Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.

|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected. No texting or chat messages, please. Ordinary e-mails are welcome.
 I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles that you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
![]() KCUMB Students
KCUMB Students
"Big Robbins" -- Bones / Joints / Soft Tissue Tumors
Lectures follow Textbook
INTRODUCTION TO ARTHRITIS TESTING
Joint diseases are distinguished from one another by the history and physical exam. You can make a diagnosis with reasonable confidence in most cases without doing ANY labs. The lab tests are ancillary, for confirmation and for monitoring.
Keep this in mind as you work through this confusing unit.
You can do a "sed rate" in your office. ("And get those temporal arteritis / polymyalgia rheumatica patients on glucocorticoids NOW!") For the Westergren, here's a reasonable "normal range":
Women: < up to (age+10)/2
SYNOVIAL FLUID (JAMA 264: 1009, 1990, still the best)
The fluid that nourishes and lubricates the joint space is named "syn-ov-ial" because it is "like egg white" in color and consistency!
It is an ultrafiltrate of extracellular fluid that has passed through the synovial lining, a layer of more-or-less cuboidal cells that possess neither desmosomes nor basement membrane.
Therefore, synovial fluid is almost identical to the rest of the extracellular fluid, except that the synovial lining cells add hyaluronic acid.
INDICATIONS for tapping and examining synovial fluid are fairly well defined. You'll usually do it when there is an acute inflammatory arthritis with an effusion, unless the cause is apparent.
Tests on synovial fluid are old-fashioned but still worth knowing.
Tapping a joint is therapeutic in septic, crystalline, or traumatic arthritis, or when there is a large effusion. You can use the same tap to inject corticosteroids when this is indicated (but be SURE the joint isn't infected!)
The principal hazard is infection and this is rare. Relative CONTRAINDICATIONS are infection in the soft tissues around the joint, sepsis, and bleeding disorder or anticoagulant therapy.
You will learn how to tap a joint in the clinic. Generally the best approaches are on the extensor aspects of the joints. Be sure to use good sterile technique.
* For nice instructions on how to tap each joint in the body, see J. Fam. Pract. 20: 179, 1985.
* One trick to see whether you have synovial fluid is that a droplet will turn toluidine blue dye red. (Hyaluronic acid does this by lining up the dye molecules along the polymer -- it's called "metachromasia".)
If you can, send one mL of fluid in each of two tubes:
Even if you get "nothing", send the needle to the Microbiology lab for culture and sensitivity.
SYNOVIAL FLUID CELLS
Healthy synovial fluid contains fewer than 200 cells/mcL, mostly lymphs.
The lab will at least give the total red and white count, and the percentage of the white cells that are polys.
* If you are performing the count yourself using a counting chamber, remember the white cell diluting solution you use for blood contains acetic acid, which "clots" synovial fluid. Use saline instead. Do NOT use an automatic blood cell counter.
Regardless of the total white count, more than 90% polys strongly suggests septic (bacterial) arthritis.
Red blood cells in the synovial fluid suggests a traumatic tap.
If you do not think this is the problem, the patient probably has a fracture through the joint surface. Look for marrow elements in the synovial fluid, though fat by itself is not diagnostic.
* Other possibilities are hemophilic arthritis, traumatic arthritis, or a tumor (i.e., "pigmented villinodular synovitis").
* Total WBC is not very useful in distinguishing different types of arthritis.
The highest values
(over 100,000/mcL) suggest septic arthritis, TB![]() , or acute gout.
, or acute gout.
* Of course, determining exactly what kinds of lymphocytes, macrophages, cytokines, and bacterial and viral antigens are present in the synovial fluid of study subjects is a major research interest.
SYNOVIAL FLUID CRYSTALS
Crystals found with polys in synovial fluid may establish the diagnosis of gout (uric acid -- if you try, you can recover crystals in 85% of cases) or pseudogout (calcium pyrophosphate). Unless you have a special interest, leave crystal identification to the lab. Probably you do not need fluid to consider a therapeutic trial of gout treatment; a serum uric acid and a typical clinical picture is usually plenty (Arch. Int. Med. 170: 1120, 2010).
* Unless you're a rheumatologist and looking at a synovial fluid aspirate in your office, let the pathology folks in the lab worry about birefringence. For wards trivia -- uric acid crystals are needles and show striking negative birefringence, calcium pyrophosphate crystals are squares / rhomboids and show weak positive birefringence, and the cholesterol crystals that you may see in an immune-based synovitis are rectangular with notched corners and very biregringent (neither strongly negative nor strongly positive) and likely to be accompanied by maltese-cross lipid drops.
All synovial fluid contains some small, calcium-rich crystals, and that these are likely to be numerous in osteoarthritis.
Warning: certain injectable corticosteroid preparations produce needle-shaped crystals that polarize exactly like uric acid.
SYNOVIAL FLUID MUCIN-CLOT ("Ropes test")
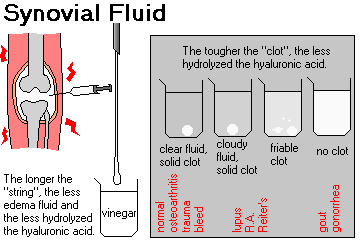
This measures how well-polymerized the hyaluronic acid is.
A few drops of synovial fluid are added to 10 mL or so of 5% acetic acid in a beaker and swirled for a minute. The resulting "clot" is rated:
Inflammation in the joint space damages the hyaluronic polymers, shortening them.
Thus, the "mucin clot" is:
SYNOVIAL FLUID STRING TEST ("Viscosity test")
This test (not to be confused with Ropes, which is a name) measures the polymerization of hyaluronic acid plus how much it has been diluted by the rapid entry of extracellular fluid into an inflamed joint.
All the different ways of doing this test involve stringing a drop of the fluid out (from the end of a syringe, etc., but not between your fingers because of the HIV risk). If you can pull the drop into a string longer than 3 cm, the test is normal.
Interpretation is the same as for the mucin clot test.
OTHER TESTS ON SYNOVIAL FLUID
Synovial fluid GLUCOSE is normally the same as venous glucose in the fasting patient; decreased values occur when there are many white cells, especially polys, active in the joint space. (In septic arthritis, synovial fluid glucose is often more than 40 mg/dL below the venous value).
GRAM STAIN will show the causative organisms in around 70% of cases of gram-positive septic arthritis, and around 30% of cases of gram-negative disease. (When you are getting your cultures ready, remember to inoculate Thayer-Martin medium which will allow the growth of gonococci.) We suggest you get a blood culture as well.
* COMPLEMENT is often low in active joint disease caused by autoimmunity (lupus, rheumatoid arthritis). Again, I cannot recommend spending money on this unless you are a researcher.
* In effusions from patients with lupus, you may see an LE cell (not really pathognomonic, but helpful, and oh, so classic!).
* RHEUMATOID FACTOR may be present in effusions from patients with rheumatoid arthritis when it is not (yet) present in the blood.
* The rice granules of rheumatoid arthritis, which result from failure to clear or organize a fibrinous effusion, are usually too large to pass through even a 16-gauge needle.
* Of course, Congo Red can help identify amyloid in dialysis arthropathy.
SERUM RHEUMATOID FACTOR (RF)
Rheumatoid factor is any autoantibody or autoantibodies (IgM, IgG, or IgA) against the Fc portion of slightly altered IgG.
Probably these contribute to the pathogenesis of joint and vessel disease by forming complexes that attract and activate killer-T cells, fix complement, and so forth.
* The molecular biology is very complicated, of course. The antigen on the altered IgG is Gm(a) or Gm(g); IgG's lacking these antigens can still be recognized by rheumatoid factor if they are aggregated or bound to antigen; maybe this is why some people produce antibody against these "non-self" proteins.
Many procedures have been developed to test for the autoantibody. The two usual tests measure mostly IgM rheumatoid factors.
The standard is based on the agglutination of latex particles coated with IgG.
This "latex slide test" is negative in most people, and titers of 1:80 or less are common in infectious mono, acute inflammation, and up to 15% of people over age 60.
Depending on your lab, you may be instructed to ignore titers of 1:40 or less if you are considering the diagnosis of rheumatoid arthritis. This is the norm nowadays ("Less than 1:80 is negative.")
*nbsp;The older Rose-Waaler test is based on the agglutination of sheep red blood cells coated with rabbit IgG. Some rheumatologists prefer this, or like to get both.
This "sheep red cell tube test" is still popular Normal people have titers 1:16 or less.
The principal INDICATION for ordering a serum "rheumatoid factor" is suspected adult rheumatoid arthritis.
The majority of adults with rheumatoid arthritis will have significant titers of rheumatoid factor (1:160 or above) in their serum.
Circulating rheumatoid factor may precede the illness or only appear later.
The higher the titer (* especially above 1:640), the more likely the patient is to have rheumatoid arthritis.
Titers correlate some with severity of the disease, and do not usually drop in response to treatment. Especially, patients with rheumatoid vasculitis tend to have higher titers. (Perhaps this is why a group in England lately decided that having rheumatoid factor on board was a coronary risk factor and perhaps even etiologic: Heart 93: 1263, 2007).
Around 25% of adults with clinically obvious rheumatoid arthritis never develop rheumatoid factor in the serum ("seronegative" RA).
* Checking synovial fluid for rheumatoid factor is probably obsolete.
* Tests for IgG, IgA, and IgE rheumatoid factors have not proved useful.
Rheumatoid factor is usually ABSENT in patients with arthritis due to one of the following "seronegative arthropathies"
Other causes of "significant titers" of rheumatoid factor in the serum include:
(You can document clinical improvement in patients with SBE or advanced syphilis by their falling RF titers.)
* All type II cryoglobulins are by definition an IgM RF, and all type III cryoglobulins contain it.
Even "young normals" can have high titers of RF. Note that the diseases on the above list are those that tend to feature polyclonal gammopathies.
Lab users: Remember that anemia of chronic disease is common in severe rheumatoid arthritis.
ANTI-CCP ANTIBODIES (anti-cyclic citrullinated antibodies; now anti-CCP1 and anti-CCP2; updates Rheumatology 45: 478, 2006; Ann. Rheum. Dis. 65: 845, 2006; J. Imm. 175: 5575, 2005)
By now, a host of subtypes are known, and they tend to appear a few years before the symptoms (Arth. Rheum. 65: 899, 2013). There has been talk about the anti-CCP's being etiologic. Stay tuned.
It also seems that anti-TNF-alpha agent stop the production of anti-CCP, directly or indirectly, and this may be one way in which they work (Ann. NY Acad. Sci. 1051: 559, 2005).
Of course the anti-CCP antibodies are also present in the synovial fluid in different forms (Arth. Rheum. 62: 1620, 2010).
* An early report is that the "shared epitope" HLA-DRB1 alleles predict that one will develop anti-CCP, rather than one will develop arthritis (Arth. Rheum. 54: 1117, 2006). First-degree relatives of rheumatoid arthritis patients often have IgA anti-CCP; they tend to have the shared epitope, to be smokers, and to have some joint problems (Arth. Rheum. 65: 1439, 2013).
There are several specificities; the new point-of-care screen for rheumatoid arthritis combines rheumatoid factor and anti-mutated citrullinated vimentin.
* Watch a new system of autoantibodies in rheumatoid arthritis -- the anti-carbamylated protein (anti-CarP) antibodies that are related to joint destruction (Arth. Rheum. 65: 911, 2013).
ANTI-NUCLEAR ANTIBODIES ("ANA's"): Pathology evidence-based consensus document Arch. Path. Lab. Med. 124: 71, 2000. Simple update: J. Allerg. Clin. Imm. 117(2): S-445, 2005.
| RIM PATTERN |  |
Probably anti-dsDNA. Your patient probably has SYSTEMIC LUPUS. |
| HOMOGENEOUS PATTERN |  |
Probably anti-histones / anti-chromatin. Your patient probably has DRUG-INDUCED LUPUS. |
| SPECKLED PATTERN |  |
Could be anti-Sm and/or anti-Ro/SSA and/or anti-La/SSB and/or anti-U1snRNP and/or any of several others, or nothing at all that anybody knows. You'll need to decide whether to continue your workup! |
| CENTROMERE PATTERN |  |
An especially fine speckling with little background staining. This is anti-centromere, the marker for CREST / pulmonary hypertension. |
| NUCLEOLAR PATTERN |  |
anti-Th/To or anti-fibrillarin / anti-U3snRNP or anti-U17RNP. Think of SCLERODERMA, though most scleroderma patients don't show the nucleolar pattern. |
All sorts of information about ANTI-NUCLEAR ANTIBODIES (ANA) is available in the references and the literature for the extremely curious student. As a resident, this was one of my favorite areas of "clin path". With the "new biology" (recombinant DNA and monoclonal antibodies), the various tests for autoantibodies are becoming more sensitive and more specific for particular diseases. Use these judiciously -- for the most part, they are neither sensitive nor specific (the many pitfalls: South. Med. J. 98: 703, 2005). The most helpful test is still your history and physical exam.
Old tests for antinuclear antibodies used fluorescence to detect antibodies stuck to real mammalian nuclei ("rat liver test"; "mouse kidney test"; newer tests are done on human epithelial cells -- "HEp2 test"). These are still the screening tests. (And they're for screening: Postgrad. Med. 94: 55, 1993). As you have guessed, differences in substrate account for the great variability among different labs. New tests for specific antinuclear antibodies are mostly tube tests; there are now kits that will do enzyme immunoassays for many different ANA's at once (update J. Clin. Path. 64: 631, 2011).
RULE: In dealing with anti-nuclear antibody tests, the higher the titer, the more likely it is to mean something.
You already know how to do an LE-cell prep, which begins best with a clumsy phlebotomy. It is a cheap, easy way to detect a presently-uncharacterized antibody or antibodies against something on the nucleus.
* We think that there is no longer any indication for an LE-cell prep, unless you want to do it yourself for your own interest. There are rare reports of LE-positive, f-ANA-negative lupus victims, but tube tests should pick these patients up (Am. J. Clin. Path. 101: 65, 1994).
* When lupus is treated with TNF-receptor blockers such as infliximab, the autoantibodies often rise transiently and this does not herald an exacerbation (Arth. Rheum. 56: 274, 2007).
Fluorescent ANA (f-ANA) titers for the older test:
1:20 or less... "negative"
1:40 to 1:160... infections, "one organ autoimmune diseases", normals (especially oldsters, and perhaps 10% of healthy children and adolescents: Clin. Ped. 43: 637, 2004), some "collagen-vascular diseases"
Above 1:160... "collagen-vascular diseases"
The only real INDICATION for an f-ANA is when you have some reason to suspect:
Worth remembering: Among patients with a positive ANA ordered to screen for lupus or some other autoimmune disease and sent to a rheumatology specialty clinic, 90% will have no rheumatologic or other disease for which a positive ANA is typical (Am. J. Med. 126: 342, 2013).
* It's likely that the fluorescent-ANA will be replaced, at least in some settings and especially when it's being ordered as part of a fishing expedition, by a group of tests for individual autoantibodies (Am. J. Clin. Path. 138: 551, 2012).
If the f-ANA comes back positive, and you think this is lupus, consider these tests:
(1) an ANTI-DOUBLE-STRANDED DNA ANTIBODY (anti-dsDNA, formerly "anti-native DNA").
![]() Anti-nuclear antibodies
Anti-nuclear antibodies
Crithidia
These are pathogenic (for example, J. Imm. 151: 1128, 1993; Arth. Rheum. 36: 355, 1993), quite specific for lupus, and are present in high titer in around half untreated systemic lupus patients. (* Beware: extreme cases where there is antigen-excess or antibody-excess in the serum). The wire loops have ds-DNA and its antibody in them.
Titer of anti-ds-DNA is a good way to follow disease activity and predict exacerbations; a rise in titer commonly precedes a flareup.
* Future pathologists: Several testing methodologiest exist, and do not always agree. A "Crithidia test" (a leishmania with an easy-to-stain blobbie of ds-DNA) may give quite a different result for a particular serum than does a binding asssay (Ann. Rheum. Dis. 63: 386, 2004).
* Intriguing study: Dogs owned by lupus patients are much more likely to have anti-dsDNA on board (Lancet 339: 1378, 1992).
* For some reason, rheumatoid arthritis patients treated with infliximab, the antibody against tumor necrosis factor, commonly develop anti-ds-DNA antibodies that however do not seem to produce symptoms (Arthr. Rheum. 43: 2383, 2000.)
(2) a SERUM C3. It should be low in active systemic lupus (it's usually normal in rheumatoid arthritis). So are SERUM C4 and SERUM CH-50 (see below) You may use these to follow disease activity.
(3) for confirmation, an ANTI-SM and/or ANTI-RO.
ANTI-SM ANTIBODY is a tube test. This is not very sensitive (30%), but quite specific for lupus (and somewhat ominous). ANTI-RO (formerly "anti-SSA") is not very sensitive and not very specific, but warns of photosensitivity, sicca, thrombocytopenia, and especially heart block in the unborn (Circulation 124: 1919, 2011) or newborn (Circulation 124: 1927, 2011) child; using the older substrate, it was used to support a diagnosis of lupus in old "ANA-negative" cases.
If the f-ANA comes back negative, and you still think this is lupus, consider these tests:
Remember this is very uncommon nowadays. If the lab was using the old-fashioned test, order an ANTI-RO/SSA and consider other tube tests. You'll be using the list of criteria to make the diagnosis. You may also order an ANTI-EXTRACTABLE NUCLEAR ANTIGEN (anti-ENA; anti-ENA4) assay, a possible lupus-and-others marker that modern fluorescent ANA testing misses: Medicine 84: 208, 2005; J. Clin. Path. 54: 187, 2001; Medicine 84: 208, 2005 -- the anti-ENA panel will often light up anti-Sm, anti-RNPs, anti-Ro and anti-La better than a f-ANA.)
ANTI-HISTONE ANTIBODY ("anti-chromatin") is a marker for drug-induced lupus (hydralazine, isoniazid, procainamide, phenytoin.)
This is supposed to be 100% sensitive, but not really specific; up to 70% of patients with regular lupus will have at least one anti-histone antibody, and they pop up in plenty of other autoimmune diseases (* notably morphea: Arth. Rheum. 36: 1137, 1993). Plus, how is the test going to help guide therapy? We don't really recommend doing this.
Over half the patients you put on hydralazine or procainamide will become f-ANA-positive, but only around 10% will get sick.
You can biopsy a piece of normal-looking skin and ask the pathologist to check for immunoglobulins and complement components along the dermal-epidermal junction (THE LUPUS BAND TEST). This suggests systemic lupus, but interpretation is complex. (See Arthr. Rheum. 27: 382, 1984). Send sun-exposed, non-rash skin if you want a diagnosis.
{33205} positive lupus band test
* ANTI-RIBOSOMAL P antibodies are discredited as a test for lupus psychosis, but are fairly specific (though not sensitive) for lupus.
* ANTI-DNP (deoxyribonucleoprotein) is a known marker for lupus and scleroderma that is not much used except by researchers, but has been a subject of ongoing interest.
Whether or not you have established a diagnosis of lupus, a high f-ANA titer or LE-cell in an effusion suggests the cause is lupus.
If you have established the diagnosis for lupus by any means (remember there are clinical criteria), you can "follow the disease activity and its response to your treatment" with serial f-ANA's, C3's, C4's, etc.
ANA and anti-dsDNA titers tend to drop after effective treatment (see Arthr. Rheum. 29: 26, 1986). Complement components rise to normal levels. However, why are you ordering this?
The classic CH-50 assay for complement was a measure of the titer of complement required to hemolyze 50% of a standardized preparation of IgM-coated RBC's. Its main use today is to check for specific complement component deficiencies -- where C3 is normal but CH-50 is very low.
* ANTI-NUCLEOSOME ANTIBODIES (anti-nuc / anti-ncs) suggest lupus (Rheumatology 43: 220, 2003) but they've never become popular for diagnosis; curiously they may appear in rheumatoid arthritis treated with anti-TNF agents (Clin. Rheum. 27: 91, 2008).
ANTI-RIBONUCLEOPROTEIN ANTIBODIES (anti-nRNP, anti-U1-snRNP etc.) is always present in high titer in "mixed connective tissue disease" (anti-U1-snRNP disease, i.e., Raynaud's, swollen fingers, arthritis, mild myositis). Order it if (and only if) you suspect this illness. It is often is positive at low titer in systemic lupus, * scleroderma, and even * healthies (Arch. Derm. 123: 601, 1987).
* Components of the snRNP antigen include U1 and U2, which seem linked to MCTD (U1), psoriasis and Raynaud's (NEJM 315: 105, 1986), and fibrillarin, which is common in and fairly specific for scleroderma. U1 is part of the splicosome, coded by SNRNP70.
* Anti-U1snRNP can cause neonatal lupus, just like anti-Ro can (Arch. Derm. 128: 1490, 1992). It is less severe. Anti-U1snRNP heart block in adults: Arth. Rheum. 32: 1170, 1989.
ANTI-SCL-70 ANTIBODY (* anti-DNA-topoisomerase I) is an antibody against an alkaline, nonhistone nuclear protein. It is positive only in about 20% of patients with diffuse scleroderma. It is very specific, and suggests a relatively bad prognosis. Consider ordering this if you believe your patient is coming down with scleroderma.
* ANTI-RNA POLYMERASE (anti-RNAP I, II, and/or most famously III) are common in diffuse scleroderma and are now into clinical use (Arth. Rheum. 42: 275, 1999; Arth. Rheum. 52: 2425, 2005; Rheumatology 47: 976, 2008 -- anti-RNA polymerase III is available as anti-ARA).
ANTI-CENTROMERE ANTIBODY (* really "anti-kinetochore antibody") is a sensitive and (in high titer) specific marker for CREST syndrome (Mayo Clin. Proc. 59: 708, 1984). This has stood the test of time (though it no longer defines the disease, as was once proposed), and is also present in the animal model ("the tight-skin mouse": J. Imm. 175: 2418, 2005). With today's f-ANA substrates, the anti-centromere pattern is obvious and there is perhaps no need for a tube test.
ANTI-RO/SSA ANTIBODY is an anticytoplasmic autoantibody that occurs in nearly all patients with Sjogren's syndrome; high titers can cause a vasculitis. Low titers occur in other autoimmune diseases and normals.
Neonatal lupus (i.e., rash/heart block) is usually caused by Mom's anti-SSA/Ro. Discovery NEJM 312: 98, 1985; update on these kids, who are likely to be permanently damaged is the illness is severe Pediatrics 121: e803, 2008.
Anti-Ro is also the key player in subacute cutaneous lupus, with the non-scarring bumps on sun-exposed areas.
Anti-Ro can produce a multiple-sclerosis-like picture. Nobody really understands how.
* Researchers subclassify anti-Ro's (anti-Ro 52, anti-Ro 60).
ANTI-LA/SSB ANTIBODY is an anticytoplasmic autoantibody that is seen in patients with primary Sjogren's. Patients with anti-SSB always have anti-SSA by the old tests, since LA is a component of the "Ro/La" group of molecules. The newer version of this test appears to be the best seromarkers for primary Sjogren's (Autoimmunity 38: 55, 2005. Having anti-Ro and/or anti-La is now one of the criteria for diagnosis ("you need four of the following six...")
ANTI-JO-1 and several other markers for polymyositis-dermatomyositis are antibodies against transfer RNA synthetases for specific amino acids.
* Other antibodies that may produce slightly different myopathies are anti-Mi-2 and anti-SRP (Arth. Rheum. 50: 209, 2004). They are still of research interest only. Anti-Ku is an antibody that runs with corticosteroid-sensitive inflammatory myopathy and corticosteroid-resistant interstitial lung disease (Medicine 91: 95, 2012).
Anti-Jo is a fair marker for polymyositis-dermatomyositis lung disease, and a good marker for the subluxing arthropathy (Arth. Rheum. 33: 1640, 1990). Today, the tendency is to call this "anti-Jo syndrome" (Autoimmunity 39: 243, 2006), and titers of anti-Jo, when present, correlate with the severity of the "idiopathic inflammatory myopathy" (Arth. Rheum. 56: 3125, 2007). Consider ordering this if you suspect or have diagnosed polymyositis / dermatomyositis.
ANTI-PM/SCL seems to define a scleroderma-polymyositis overlap syndrome (Arth Rheum. 50: 565, 2004; this is holding up Arth. Rheum. 66: 1608, 2014.)
* More anti-nuclear antibody subtypes exist. During the past twenty years, I've watched claims made for anti-single-stranded DNA antibody (localized scleroderma / morphea), anti-proliferating cell nuclear antigen (anti-PCNA), anti-RA33 (a discredited marker for rheumatoid arthritis), anti-DEK (immune iridocyclitis), anti-H3 (lupus-like syndrome), anti-centriole (scleroderma), anti-nucleolar antibody tube test (scleroderma), anti-heatshock protein 90 (anti-HSP90; wide claims), anti-nuclear matrix antibody (wide claims), and a host of others all fail to find clinical usefulness.
{29557} ANA, speckled pattern
{33154} ANA, rim pattern
{33248} ANA, nucleolar pattern
{08457} ANA, nucleolar pattern
| TEST |
|
|
|
Tapping the joint |
Consider doing this especially when there is a hot joint with an effusion | Heparin tube for crystals and CBC-diff;
Plain tube(s) for viscosity, mucin clot, complement, glucose, gram stain, and culture
|
|
* Synovial fluid complement |
Acute lupus, acute RA |
Likely to be low in active autoimmune disease.
|
|
* Synovial fluid RF |
Early adult RA |
Becomes positive before serum RA. Limited usefulness.
|
|
Serum rheumatoid factor |
Adult RA |
75% of adult RA's will be positive Many positives in old age, SLE, SBE, syphilis Negative in juvenile arthritis, osteoarthritis, others
|
|
* Serum IgG RF |
Adult RA |
Available. Of doubtful value.
|
|
* Serum anti-RANA |
Adult RA |
Old test based on the idea that Epstein-Barr
|
|
Serum f-ANA |
Those multi-organ autoimmune diseases |
Screening test. Titers 1:20 to 1:160 are nonspecific. Rim: Classic lupus Speckled: Classic lupus, Sjogren's, MCTD, others Homogeneous: Drug-induced lupus Nucleolar: Scleroderma ... again, this is NOT specific (J. Clin. Path. 61: 283, 2008)
|
|
Serum anti-dsDNA |
SLE |
Same as anti-nDNA and anti-DNA. Higher titers are very specific for lupus. Rising titers predict an exacerbation. Titers fall on successful treatment. Now being seen after infliximab therapy also. Stay tuned.
|
|
Serum C3 |
SLE |
Usually low in lupus; of course this is not specific. Value rises to normal on successful treatment
|
|
Serum anti-Sm |
SLE |
Very specific for lupus, positive in 30% of cases.
|
|
Serum anti-histone |
Drug-induced lupus |
Most patients with this antibody remain asymptomatic. A negative value pretty much rules out drug-induced lupus.
|
|
Lupus band test |
SLE |
Requires skin biopsy. Becoming obsolete
|
|
Serum anti-snRNP |
Mixed CT disease |
All MCTD's positive, low titers in other diseases. Ask whether the lab can give you just an anti-U1.
|
|
* Serum anti-centriole |
Scleroderma |
Promoted as positive in some patients with scleroderma; not much used nowadays
|
|
Serum anti-centromere |
CREST |
High titer defines CREST syndrome
|
|
Serum anti-SSA (-Ro) | Sjogren's |
Often positive but not specific. This is the autoantibody that causes neonatal lupus with heart block.
|
|
Serum anti-SSB (-La) | Sjogren's |
Often positive but not specific
|
|
* Serum anti-adrenal |
Autoimmune Addison's |
Helps rule out other causes of Addisonism. The antigen is (at least usually) 21-hydroxylase.
|
|
* Serum anti-islet-cell |
New or impending DM type I |
Usually positive, doubtful clinical usefulness
|
|
Serum anti-insulin receptor |
Type II diabetes variant |
Insulin resistance caused by blocking autoantibody
|
|
Serum anti-sperm antibodies |
Infertility |
Husband or wife
|
|
Serum anti-AchR |
Myasthenia gravis |
Anti-acetyl cholinesterase receptor. The first test to order in suspected MG. * False positives occur in patients injected with bungarotoxin (cobra venom, quack remedy)
|
|
Serum anti-AchR Blocking Ab |
Myasthenia gravis |
Order in suspected MG if Anti-AchR is negative
|
|
* Serum anti-striational ab's (StrAbs; anti-titin, anti-ryanodine reeptor) |
Myasthenia gravis, thymoma is usually present |
If negative in MG, some surgeons will not remove thymus. See Arch. Neurol. 62: 442, 2005.
|
|
* Serum Kv1.4 (potassium channel) |
Myasthenia gravis |
New possible marker for more serious disease (Arch. Neuro. 64: 1121, 2007)
|
|
Serum anti-GBM |
Goodpasture's |
A few false negatives. If the pathologist who does the test isn't experienced, there will be lots and lots of false positives.
|
|
Serum anti-tubular BM |
Renal interstitial disease |
Anti-TMB disease is an important, under-recognized cause of acute interstitial nephritis.
|
|
* Serum anti-intrinsic factor |
Pernicious anemia
|
Probably worthless, less sensitive and less specific than a Schilling test
|
|
* Serum anti-parietal cell abs |
Pernicious anemia |
Probably worthless, less sensitive and less specific than a Schilling test
|
|
Schilling test |
Pernicious anemia etc. It's a shame when the reagents aren't available -- here's hoping this good test will be re-instituted |
Step 1: Give your patient radioactive vitamin B12 by mouth. See how much
comes out in the urine. If very little comes out in the urine, your patient can't absorb straight
vitamin B12 (pernicious anemia, fish tapeworm, or ileal disease).
Step 2: If your patient just proved he or she cannot absorb straight vitamin B12, repeat the test by administering a mix of vitamin B12 and intrinsic factor. If, this time, the patient excretes more of the vitamin B12 in the urine, you have established the diagnosis of addisonian pernicious anemia. Check your protocol. You'll probably want to administer an injection of vitamin B12 before the test, since you don't want the patient actually storing the radioactive substance.
|
|
Platelet-associated Ig |
Immune thrombocytopenia |
Idiopathic thrombocytopenic purpura, also SLE, AIDS
|
|
Serum anti-skin |
Blistering diseases |
Inter-epithelial antibodies: Pemphigus vulgaris Dermal-epidermal junction: Bullous pemphigoid Reticulin: Dermatitis herpetiformis (biopsy it instead!)
|
|
* Serum anti-reticulin * Serum anti-endomysium * Serum anti-gliadin |
Sprue / dermatitis herpetiformis |
Nowadays some clinicians omit small bowel biopsy
when these are positive, and move right to
the gluten-free
diet trial.
|
|
* Anti-collagen (I, IV, etc.) | Various joint diseases | Research interest only; nothing's really come of these in humans despite decades of work. |
|
Serum anti-smooth muscle |
Lupoid hepatitis 1 |
Only high titers are significant, low titers occur in many diseases
|
|
Serum anti-LKM1 ("liver kidney microsome") |
"Lupoid hepatitis" 2 | Defines the illness
Anti-liver-kidney-microsome disease.
|
|
Serum anti-mitochondrial |
Primary biliary cirrhosis |
Sensitive and specific, but only high titers are significant health threats
|
|
* Serum anti-myocardial |
"Dressler's" |
Completely out of use. The existence of Dressler's is very much in doubt anyway.
|
|
Serum anti-streptococcal |
Glomerulonephritis, rheumatic fever. Several tests are available, ask you lab ("ASO", "anti-hyaluronidase" are popular). They will be positive by the time your patient has rheumatic fever or glomerulonephritis.
|
|
* Serum anti-teichoic acid | This used to be
used to monitor the treatment of osteomyelitis, but is now completely out of
use which is fine (Ped. Inf. Dis. J. 17: 1021, 1998)
|
|
Serum anti-neutrophil cytoplasmic antigen |
Wegener's, polyarteritis |
Anti-myeloperoxidase (p-ANCA, p-ACPA) causes many cases of polyarteritis (the "small vessel" variant, now clearly a distinct disease from "classic polyarteritis nodosa"). You'll also see it in most patients with the combination of sclerosing cholangitis and ulcerative colitis.
Anti-proteinase 3 (c-ANCA, c-ACPA) is closely linked to Wegener's granulomatosis. You can see these in various systemic autoimmune diseases; whatever the "underlying systemic vasculitis. Certain nonspecific ANCA's probably result from longstanding inflammation, as in rheumatoid arthritis (Art. Rheum. 36: 994, 1993).
|
|
Serum C' esterase inhibitor |
Hereditary angioedema |
Ask for both level and functional assay
|
|
Serum complement components |
Deficiency states |
Deficiencies of C1q, C1r, C1s, C4, C2, C5, and/or C8 simulate SLE
Deficiency of C6, C7, C8 have recurrent neisserial infections In seeking out genetic birth defects, ask for both level and functional assay. You can of course also use C3 and C4 to monitor the course of lupus.
|
|
Serum CH-50 |
Screening test for all complement component deficiencies ("titer that hemolyzes 50% of the test red cells") |
Has also been used to follow the course of SLE
|
|
Nitroblue Tetrazolium test |
Chronic granulomatous disease (i.e., the neutrophil killing defect) |
Hereditary immunodeficiency syndrome with defective killing of
staphylococci
|
|
Serum anti-allergen IgE |
Food or penicillin allergy |
"RAST", supposed to replace skin tests, expensive.
|
|
* Raji cell assay |
Circulating immune complexes |
Limited usefulness
|
|
HLA-B27 |
Ankylosing spondylitis, etc. |
Classic example of a result that is unlikely to affect patient management
|
|
* Von Willebrand factor |
Vasculitis |
In patients who do not have von Willebrand's disease but who do have some kind of serious systemic vasculitis (lupus, polyarteritis nodosa, Wegener's, Henoch-Schonlein, and so forth), levels of vWFAg are likely to be elevated (why? Arch. Dis. Child. 70: 40, 1994)
|
|
* Thrombomodulin |
Vasculitis |
Endothelial thrombin receptor. Serum levels increase in vasculitis (Am. J. Clin. Path. 101: 109, 1994)
|
|
Complement 3 nephritic factor |
Membranoproliferative glomerulonephritis types I and (now) II |
Pathogenic; helps establish the diagnosis
|
|
"Heterophile antibodies" |
Many inflammatory diseases |
Agglutinate sheep red cells. Nobody orders this test.
|
|
Forsmann antibodies |
Many inflammatory diseases |
Heterophile antibodies that are absorbed by guinea pig kidney but not by beef RBC's. Nobody orders this test.
|
|
Mono test ("Mono-spot") | EB-virus infectious mono |
Heterophile antibodies that are absorbed by beef RBC's, not by guinea pig kidney. Cheap test, sensitive and specific, but often remains negative for many weeks, often never turns positive in children
|
|
Expensive, high titers suggest current infection. This is the test to order
if the "Mono-spot" is still negative but you still suspect EBV mono.
|
|
Current EBV infection |
Sensitive and specific, very useful in children
|
|
Early or chronic EBV disease |
Ask your infectious disease expert whether these tests are useful.
|
|
Remember these too in "infectious mononucleosis"; "post-viral fatigue syndrome"
|
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about arthritis labs to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
| New visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
