"): accumulation of excess neutral fat in vacuoles within non-adipocytes
If there's one big fat vacuole in a hepatocyte or elsewhere, it's "macrovesicular". If there's many little fat vacuoles, it's "microvesicular".
FATTY CHANGE OF INJURED CELLS occurs classically in the LIVER and the HEART.
Probably the fat / triglyceride itself does not damage the cells, but is a marker that the cell has been injured.
There are at least six mechanisms by which the liver cell accumulates fat during disease, any or all of which may be operating in a given situation.
1. Too much free fat coming to the liver
2. Too much fatty acid synthesis by the liver
3. Impaired fatty acid oxidation by the liver
4. Excess esterification of fatty acid to triglycerides by the liver
5. Too little apoprotein synthesis by the liver
6. Failure of lipoprotein secretion by the liver.
At first the fat accumulates in the rough endoplasmic reticulum, but soon fat globules occur that are not membrane-bound.
You will care for many patients with fatty liver.
It is now clear that, as the world's population gets fatter, the commonest cause of fatty liver in non-drinkers is non-alcoholic steatohepatitis ("NASH", runs with "the metabolic syndrome"). Much, much more about this later.
Fatty liver develops during heavy drinking, and all six mechanisms are known to contribute here.
As you'd expect (why?), liver hypoxia from any cause will produce mild fatty change. Also note that both ischemia and toxic injury are worst in the centers of the lobules, since this is where the oxygen supply is poorest (why?)
If the fat is periportal, think of malnutrition / total parenteral nutrition / AIDS wasting.
Among the viruses, only hepatitis C produces much fatty change. Nobody knows why.
Other causes of heavy-duty fatty liver include kwashiorkor (why?), Reye's syndrome, poisoning by phosphorus, carbon tetrachloride, outdated tetracycline, pregnancy (rare and mysterious), the bad kind of galactosemia, a host of uncommon inborn errors of metabolism (some of which can announce themselves in adults -- check the ammonia level to find the urea cycle defects), and following ileal bypass for weight reduction.
{46294} fatty liver in kwashiorkor
{40039} Reye's syndrome, liver; microvesicular fatty change
{40040} Reye's syndrome, liver; microvesicular fatty change; oil red O
After a boozy weekend, a person can have several hundred grams of excess fat in the liver. People dying on benders often have livers weighing more than 4000 gm (normal is 1500 gm or so). These livers hurt (stretched Glisson's capsule), can be palpated below the costal arch, and sections float.
By itself, the fat is probably harmless enough, but its presence is a marker for injury.
Patients with fatty livers do occasionally "die of it". A blow to a drinker's abdomen can disrupt enough hepatocytes to cause fatal fat embolization (lung, brain). Or the patient may die of hypoglycemia (not due to the fat, but to the sick liver's not being able to buffer a falling blood glucose.)
{08357} fatty liver, gross (we would confirm
our impression microscopically)
{08366} fatty liver, micro
{08829} fatty liver, micro
{37589} fatty liver, micro
Fatty change in the heart is seen in two classic situations, both fortunately rare today:
(1) It most often reflects poor oxygenation (i.e., chronic severe anemia). It is distributed away from the vessels, and produces a "tiger-stripe" or "thrush-breast" heart.
(2) The heart damaged by diphtheria exotoxin is uniformly flabby and often fatty. (The old idea that diphtheria toxin blocks fatty acid burning by inhibiting the carnitine shuttle has been replaced by the finding that the protein is a nonspecific and very potent inhibitor of protein synthesis.)
Notice that the injured, fat-laden cell may not be permanently damaged or killed. And remember cells can and do die without undergoing fatty changes.
ACCUMULATION OF FAT IN PHAGOCYTIC CELLS is a common theme in pathology. The fat is usually made up largely of CHOLESTEROL ESTERS.
ATHEROSCLEROSIS, still the #1 disease in our country, results when phagocytic cells in the intimal layers of large arteries become engorged with cholesterol and its esters. The phagocytes themselves tend to die off and leave the cholesterol to crystallize.
{11051} early atherosclerosis ("fatty streaks", all of you have these already)
{11648} early atherosclerosis, gross (natural-color and "oil red O stain")
LIPOPHAGES are scavenger macrophages that have devoured fat. This is common wherever lipid-rich tissues (belly fat, brain, others) have been injured, or where alveoli cannot drain (surfactant).
The cytoplasm of these cells typically looks "foamy" ("foam cells", etc.)
{05955} foam cells, wall of gall bladder (these are laden with cholesterol)
{08108} foam cells, wall of gall bladder (ditto)
{01453} microglia (macrophages) eating up necrotic myelin lipid following a stroke
* Likewise, fixed phagocytes the kidney turn into "foam cells" when sick people pass lipoproteins through their glomerular basement membranes.
"Tumors" (nodular hyperplasias, really) composed of these cells are called XANTHOMAS ("xanthos" means yellow). These often (but not always) suggest some problem with blood lipids.
Xanthomas over the extensor tendons: One of the famous markers for familial hypercholesterolemia (lack of LDL receptors).
Flat xanthomas on the palms: If the serum lipids are normal, think of primary biliary cirrhosis.
There are about a dozen obscure illnesses and semi-illnesses in which xanthomas appear around the body. Don't worry about these.
{09741} xanthelasma
{38332} eruptive xanthomas
{24886} xanthoma histology (* the thing that looks like a flower is a "floret" giant cell)
|
|
FATTY INGROWTH ("stromal infiltration of fat", * "lipomatosis") is totally different from fatty change. It is metaplasia of an organ's capillary pericytes into mature adipocytes.
|
This is a common finding in lymph nodes, in the pancreas, and in the right ventricle and atria of the heart. We're seeing it now in the muscles of people on the new anti-HIV medicines. Usually it has no effect on organ function.
* You probably know that all adipocytes are modified pericytes.
* I learned to call this "fatty infiltration". Textbooks use "fatty infiltration" as a not-recommended synonym for fatty change.
* The most important appearance of fatty ingrowth in medical pathology is as a component of most muscular dystrophies. You'll make the diagnosis on other criteria, however.
Fatty ingrowth in skeletal muscle is a hallmark of the HIV-insulin resistance syndrome, seen in patients on long-term antiretroviral therapy (J. Clin. Endo. Metab. 89: 2171, 2004.)
GLYCOGEN ACCUMULATION
Glycogen ordinarily is present in the livers of people in the fed state, and is abundant if the patient has an IV line infusing glucose ("dextrose", "D5", etc.).
In HYPERGLYCEMIA, it is common to see glycogen "in" hepatic nuclei (really, in a deep cup-shaped depression in the side of the nucleus; the nucleus looks clear), pancreatic beta cells, and (if control is really poor) in the proximal tubular epithelial cells (why?). These accumulations are probably harmless.
You'll study glycogen storage diseases later.
{17421} glycogen "in" hepatocyte nuclei
{17422} the real picture of a "glycogen nucleus"
{46306} glycogen in the proximal tubule in poorly-controlled diabetes
The various GLYCOGEN STORAGE DISEASES result from inborn errors of metabolism.
ACCUMULATIONS OF COMPLEX LIPIDS AND CARBOHYDRATES
These typically result from inborn errors of metabolism. Typically the substance is stored in lysosomes. Eventually enough accumulates to compromise organ function.
Now's a good time to memorize what accumulates in what disease:
Gaucher's disease is common, and produces huge, pink-staining, glucocerebroside-laden, "crumpled tissue paper" (* old-timers say "watered-silk") macrophages in the bone marrow and elsewhere.
I-cell disease / "mucolipidosis II" features inability to tag proteins that are to be discarded via the Golgi apparatus.
Before we leave the subject of inborn errors of metabolism, remember that in GOUT, uric acid accumulates in nodules in the tissues. These are called "tophi" (singular "tophus").
IATROGENIC ACCUMULATIONS
LIPOGRANULOMAS in the spleen and celiac lymph nodes are thought to have several causes, including oral mineral oil.
* Enjoy reading about "sclerosing lipogranuloma of the penis" in J. Urol. 133: 1046, 1985. One of the great pathology mysteries solved.
LYMPHANGIOGRAM CONTRAST MEDIUM is an oil from an obsolete imaging technology that stays in lymph nodes for years.
ARGYRIA results from silver salts being permanently deposited in the skin (J. Clin. Path. 47: 556, 1994). With improved industry safety standards, the usual cause today is quack medicines. Update on silver charlatanism: J. Am. Acad. Derm. 53(2S1): S105, 2005. Two faddists make their baby horribly sick: J. Ped. Gastro. 33: 439, 2001. Massive brain damage in an adult using silver as "natural medicine": Neurology 62: 1408, 2004. The fraud is widespread in other nations: Am. J. Ind. Med. 52: 246, 2009. Localized argyria from acupuncture simulates a blue nevus: J. Drugs Derm. 9: 1019, 2010 (do silver needles channel cosmic energies better?) The first report of effective laser treatment (takes a lot of sessions and hurts): Int. J. Derm. 50: 751, 2011.
THORIUM DIOXIDE was, believe it or not, once used to make liver x-rays, as "Thorotrast". It stays around permanently, giving off radiation. Nobody knows how many people were given it, but it was in the millions. People who were followed averaged 14 years less life expectancy (Eur. J. Cancer 44: 1259, 2008 -- the study managed to eliminate people who died soon after their studies because of the disease for which they were scanned.) The major killers are leukemia and primary liver cancers, notably intrahepatic cholangiocarcinomas and angiosarcomas (update Cancer Science 101: 336, 2010).
PIGMENTS
Soluble pigments do not appear in tissue sections. They include CAROTENE (carrot gluttons, most yellow on palms and soles, take a history; your lecturer likes his carrots; NEJM 346: 821, 2002), BILIRUBIN (except in bile plugs), and UROCHROME (kidney failure, check the patient's lab results).
| {12216}carotenemia | 
|
Insoluble pigments inside cells are typically stored in phagolysosomes.
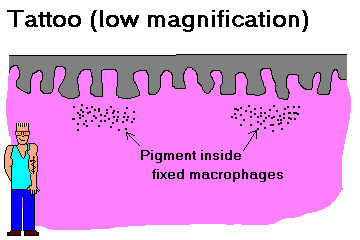
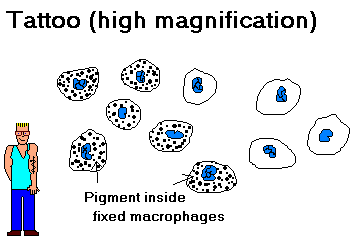
Carbon particles enter our bodies in smoke and soot or as the pigment in jailhouse tattoos (Lancet 338: 380, 1991).
|
{37887} jailhouse tattoo
{17439} interesting tattoos {38249} more tattoos {10943} carbon in macrophages from an excised tattoo |
|
|
|
![]() Tattoo Pigment
Tattoo Pigment
Text and photomicrographs. Nice.
Human Pathology Digital Image Gallery
Carbon settles in macrophages, where it remains indefinitely. Carbon in the lungs and nearby lymph nodes is called "anthracosis". It is inert though ugly. ("If you keep smoking, kid, your lungs will get blacker and blacker!")
|
{17438} carbon in the lung, gross
{17437} carbon in the lung, histology
{36157} carbon in macrophages, papanicolaou stain
{26047} carbon in macrophages, papanicolaou stain
|
|
Other mineral dusts include silica (colorless, very harmful) and iron oxide ("rusty lung", not very harmful).
* NOTE: Professional tattooers use metal salts. Lots of people are allergic to the red mercuric sulfide; the yellow cadmium sulfide is a photosensitizer for some folks. After this, green (often chromium oxide), blue (usually cobalt aluminate), brown (ferric oxide), purple (usually manganse or aluminum), white (titanium oxide or zinc oxide), and black (usually carbon, occasionally iron oxide or even hematoxylin) rank from most to least likely to cause trouble. Tattoo lymphadenopathy: Ob. Gyn. 120: 442, 2012.
LIPOFUSCIN (* "lipochrome"; "fuscus" is Latin for brown)
This is another brown pigment that is now known to be the hard-to-digest residue of subcellular membranes whose unsaturated lipids have been scrambled ("polymerized", "peroxidated", etc.) by free radicals.
For example, lipofuscin is a marker for "oxidative stress" in overworked cells -- this was recently confirmed by a before-and-after biopsy study of patients undergoing repair of mitral valve regurgitation. There was about a 50% reduction in lipofuscin (J. Am. Coll. Card. 55: 671, 2010).
Lipofuscin is the "cellular clinker" or "wear-and-tear pigment". It is considered harmless, and usually takes a weak stain with the lipid dye Sudan* B.
The area of the body most likely to undergo extensive death-and-rebirth (the central area of the liver) are usually loaded with lipofuscin by the time you're an adult.
* Not all lipofuscins are wear-and-tear clinkers. Even in youth, the interstitial cells of the testis, and the epithelial cells of the epididymis and seminal vesicles are packed with lipofuscin, young men's prostatic epithelium has lipofuscin in the central region, and there is lipofuscin at the poles of the cardiac nuclei even in babies. And earwax pigment is an acid-fast lipofuscin. Some of the genetic retinal dystrophies feature abundant lipofuscin accumulation (Am. J. Ophth. 147: 895, 2009).
"Ceroid" is lipofuscin that has become acid-fast and autofluorescent for some reason. It is of no special significance. (* Future pathologists: the best acid-fast stain for this purpose is the Fite.)
* Hamazaki-Wesenberg bodies are giant lysosomes / residual bodies loaded with lipofuscin. Look for them in lymph nodes especially near sarcoid granulomas. They are a minor mystery of medicine. Update J. Clin. Path. 60: 1169, 2007.
* The strange dementia that causes cocker spaniels to attack their masters is ceroid lipofuscinosis involving brains, arteries and smooth muscles.
{17348} lipofuscin (EM and H&E)
* The chemistry of lipofuscin formation is just getting worked out. Recipe: Bioch. Biophys. Acta 1290: 319, 1996.
Lipofuscin becomes more abundant during normal aging, and remains abundant after cells atrophy.
"Brown atrophy" is simply atrophy where the lipofuscin is visible grossly.
{17454} hypertrophy vs. brown atrophy
{18720} hypertrophy vs. brown atrophy
![]() Brown atrophy of the heart
Brown atrophy of the heart
Classic drawing
Adami & McCrae, 1914
A good place to find lipofuscin is at the poles of the nuclei of cardiac muscle cells from elderly people. By age 90, the heart may contain 30% lipofuscin by weight.
{17443} lipofuscin (H&E, EM)
* Two rare genetic diseases (Hermansky-Pudlak and Batten's) feature extensive lipofuscin/ceroid deposition in lysosomes.
* In other species, the faster the rate of basal metabolism, the faster lipofuscin accumulates (J. Ger. 47: B-126, 1992).
MELANOSIS COLI PIGMENT (* "pseudomelanin") is a curious pigment found within macrophages in the mucosa of the colon. This imparts a tortoise-shell appearance to the colons of certain people.
It is typical of people who eat a lot of rhubarb and/or like over-the-counter anthraquinone ("cascara", etc.) laxatives. However, this isn't the whole story (Dis. Col. Rect. 32: 235, 1988). The pigment apparently results from apoptosis of the colonic epithelial cells, and they are then digested by those macrophages, with indigestible cell fragments becoming the pigment. You may also see it in people with inflammatory bowel syndrome who do not use laxatives (from all the damaged cells, J. Clin. Gastro. 26: 167, 1998). Read all about it: Am. J. Path. 131: 465, 1988; update Arch. Path. Lab. Med. 128: 565, 2004 (from someone so devoted to a laxative that the pigment was in the lymph nodes, too).
Even the chemical nature of melanosis coli pigment remains unknown. It reportedly stains as melanin AND lipofuscin; most say it's iron-negative but there's some discussion here. And it's reversible (Colorect. Dis. 11: 788, 2009).
|
|
{49202} melanosis coli
TOBACCO PIGMENT is common in alveolar macrophages in heavy smokers. It is a fine, powdery mix of brown pigments, sometimes including iron. Don't confuse it was carbon, which is black.
![]() Melanoma
Melanoma
Cancer cell with melanin pigment
Urbana Atlas of Pathology
![]() From Greek "melos", black. This is the principal pigment of human skin. It is a complex
composed of
polymerized 5,6-dihydroxyindole and other tyrosine oxidation products.
From Greek "melos", black. This is the principal pigment of human skin. It is a complex
composed of
polymerized 5,6-dihydroxyindole and other tyrosine oxidation products.
Melanins are widely distributed in the animal kingdom, and the melanin in octopus ink is much like ours. Neuromelanin in the brain is much like skin melanin.
Natural selection: Races from near the equator are protected from skin cancer and hypervitaminosis D by dark pigmentation. Races from high latitudes are protected from rickets by light pigmentation.
* Cloning the mouse redhead gene perhaps homologous to a rufous albinism (red-hair, red skin in Africans; Nature 361: 72, 1993). This led to the discovery of MC1R as the usual cause of red hair. People lacking pro-opiomelanocortin also have red hair, along with obesity and congenital hypocortisolism (Hum. Molec. Genet. 11: 1997, 2002; Ann. N.Y. Acad. Sci. 994: 233, 2003).
Albinos cannot make melanin, and usually have genetic defects of tyrosine metabolism.
In the familiar oculocutaneous albinism syndromes, there are often subtle retinal morphologic defects as well -- it seems that you need the melanin of the uveal layer for the retina to form properly (Arch. Ophth. 127: 37, 2009).
|
{53602} albino
{18250} phenylketonuria patient {18253} phenylketonuria patient |

|
Melanin is characteristically seen in melanocytes and their tumors (common "moles", malignant melanomas)
Most (not all) melanomas contain at least a little melanin, and finding melanin production by tumor cells proves a cancer is a melanoma.
To prove a pigment is melanin, the pathologist applies a little hydrogen peroxide (hair bleach) to the section. If it's melanin, it bleaches. * The old Fontana technique uses silver, which is reduced to a black substance by melanin, etc.
Abnormalities of melanin occur in other settings. You will learn them soon enough.
Diseases with increased ACTH ("MSH" -- think especially of primary adrenocortical insufficiency -- why?) cause hyperpigmentation.
![]() Suntanning is physiologic (and does not keep out cancer-causing rays). Ingestion or application of
psoralens (celery juice, limes, etc.) makes the skin sensitive to sunlight.
Suntanning is physiologic (and does not keep out cancer-causing rays). Ingestion or application of
psoralens (celery juice, limes, etc.) makes the skin sensitive to sunlight.
Ferric ion blocks breakdown of melanin, a fact that explains the dark pigmentation in the skin of hemochromatosis patients and over dermatofibromas.
Melanin in the urine indicates extensive malignant melanoma.
The stainable form of iron is hemosiderin, a complex mixture of proteins and ferric ions. It is faintly visible as shiny golden granules in unstained tissue sections.
![]() Hemosiderin
Hemosiderin
In lung macrophages
WebPath Photo
The best way to demonstrate hemosiderin is using acid ferrocyanide, which forms a striking blue complex with stainable ferric ion ("Prussian blue").
In hepatocytes, hemosiderin tends to locate near the bile canaliculi.
Note that ferrous iron in heme groups (hemoglobin, myoglobin, cytochromes) does not stain. Neither does the ferric iron stored as ferritin, since the apoferritin protein shields the iron atoms.
Normally there is some stainable hemosiderin in marrow, spleen, liver.
Lack of stainable iron of course indicates systemic iron deficiency.
Localized accumulations of iron ("local hemosiderosis") reflect longstanding congestion (lungs, leg veins), repeated minor injury (shrapnel fragments, sports, etc.).
Too much iron in the whole body ("generalized hemosiderosis") has several causes that are worth learning now:
 |
Excess
hemosiderin eventually causes organ injury by generating free oxygen radicals. This leads to
organ failure, called "hemochromatosis". ("Hemochromatosis is generalized hemosiderosis
that has made you sick.") This is a major, under-diagnosed, treatable disease in the U.S.
In a few cases, the disease has been detected by sufferers' tripping airport metal detectors. |
{34364} hemosiderin at site of hemorrhage in a malignant brain tumor
{37592} hemosiderin, Prussian blue stain; there is also black carbon
{38491} hemosiderin-laden macrophages in the lung ("heart failure cells")
|
|
|
|
A special case of iron deposition is the FERRUGINOUS BODY of asbestosis -- iron-calcium salts encrusted on an asbestos fiber in the lungs.
{36189} ferruginous body in asbestosis
COPPER PIGMENT
Copper penny and blue copper-salt colors. Deposited in the liver and/or basal ganglia in WILSON'S DISEASE, an important diagnosis not to miss.
* MINOCYCLINE, an antibiotic, is acted upon by the peroxidases in the thyroid and turns the gland black, permanently. To a lesser extent, long-term use can cause pigmentation elsewhere, including the skin (J. Am. Acad. Derm. 57: 836, 2007.
HOMOGENTISIC ACID POLYMER ("alkapton"):
Patients with the hereditary arthritis syndrome "alkaptonuria" accumulate homogentisic acid, a breakdown product of tyrosine / phenylalanine, which polymerizes into black pigment, in their cartilages (nose, ears), joints, sweat. The accumulation itself is called "ochronosis". Histopathology: Am. J. Clin. Path. 90: 95, 1988. Genetics: Nat. Gen. 14: 19, 1996. Update NEJM 347: 2111, 2002.
* "Exogenous ochronosis" is the same polymer laid down in the skin as the result of overuse of skin-lighteners. The skin looks blue and may have nodules.
{18252} ochronosis (black cartilage in the ear)
HEMOZOIN: This is a ferric iron pigment that looks like hemosiderin when unstained, but that does not exhibit the Prussian Blue reaction because the iron is sequestered by protein.
It consists of polymerized heme with each iron atom joined to a carboxyl group on the next porphyrin unit (Proc. Nat. Acad. Sci. 88(2): 325, 1991).
It is seen in reticuloendothelial cells in malaria![]() ; the plasmodia protect themselves from free iron-heme complex by
converting it into this substance. Once it's been deposited, it apparently autocatalyzes its own
production (Nature 374: 269, 1995). Some of the antimalarials work by preventing the bugs from
producing this stuff.
; the plasmodia protect themselves from free iron-heme complex by
converting it into this substance. Once it's been deposited, it apparently autocatalyzes its own
production (Nature 374: 269, 1995). Some of the antimalarials work by preventing the bugs from
producing this stuff.
* Malaria kills as many or more people as AIDS. Almost every one of the deaths could be prevented fairly easily. Three cheers each for Bill Gates and the Global Fund. See Br. Med. J. 328: 1033 & 1086 & 1378, 2004; Lancet 363: 237, 2004; lots more.
* HEMATIN, sometimes deposited in reticuloendothelial cells in other cases of heavy hemolysis, is ferriprotoporphyrin IX hydroxide. You know it as a treatment for some of the porphyrias. Not to be confused with "hematein", which is the oxidized form of hematoxylin.
{12220} jaundice
This is the non-iron-containing, yellow-orange pigment that results from breakdown of porphyrin rings (mostly hemoglobin).
Bilirubin by itself is insoluble in water and is carried on albumin to the liver, where hepatocytes conjugate it with glucuronic acid and pour it into the bile.
Elevated levels of bilirubin in the blood mean jaundice. Mechanisms:
You may see bile plugs (bile in distended canaliculi; big ones that ruptured are "bile lakes") or intracellular bilirubin in the liver in obstructive jaundice or primary cancer of hepatocytes.
{24559} liver that is green from biliary obstruction
{39787} bile plug
Of course, if you find a cancer cell is making bile, you know the cancer arose from a hepatocyte.
| * Fun to know: Two proteins, ligandin and protein Z, process bilirubin in the hepatocyte. Phenobarbital increases ligandin and speeds processing of bilirubin. Once it was fashionable to treat everyone with Gilbert's "disease" with phenobarbital, thereby turning healthy adults with a slightly abnormal lab value into chronically and iatrogenically sick adults with a normal lab value. | 
|
CALCIFICATION: A subject of interest to most physicians, not just radiologists.
Calcium salts (hydroxides, phosphate-hydroxides) are deposited. Regardless of cause, calcium salts stain dark blue on H&E. (* If there is any doubt, special stains like the Von Kossa for phosphate or Alizarin red for calcium itself.)
DYSTROPHIC CALCIFICATION
This is calcification that takes place locally, in the presence of normal overall calcium-phosphorus metabolism.
The calcifications may be of any size.
"Dystrophic" means "seeking out the bad". While a necrotic cell whose mitochondria calcified may provide a nidus for stone-building, some texts suggest that only dead things calcify. This is simply not true.
* In extracellular calcification, calcium salt is often complexed to coagulation factors II, VII, IX, and X, the ones that contain gamma-carboxy glutamic acid (and therefore require vitamin K, etc.)
* Osteopontin is a bone protein that we are now discovering to be produced at sites of unexplained calcification. Stay tuned.
In intracellular calcification, the first organelle to calcify is usually the mitochondrion. Of course, that's the end of the cell....
Several normal structures tend to calcify during adult life.
This includes the pineal gland, the cartilages in the airways, the media of large arteries ("Monckeberg's") and the mitral valve annulus. These are probably harmless.
Around 1% of adults develop calcifications in their otherwise-normal sinuses of Valsalva, causing deadly aortic valve stenosis.
{03560} calcified aortic valve, x-ray
{06461} calcified aortic valve, gross
{45702} calcified carotid artery (the proximal portion of the common carotid, and the proximal
portions of both internal and external carotid arteries are visible; look carefully!)
{15856} dystrophic calcification in heart muscle (myocarditis patient)
|
|
Little bits of calcium help mammographers recognize breast cancer -- there are a great many false positives.
![]() Breast cancer with microcalcification
Breast cancer with microcalcification
WebPath Photo
Advanced atherosclerotic plaques undergo calcification, but this is not the principal problem in atherosclerosis.
![]() Severe atherosclerosis with calcium
Severe atherosclerosis with calcium
WebPath photo
* Claims from the 1990's that dystrophic calcification was caused by biofilms of nanobacteria seem to have come to nothing. The calcium is often deposited as microspherules, but these vary greatly in size, which bacteria wouldn't do. There's still conflicting data, but I was most impressed by a totally-negative study of immunostaining calcified aortic valves for chlamydia (J. Heart Valve Dis. 12: 447, 2003).
* "Chelation therapy" (infusions of EDTA) is a perennial health fraud that claims to "cure atherosclerosis by removing calcium from the walls of vessels". Patients feel their fingers tingle during the infusion, and they are told that this is "proof that the circulation was being restored." Explain.
Dystrophic calcification is characteristic of other diseases as well. The reasons are generally obscure.
Malformed or damaged cardiac valves tend to calcify, especially congenitally bicuspid aortic valves (another common cause of aortic valve stenosis).
Caseous![]() granulomas (tuberculosis, histoplasmosis
granulomas (tuberculosis, histoplasmosis![]() , others) often calcify.
, others) often calcify.
Scars (surgical, myocardial) often calcify.
The fingertip pulp calcifies in scleroderma and CREST syndrome.
Certain tumors contain "psammoma bodies", little spherules of basement membrane that calcify. (Think of thyroid cancer, ovarian cancer, meningioma, somatostatinoma). Little spherical calcifications inside giant cells in granulomas are called "Schaumann bodies" or "conchoid bodies". More about these things later.
{35552} Schaumann bodies in giant cells of granulomas (berylliosis case)
* Uterine fibroids (smooth muscle tumors) often calcify. (This is an ancient finding: Arch. Path. 107: 91, 1983.)
* Calcification of the pinna of the ear occurs for some reason in some cases of longstanding adrenocortical insufficiency (Addison's disease; there are other causes too).
If a fetus dies and calcifies, it may be retained for years as a "lithopedion" ("stone child" -- * read Michael Bishop's famous non-supernatural horror story, "Within the Walls of Tyre").
A special case of dystrophic calcification is precipitation of calcium stearate in pancreatitis-associated fat necrosis. If the celiac plexus is involved, this produces one of medicine's most intractable pain syndromes.
METASTATIC CALCIFICATION:
"Metastatic" means "another place". Here the serum calcium and/or phosphate ion concentration is already elevated for some reason (i.e., disease at some other place). Healthy tissues calcify.
High blood calcium is usually due to cancer destroying bone, high hPTH levels (parathyroid adenomas and hyperplasias, squamous cell carcinoma of the lung, rarely others), sarcoid, vitamin D abuse, milk and antacid abuse.
High blood phosphate is usually due to kidney failure or massive tumor lysis.
* Of course Virchow first explained the mechanism.
* The most grisly example of metastatic calcification is the severe autosomal recessive disease FAMILIAL TUMORAL CALCINOSIS. Gene GALNT3: Nat. Genet. 36: 579, 2004.
Metastatic calcification occurs predictably in the pulmonary alveolar walls, the gastric fundic epithelium (near parietal cells), the basement membranes of certain renal tubules, and the walls of small blood vessels.
Note that all but the last are sites of pH gradients. The calcium precipitates first where there is excess hydroxyl ions.
In very severe lung or kidney involvement, respiratory insufficiency ("pumice lung") or renal tubular failure can occur. But usually metastatic calcification is harmless evidence of serious disease elsewhere.
* Future pathologists: A few calcifications around the thin limb of Henle's loop is "normal" and does not indicate a calcium problem.
{39670}calcification, metastatic, in the lung;
{08099} calcification, metastatic, in the lung
|
|
|
|
Modern-era pathologists: CALCIFICATION OF COLLAGEN is diagnostic of sustained electrical injury (happens at the cathode during electrical torture; J. Clin. Path. 53: 569, 2000; Nature 301: 75, 1983).
Any kind of calcification can OSSIFY, i.e., produce bone and even bone marrow. (It's commonplace to see bone, with active marrow, in airway sections of elderly patients, in calcified atherosclerotic plaques, and so forth.)
HYALINE: Any substance (intracellular or extracellular) that stains a homogeneous (say "homo-JEAN-yuss") pink on routine H&E stains.
{17485} treatise on hyaline
When patients are losing lots of protein trough their glomeruli, it's common to see EOSINOPHILIC DROPLETS IN THE PROXIMAL TUBULAR EPITHELIAL CELLS. This is a good autopsy marker, especially if the patient was not well worked-up during life.
{46308} hyaline droplets in proximal tubules
{17440} hyaline droplets in proximal tubules
RUSSELL BODIES are round accumulations of monoclonal protein that are (or used to be) inside the endoplasmic reticulum, usually immunogloublin within plasma cells. Nobody knows how or why they form, though the question has been addressed by elite pathologists (EMBO Reports 1: 225, 2000).
The only time that, to my knowledge, Russell bodies make a major difference is in the autopsy confirmation of African sleeping sickness. IgM-based Russell bodies abound in the plasma cells within the brain.
* Their intranuclear counterpart is the Dutcher body, seen in Waldenstrom's and mantle cell lymphomas.
* THANATOSOMES (the new name for "hyaline globules") are remnants of apoptotic cells found at sites of ongoing apoptosis (famously chronic gastritis.) Discovery and naming: Hum. Path. 32: 894, 2001; update Am. J. Clin. Path. 127: 792, 2007.
|
|
|
VIRAL INCLUSIONS![]() are crystalloids of virus components within infected cells. The most famous are
herpes
are crystalloids of virus components within infected cells. The most famous are
herpes![]() inclusions -- look in the cell nucleus, since they will give you the diagnosis.
inclusions -- look in the cell nucleus, since they will give you the diagnosis.
MALLORY'S (ALCOHOLIC) HYALINE is scrambled prekeratin intermediate filaments plus ubiquitin, typically in liver cells. This usually reflects weeks of heavy drinking ("alcoholic hepatitis") or years of overeating and not exercising ("bad NASH"). The stuff is eosinophilic and flocculent (i.e., it looks like pink cottage cheese).
Several drugs are also causes. Most important right now is perhaps dideoxyinosine therapy for HIV. Am. J. Clin. Path. 108: 280, 1997.
![]() Mallory's hyaline
Mallory's hyaline
WebPath Photo
{09103} Mallory's alcoholic hyaline, electron micrograph
(upper right)
{17418}
Mallory's alcoholic hyaline, H&E and electron micrograph
Alpha-1 protease inhibitor ("antitrypsin") globules look like multi-sized cherries within hepatocytes that are unable to secrete this product (inborn error, regenerating cells).
![]() Alpha-1 antitrypsin globules
Alpha-1 antitrypsin globules
WebPath Photo
* Biotin and a mix of proteins (i.e., one of them a binder of biotin) cause eosinophilic inclusions and optically-clear nuclei in the endometrial glands in pregnancy: Lancet 364: 532, 2004.
* Giant mitochondria, a feature of alcoholic liver disease. If you can spot these, you have exceeded undergraduate pathology expectations. These are called "Yokoo bodies", having been discovered by one of my teachers. They're seen in a few other entities which seem to have in common cell death mediated via the HMGB1 signallnig protein (Cancer Res. 70: 8558, 2010).
Collagen can hyalinize, especially in keloids / hypertrophic scars and other abnormal fibrous proliferations. Here, it is woven as densely as in osteoid, and hence had the same, pink homogeneous look as other hyaline substances.
{17646} keloid, gross
{17647} keloid, histology
{17648} keloid, histology
{46351} keloid, histology
![]() Keloids (hypertrophic scars?)
Keloids (hypertrophic scars?)
Actor Benjamin Bratt
UCSF Skin-In-Cinema
|
|
Excess basement membrane and other proteins "hyalinizes" the body's small arteries in high blood pressure and diabetes.
Of course this narrows the lumens. Other proteins may attach themselves to the components of the vessel as well.
Thickening and excesses of basement membrane are a major theme in renal glomerular disease, and in diabetes mellitus. Much more about this later.
{17472} hyaline arteriolar sclerosis (right, one on left is normal)
Amyloid, mentioned above, is another extracellular accumulation that always has a hyaline appearance.
{13613} amyloid, H&E
|
|
{11427} fibrin in a premature baby's lung ("hyaline membranes")
|
|
Fibrinoid is a special "material" seen in the walls of blood vessels that are dead but still contain flowing blood. A mix of plasma proteins and dead cell debris solidifies in the media and stains intensely pink.
If solid "hyaline" looks inflamed, it's usually fibrin or "fibrinoid".
* The centers of rheumatoid nodules may be filled with "fibrinoid", and it is also characteristically seen in the myocardium in rheumatic fever.
* Radiation injury to vessels appears as hyaline-fibrinoid in vessel walls. Early, there may be some inflammation and/or necrosis. Later, the vessels look more subdued, but the lumen continues to narrow throughout the patient's life-span.
{01917} radiation injury to vessels; the hyaline fibrinoid is pink
* Future pathologists only: The Splendore-Hoeppli phenomenon of little pink-staining club-shaped
things around actinomyces colonies![]() ,
fungus masses,
schistosome
,
fungus masses,
schistosome![]() eggs, and occasionally other organic-based "foreign bodies".
eggs, and occasionally other organic-based "foreign bodies".
* Future pathologists only: Spironolactone bodies are found in the mineralocorticoid-producing cells of the adrenal gland in people treated with this Rx. They are hyaline, laminated things, up to 15 microns, derived from S.E.R.
In kidney disease, entire glomeruli "hyalinize". Depending on the disease, these dead glomeruli are replaced by basement membrane-mesangial matrix, collagen, and/or plasma proteins.
MYXOID CHANGE
Increased ground substance.
* The comb and wattles of a rooster is the familiar example from normal comparative physiology.
There is increased ground substance throughout much of the body in hypothyroidism (myxedema).
* (Curiously) many patients with Graves' disease (which usually produces hyperthyroidism) have localized accumulation of ground substance on their shins ("pretibial myxedema"; it may be severe enough to compress the lymphatics and give superimposed elephantiasis. See Lancet 341: 403, 1993).
If there is associated damage to the connective tissue fibers, we use the term myxomatous degeneration ("myxoid degeneration").
The two real-life examples are "cystic medial necrosis" of the aorta (prelude to a lethal tearing called "aortic dissection") and Barlow's floppy mitral valve (a semi-disease that if you really search for it affects a few percent of humankind.)
* Myxoid change of the intima narrows the renal arteries in scleroderma and Balkan nephropathy, eventually causing kidney failure.
Accumulation of epithelial mucin, as large pools, may be seen in several diseases, most notably "colloid cancers". More about them later.
ABNORMAL MITOCHONDRIA
Selective damage of the mitochondria (i.e., extreme swelling seen on electron microscopy) is the essential lesion of true Reye's syndrome.
Friedreich's ataxia features clunkers of iron in the mitochondria as the essential lesion.
Parking-lot crystals inside mitochondria are a hallmark of the genetic diseases of mitochondria, in which a portion of their genetic code is faulty. Abnormal creatine kinase is being synthesized and accumulating.
* Most of these diseases show up primarily in muscle (why?), and the sick mitochondria accumulating around the edges of the worse-involved fibers create a "ragged red" appearance. More about this later.
Hürthle cells (oncocytes, Ashkenazy cells, oxyphil cells) have their cytoplasm so packed with mitochondria that there is little room for anything else. You already know these from parathyroid and armpit (apocrine cell) histology. We'll see them at other sites as disease markers; famously, they can pop up in a huge variety of thyroid lesions (Arch. Path. Lab. Med. 132: 1241, 2008).
We've already mentioned the giant mitochondria of the alcoholic's liver.
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about the accumulations and deposits that pathologists see in tissues to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
| New visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
