Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.

|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected. No texting or chat messages, please. Ordinary e-mails are welcome.
 I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
at www.afraidtoask.com.
I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
at www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles that you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
Once again, this is absolutely essential material. Given any of the definitions, you should be able to supply the word. Given any of the processes, you must be able to explain "how", "when", "where", and "why".
Describe the processes that give rise to transudates, and those that give rise to exudates.
Describe edema as seen in inflammation, heart failure, liver failure, and kidney failure. Describe the special cases of cerebral edema and "angioedema". Explain how lymphedema develops.
Describe in general terms the causes and consequences of hemorrhages.
Cite Virchow's triad for the causes of thrombosis, and recognize and give examples in each category. Explain why turbulent flow promotes thrombosis, why damaged endothelium promotes thrombosis, and how blood can become hypercoagulable. Describe the possible fates, good and bad, of a thrombus.
Describe the nature, causes, and significance of disseminated intravascular coagulation, and give its synonyms.
Describe things that embolize. Briefly discuss classic pulmonary thromboemboli, paradoxical emboli, and systemic thromboemboli. Give an account of the causes and consequences of amniotic fluid, air, fat, atherosclerotic, marrow, tumor, and therapeutic emboli.
Give a full account of the various types of infarcts. Mention two factors contributing to "reperfusion injury".
Define shock, and mention its major causes. Describe how whole-body hypoperfusion causes problems. Discuss the physiology of shock, and describe its stages (compensated, progressive, and irreversible). Describe the anatomic pathology that results from fatal shock. Tell how prolonged compensated shock affects the whole person.
Use the following terms correctly, and produce the term given a definition or description:
|
 Fluid and Hemodyamic "Bringing Out the Dead" |
Recognize the following gross items:
a patient with anasarca
a liver or lung with congestion
a brain with hydrocephalus
an ante-mortem thrombus, anywhere
a pulmonary thromboembolus
petechiae, ecchymoses, and other bleeds
infarcts in brain, heart, gut, and solid viscera
Be sure you can recognize the following under a microscope, with or without other pathologic lesions:
protein-rich edema fluid
ante-mortem thrombi
post-mortem thrombi
DIC microthrombi
marrow emboli
![]() KCUMB Students
KCUMB Students
"Big Robbins" -- Hemodynamic
Lectures follow Textbook
QUIZBANK
Hemodynamic 31-113, 198-251
* As he was dying of alcoholic liver disease, W.C. Fields was told he had excessive accumulation of water in his abdomen. He replied, "I knew that insipid, tasteless fluid would be the death of me!"
LEARN FIRST
EDEMA is excess interstitial fluid, for whatever reason. TRANSUDATES are fluid accumulations that are essentially salt-water, accumulated because of pressure problems. EXUDATES are protein-rich fluid accumulations, due to leaky vessels.
THROMBI, or blood clots within the vessels or heart, form when the blood flow is abnormal (turbulent or static), or the blood is too coagulable, or the endothelium of the vessels is damaged. Thrombi are said to EMBOLIZE when they break free and sail downstream to obstruct a vessel.
An INFARCT is an area of tissue that has died because its vascular supply was suddenly occluded. VENOUS INFARCTS result when veins can no longer drain an organ, and they tend to be very bloody. ARTERIAL INFARCTS may be bloody (red) or not (white), depending on whether blood leaks back into the dead tissue (collaterals / dual supply; reperfusion) after the damage is done.
In DISSEMINATED INTRAVASCULAR COAGULATION, the clotting cascades are activated throughout the body. This is bad, since it tends to shut down organs due to microthrombi, and also causes bleeding due to consumption of clotting factors and activation of plasmin. ("Thrombin and plasmin are both being activated" is a common, simplistic account that you may hear.)
SHOCK is the inability to adequately perfuse the whole body, for any reason. Shock is likely to deteriorate into a vicious cycle of organ failure and subsequent exacerbation of shock resulting in death.
|
|
|
|
|
|
|
|
|
|
|
EDEMA
This is a generic term for too much interstitial ("intercellular") fluid.
Contrast "cell swelling" or "intracellular edema". You are already familiar with this hallmark of cell injury.
Edema may be localized or generalized. Bad generalized edema is called ANASARCA.
|
|
|
Some definitions of edema also include excess fluid in the body cavities ("third space" -- normally, these cavities contain <50 mL or so of fluid). Most people call these EFFUSIONS. More words to learn now:
ASCITES: Excess free fluid in the peritoneal cavity
![]() Ascites in a cirrhotic
Ascites in a cirrhotic
From a gastroenterologist
in El Salvador. Great photos.
{19381} ascites
HYDROTHORAX ("pleural effusion"): excess free fluid in a pleural cavity. If it's pus, it's called an EMPYEMA instead, (less often, PYOTHORAX). If it's blood, you must call it HEMOTHORAX instead.
HYDROPERICARDIUM ("pericardial effusion"): excess fluid in the pericardial cavity.
HYDROCEPHALUS: Increased volume of cerebrospinal fluid from any cause; dilated cerebral ventricles. More about this at the end of the course.
{13394} hydrocephalus
{13395} hydrocephalus
![]() Hydrocephalus, untreated
Hydrocephalus, untreated
From a Saddam-era Iraqi
propaganda website (!)
HYDROCELE: Excess fluid in the space around the testis
![]() Hydroceles
Hydroceles
Photo series
Vesalius
HYDROSALPINX: A dilated oviduct full of non-inflammatory fluid
ILEUS: excess fluid within the small bowel; dilated bowel segments.
SEROMA: Accumulation of non-infected fluid in a tissue space made by surgery, especially the incision.
LOCULATED EFFUSION: an effusion divided into more than one compartment, generally by scar tissue. A problem for the physician who wishes to drain the fluid using a needle.
BLISTER: fluid within the epidermis, or between epidermis and dermis. A little blister is a VESICLE, while a big blister is a BULLA.
There is no need to review the volumes of the various body fluid compartments, or their physiology, here. Between cells or in body cavities, accumulations of fluid can be TRANSUDATES or EXUDATES.
TRANSUDATES, as you remember, are basically accumulations of salt water, with very little protein content. They result when hydrostatic pressure pushing salt and water out of normal vessels (total fluid volume, pressures in the microcirculation) exceeds the osmotic "force" of serum albumin (and other proteins) pulling the fluid back into the normal vessels, plus the ability of the lymphatics to drain the fluid (and the traces of protein that leave the vessels in health). What causes transudates?
Excess total body fluid
Salt and/or fluid overloading (self, iatrogenic)
Excess aldosterone (tumor, liver failure, other)
Kidney failure
Pre-renal
Heart failure
Prolonged hypotension
Antihypertensive therapy (notoriously calcium channel blockers)
Renal: Intrinsic kidney disease
Post-renal: Urinary obstruction
Vascular problems
All systemic veins
Right-sided heart failure
Most pericardial disease
Pulmonary veins
Left-sided heart failure
Leg veins
Prolonged standing
Pregnancy ("pressure of the uterus", estrogen)
Valve failure
Portal vein
Cirrhosis and certain other liver diseases
Obstruction or narrowing of specific veins
External pressure
Thrombi
Cerebral microcirculation (mysterious but deadly)
Brain trauma or other intracranial catastrophe
Lead poisoning
Other causes of damaged blood-brain barrier
Systemic microcirculation (angioedema)
C1-esterase inhibitor deficiency
Cyclic angioedema
ACE inhibitors (rare)
Decreased plasma protein content
Protein malnutrition
Malabsorption / protein losing enteropathies
Hepatic insufficiency
Severe urinary protein wasting ("nephrotic syndrome")
Lymphatic obstruction ("lymphedema")
Inflammatory scarring (especially from filariasis)
Cancer
After surgery (archaic mastectomies, etc.)
After irradiation
* Congenital defects in the lymphatic structure ("Milroy's disease")
Major mystery-mechanisms of medicine
Fat emboli produce pulmonary edema
* Sleep apnea (accounted for many of the old "idiopathic" cases -- Sleep Med. 5: 583, 2004)
In clinical practice, generalized edema is usually due to heart failure, cirrhosis of the liver, nephrotic syndrome, or salty-food overindulgence by people with marginal kidney function. The worst generalized edema is seen in severe hypoproteinemia (typically from the nephrotic syndrome).
Note that the causes of edema in a particular clinical situation are often complex.
In heart failure, the venous hydrostatic pressure increases, the under-perfused kidneys retain fluid, and increased intravascular fluid puts a further strain on the heart.
In cirrhosis, the pressure in the portal vein is increased ("obstruction by scarring", abnormal communications between branches of the hepatic artery and portal veins -- leading to ascites), the liver fails to synthesize albumin, and the liver fails to break down aldosterone.
In nephrotic syndrome, the blood volume eventually becomes low, and the kidney responds by retaining sodium.
Despite what "Big Robbins" once said, dilatation of the arterioles ("hyperemia") does NOT result in appreciable edema.
LYMPHEDEMA (i.e., edema due to obstruction of the lymphatic vessels.
When lymphedema involves the extremities, it can be striking, producing ELEPHANTIASIS. The textbook cause is filaria worms. Cancer of the cervix invading the pelvic lymph nodes is another important cause.
PODOCONIOSIS is elephantiasis of the lower extremities caused by longstanding shoelessness where the soil is volcanic. The glass-like particles penetrate and clog the lymphatics (Lancet 369: 888, 2007.)
Iatrogenic lymphedema still is an important problem following surgery / radiation for breast cancer (BMJ 342: d3442, 2011).
{08295} elephantiasis of leg, filariasis patient
{08259} elephantiasis of scrotum, filariasis patient
|
Obstruction of the pulmonary lymphatics by cancer is a common mechanism of death in cancer patients. Obstruction of lymphatics in the breast by a cancer produces "orangepeel skin", an ominous sign.
|
|
While we're at it... CHYLOUS EFFUSIONS result from leaking lymphatics, usually from trauma or cancer involving the thoracic duct. It'll look milky from the chylomicrons. (Future pathologists: an old exudate can look milky too, hence the term "pseudochylous.")
EXUDATES, as you remember, are protein-rich accumulations of salt water. They result when vessels leak protein (which carries water) into the interstitial fluid or third space. They may be due either to inflammation, to mild vascular injury (the familiar example is sunburn), or to abnormal vessels within tumors.
You will have many opportunities to observe edema in the clinic.
CARDIAC EDEMA involves the whole body. (If the left ventricle is okay but the right ventricle is out of order, the lungs will be spared). Since the primary problem is hydrostatic pressure, cardiac edema is worst in the more dependent portions of the body, and begins to move whenever the patient changes position. For patients standing up, look over the backs of the feet for "pitting edema". For the bedridden, check over the sacrum; check a man's scrotum. Depending on the cause, listen to the lungs for CRACKLES (formerly "rales") -- the snap, crackle, and pop of fluid bubbles in the alveoli.
RENAL EDEMA also involves the whole body. This time, since the heart is working fine and the problems are fluid overload and/or hypoproteinemia, the edema is generalized. Look first around the eyelids. (Again, listen to the lungs.)
PULMONARY EDEMA, a familiar problem, causes patients to cough up froth when the edema fluid escapes into the alveoli. At autopsy, we see heavy lungs, with frothy fluid running from their cut surfaces.
![]() Pulmonary Edema
Pulmonary Edema
Text and photomicrographs. Nice.
Human Pathology Digital Image Gallery
CEREBRAL EDEMA causes massive swelling of the brain, which is especially unwholesome since the brain is confined within a bony skull. At autopsy, the brain is heavy, the gyri are flattened against the skull, and often portions of the brain have been pushed out of their normal positions.
* In college, a communist assured me that Trotsky must have been a great thinker because he had such a heavy brain. His high brain weight was more likely due to his having died a few hours after having his skull shattered with an axe.
ANGIOEDEMA results from vessels becoming over-permeable. Outstanding among known causes is C1-esterase inhibitor deficiency, which you'll study later; this is especially serious when it affects the larynx.
OTHER LOCALIZED EDEMA needs no further description.
Under the microscope, a pathologist can appreciate edema because it spreads the connective tissue fibers. We will not expect you to recognize this.
HYPEREMIA AND CONGESTION: The two possible reasons for increased blood volume in a particular part of the body.
HYPEREMIA ("active hyperemia", a redundancy) is increased blood flow to an organ, resulting in increased blood content. This happens when the arterioles have dilated more than its venules have dilated.
Examples are blushing, erections (red and throbbing), reddening of skin to disperse heat, and "rubor" of acute inflammation.
CONGESTION ("passive congestion", another redundancy) is decreased blood flow from an organ, resulting in increased blood content. This happens when something is interfering with the organ's venous drainage.
Congestion can result from any and all the "vascular problems" that produce transudates. This can include anything from an over-tight necktie to a failing heart to erections (purple and swollen). See above. Or the blood may be hyperviscous (too much IgM, too many red cells).
Congested organs ooze excess blood when cut. Longstanding congestion is likely to result in a few microhemorrhages (or at least with "diapedesis of red cells through the capillary walls"), and abundant hemosiderin-laden macrophages ("heart failure cells", at least in the lungs) confirm that congestion has been present for at least a few days.
{10967} heart failure cells in the lung
Certain organs ("fibrocongestive spleen", "brown induration of the lung") show classic changes in longstanding congestion.
NUTMEG LIVER, with congested red centrilobular areas and lighter portal areas, is a gourmet term for a ubiquitous autopsy finding (blood pools in the liver as the heart dies; ask to see Dr. Friedlander's bisected nutmeg). Longstanding extreme hepatic congestion (i.e., usually from a tricuspid valve that will not close) can lead to scarring around the central areas; I have never seen true "cardiac cirrhosis".
{00029} nutmeg liver
{31889} real nutmeg
|
|
|
* Despite R&F, we believe that Gamna-Gandy bodies in the spleen represent healed venous infarcts, not just the sequelae of congestion.
* Somebody will probably tell you that "congestion of the liver causes centrilobular necrosis" ("the patient's liver enzymes are up because of congestion", etc., etc.) This is silly. What's really happened is that the patient's last hours were spent with a failing circulation. The cells in the centers of the hepatic lobules died because they are the ones farthest from the oxygenated blood supply. The red cells pool nearest the veins that lead back to the failing heart. These happen to be the same place. The congestion did not cause the necrosis, or vice versa.
We consider "passive hyperemia", an old term for congestion favored by R&F, to be bad usage. Note that "nasal congestion" that accompanies a cold is hyperemia and/or edema, while "congested sinuses" are filled with effusions.
{07554} petechiae on eye, strangulation victim
{14287} petechiae on legs
{08059} petechiae on heart, leukemia case
{21433} petechiae on oral mucosa
|
|
|
PURPURA: Bigger hemorrhages in the tissues. Some people define these to range from 3-10 mm. Others define them to be the multiple surface bleeds that are so common in folks with fragile vessels (including many of the normal elderly -- look especially on the forearms as they often most long-term sun-damage and their being below heart level makes for a little more venous pressure).
ECCHYMOSES: A still bigger hemorrhage in the tissues. Some people define these to be above 10 mm.; others define them to be bruises from trauma. An ecchymosis in a normal person is probably a bruise, also called a "contusion"; a person with a bleeding problem is likely to have ecchymoses despite little (or no?) trauma.
{07051} contusions, abuse
|
|
|
|
|
PETECHIAE: Little hemorrhages in the tissues, generally defined to be under 3 mm across. (If you ever need the singular, it's PETECHIA.)
HEMOPTYSIS: Bleeding from the trachea.
HEMATEMESIS: Vomiting blood.
HEMATOCHEZIA: Bright red blood out the rectum. From lower GI bleeding. Say hemato-KEYS-ia.
MELENA: Black, tarry, partially-digested blood out the rectum. From upper GI bleeding. (Pronunciation varies among regions and dictionaries; MELL-eh-nuh, MELL-uh-nuh, muh-LAY-nuh, muh-LEAN-uh).
* SEROSANGUINEOUS is a natural term pathologists use for watery effusions that contain a bit of visible blood.
You will learn about the causes of hemorrhage soon enough. In addition to trauma, there are diseases of blood vessels themselves (from the petechiae of scurvy to the rupture of a syphilitic aortic aneurysm into the throat), diseases around blood vessels (infections, cancers), lack of clotting factors (congenital, acquired, DIC), lack of platelets, and high blood pressure.
The significance of hemorrhage depends on "where" and "how much".
Bleeds into the brain are devastating. A quarter-pint of blood forced into the pericardial sac under left-heart pressures causes instant death by occluding the return of blood to the right side of the heart. A thimbleful of bleed into the vitreous lead to blindness.
By contrast, a periorbital hematoma (the familiar "black eye") merely presents an illustration of bilirubin's colorful breakdown products.
{13104} hemorrhage into the pituitary; another really bad place to have a hemorrhage
{21233} petechiae in the mouth from a mouthguard. Not so troublesome.
10%... You donated a unit of blood. Thank you. 20%... You will probably feel a little sick. 40%... You will probably go into hypovolemic shock. |

Painting, "Blood on the Floor", 1986 |
If you lose even a little bit of blood each day, you have an increased iron drain. Depending on your diet, you may become iron deficient.
Future clinicians: When a person's indirect bilirubin goes up "for no apparent reason", consider that he/she may have bled into a third-space location and is now breaking down and recycling the hemoglobin components. Also remember intravascular hemolysis and large thrombi!
{06275} hemorrhage in the lung (blood in alveoli)
{06278} hemorrhage (blood in the stomach)
THROMBOSIS: The transformation of flowing blood from a liquid to a solid within the vessels or heart.
{11456} thrombi in the venous plexus around the prostate
{31952} thrombus in the superior saggital sinus
{11639} thrombus in the femoral vein
![]() Thrombosis of intracerebral vein
Thrombosis of intracerebral vein
Baby
Pittsburgh Pathology Cases
"Blood is very special juice" (Goethe's Faust). Among other properties, blood must be a liquid inside the vessels, and a solid outside the vessels. You can review the clotting cascade and platelet activities in "Big Robbins".
The REAL clotting cascade (i.e., how it works in life most of the time)
We didn't pay any attention to TF until recently, since if you lack it, you don't get born.
Some more terms:
THROMBUS: Blood that has solidified within the vascular lumens or cardiac chambers.
CLOT: Blood that has solidified anywhere else. (Sloppy usage allows you to call thrombi "clots", at least when talking to non-physicians.)
Three conditions predispose to thrombus formation: (1) INJURED ENDOTHELIUM; (2) ALTERATIONS IN NORMAL BLOOD FLOW; (3) HYPERCOAGULABLE BLOOD. These are VIRCHOW'S TRIAD (historians see South. Med. J. 97: 213, 2004), and worth remembering (even for real life).
The only item that seems arcane is altered blood flow. There are a number of reasons for this.
You remember from physiology that blood physics keeps the formed elements, including the platelets, away from the endothelial surface. When the flow is turbulent, the platelets meet the endothelium.
Activated coagulation factors, which are ordinarily cleared by the onward flow of blood, probably accumulate in pockets of turbulence, while sufficiently anti-clotting proteins probably cannot reach these pockets.
Varying shear itself seems to activate platelets (Nat. Med. 15: 665, 2009).
Finally, turbulence itself might physically damage endothelium.
THE CAUSES OF THROMBOSIS:
INJURED ENDOTHELIUM
Myocardial infarcts
Myocarditis sites
Cardiac jet lesions (abnormal flow)
Inflamed or prosthetic cardiac valves
Ruptured atherosclerotic plaques
Vasculitis syndromes
Radiation injury
High blood pressure itself (?)
After an electrical injury (don't forget this one: Lancet 363: 2136, 2004)
Invasion of vessel by tumor
(think of renal cell, hepatocellular, adrenocortical, or follicular thyroid carcinomas)
Iatrogenic
Sclerotherapy for varicose veins
Indwelling lines, etc.
ALTERED BLOODFLOW ("TURBULENCE AND STASIS")
Myocardial infarcts (dead wall balloons out)
Quivering ("fibrillating") cardiac atria
Over big ruptured atherosclerotic plaques
In dilated cardiac chambers (valve or muscle disease)
In weakened arteries that have ballooned ("aneurysms")
Over-viscous blood (much more prone to stasis)
Polycythemia (too much red cell mass)
Cryoglobulins (proteins that tend to precipitate)
Macroglobulinemia (too much IgM)
Vascular malformations
Prolonged bed-rest or immobilization
HYPERCOAGULABLE BLOOD
Congenital factor deficiencies
Lack of antithrombin III
Lack of protein S
Lack of protein C (even heterozygotes: Lancet 341: 134, 1993)
Factor V-Leiden (poor response to C)
High blood homocysteine (Lancet 345: 882, 1995 and MUCH more...)
Pregnancy and after childbirth
Tissue damage
After severe trauma or burns
After surgery
Nephrotic syndrome
(glomerular leakage of protein; probably because small anti-coagulant proteins such as protein S are selectively lost)
Secretion of thrombogenic factors by tumors
(notably adenocarcinomas, notably of the pancreas)
Presence of "lupus anticoagulant" (paradoxical)
Skeptics: "Hypercoagulable blood" is commonly invoked, but poorly understood. Smokers, the elderly, the obese, and non-Oriental people all seem to get more thrombi than others.
{06299} thrombus on a venous catheter
What do thrombi look like?
Ante-mortem thrombi generally have formed in irregular, swirling layers with more or fewer red cells and/or platelets included. (When flow is laminar, fewer red cells are incorporated; when flow is turbulent, more red cells are incorporated.) These are the famous LINES OF ZAHN.
There are still many mysteries to thrombus formation, and only now are we getting some light on how platelets attach to the building mass in diffrent ways depending on whether the blood flow is fast or slow (Nat. Med. 15: 607 & 665, 2009).
Ante-mortem thrombi tend to be rather hard and crumbly ("friable"; especially after the factor XIII has crosslinked their molecules).
|
{11039} lines of Zahn
|
|
|
By contrast, thrombi that form after death do not have lines of Zahn. (Why not?)
At most, when
thrombosis occurs after red cells sediment to the dependent portions of the vessels, you will see separate
"chicken fat" (erythrocyte-poor thrombus;
first distinguished from pus by Virchow) and "currant jelly" (erythrocyte-rich thrombus). They are
rubbery, gelatinous, and non-adhesive.
|
|
Special thrombi:
MURAL THROMBI form on the walls ("mur-") of the cardiac chambers and aorta. As a rule, they do not occlude the lumen (since the patient would have died first.)
{06317} atrial mural thrombus
{11600} old cardiac mural thrombus
![]() Mural thrombus
Mural thrombus
After heart attack
Utah Webpath
ARTERIAL THROMBI usually occur over ruptured atherosclerotic plaques, less often at sites of other vascular disease or old surgery.
Except in the aorta, arterial thrombi often occlude the artery, adhering tightly to the wall, and seldom embolize.
{19454} thrombus on ruptured plaque in coronary artery. Fresh thrombus at bottom.
Starting to scar up at top.
{24781} thrombus in the carotid artery
Thrombi that form in the aorta, however, are notorious for embolizing.
You may hear the confusing term WHITE THROMBUS for one that forms in the arterial system. Where blood is flowing relatively fast and smoothly, the red cells are kept away from the walls (remember?), so fewer red cells are incorporated into the fibrin meshwork. Don't rely on this.
VEGETATIONS are thrombi that occur on cardiac valves. They may be loaded with bacteria ("bacterial endocarditis"), or sterile ("marantic", "verrucous", "bland"; also the thrombi of acute rheumatic fever).
{06287} thrombus on a heart valve
VENOUS THROMBI ("phlebothrombosis", the term "thrombophlebitis" is often misapplied) almost always occlude the vein. If there are valves in the vein (i.e., it's a leg vein), the valve impressions will be visible on the surface of the thrombus, even if it embolizes.
Even without embolization, venous thrombi are likely to be symptomatic.
Deep leg vein thrombi are usually asymptomatic, but often cause pain and edema ("inflammation" -- it isn't). On rotations, you'll learn "Homan's sign" -- squeezing the calf or dorsiflexing the foot to elicit tenderness in these patients. (Beware: These maneuvers can dislodge the thrombus.) You'll also learn about scans, Doppler ultrasonography, heparin therapy, etc.
Even thrombosis of superficial (varicose) veins can be painful.
MILK LEG ("phlegmasia alba dolens") is an old name for venous thrombosis in later pregnancy or after delivery.
TROUSSEAU'S SIGN (or "Trousseau's other sign") is widespread (or "migratory") venous thrombosis, in patients with cancer of the pancreas.
* More recently, it's been shown that mucins bind to selectins, and that mice without selectin are immune to thrombi from cancer mucin (J. Clin. Inv. 112: 853, 2003). This doesn't explain why Trousseau's usually means pancreatic rather than colon cancer, though colon cancers tend to be much richer in mucin.
PYEMIA is a word occasionally used for an infected venous thrombus that has embolized. The classic example is a septic venous thrombus near an inflamed appendix that has embolized to the portal vein.
Rule: When thrombi form in fast-moving blood (heart, arteries), fibrin and platelets will predominate. (Why?) When thrombi form in slow-moving blood (veins, sites of turbulence and stasis), they will contain areas that are rich in red blood cells.
What happens to thrombi?
Thrombi in contact with flowing blood tend to PROPAGATE, as more clot forms on their surface. Propagation is in the direction of blood flow, and may ultimately obstruct the blood flow.
Propagation of a thromboembolus into the distal arteries confirms that the patient survived at least for a time.
The clot physiologists identify "coralline thrombi", little coral-shaped masses of platelets formed within the turbulent bloodstream, as the framework on which fibrinous clot continues to form.
Thrombi may fragment or break free, producing THROMBOEMBOLI. More about this later.
Since thrombi are composed of fibrin, they are simultaneously attacked by plasmin (to break them up) and invaded by fibroblasts and angioblasts (to make them into scar, i.e., they ORGANIZE).
{06293} organizing thrombus, leg vein
{06305} organizing thromboembolus, lung
|
|
Australian Pathology Museum High-tech gross photos
|
When the thrombus is large, we think the plasmin almost always loses the race. As the thrombus turns, over a few weeks, into vascular granulation tissue, it RECANALIZES.
Ultimately, an occluded vessel that once had a single large lumen ends up with many tiny lumens, or a lumen crossed by a fibrous band. (A good place to catch the next thrombus....)
{06533} recanalized thrombus
|
|
Mural thrombi generally take a long time to organize, and they even calcify.
Occasionally, very large thrombi become infected with bacteria, producing an intractable infection that ultimately turns the thrombus into pus.
DISSEMINATED INTRAVASCULAR COAGULATION (the dreaded "DIC", "consumption coagulopathy", or "defibrination syndrome")
A host of disorders cause clotting of blood in the microcirculation. This may be an acute or chronic problem.
CAUSES OF DIC WORTH REMEMBERING NOW:
Things that release thromboplastin into the blood
Large infarcts
Massive intravascular hemolysis (remember bad malaria![]() )
)
Acute promyelocytic leukemia
Various obstetrical catastrophes
Disseminated cancers
Snakebite
Decompression sickness (happens on bubble surfaces)
Traumatic brain injury (J. Neurosurg. 97: 1373, 2008 -- makes an already-bad situation worse)
Ebola![]() and Marburg virus infections (macrophages express tissue factor on their surfaces: Lancet Inf. Dis. 4: 487, 2004.)
and Marburg virus infections (macrophages express tissue factor on their surfaces: Lancet Inf. Dis. 4: 487, 2004.)
Things that damage endothelium
Rickettsial diseases
Meningococcemia
Other infections (remember Ebola, Marburg, and other hemorrhagic fevers; malaria Am. J. Trop. Med. 76: 648, 2007)
Vasculitis syndromes
Toxemia of pregnancy (fibrin thrombi in placenta)
Things that do both
Shock
Gram-negative sepsis (this is a BIG deal right now, with administration of activated protein C for sepsis having become mainstream: NEJM 361: 2646, 2009.
The necrotizing fasciitis family of infections ("really bad staph"; "really bad strep") cause the necrosis by their ability to invade vessels. These bugs have elaborate arrays of toxins. More about them from your microbiology instructors.
Major surgery
Burns
Massive trauma
Heat stroke
Ebola & Marburg as above, and goodness knows what other emerging infectious diseases
Regardless of the cause of DIC, factors I, II, V, VIII, and X, as well as platelets, become depleted. Fibrinolysis becomes activated, and formed clots break down.
Fibrin split products in the blood result from breakdown of thrombi of any size by plasmin. Increased amounts of these substances in the blood is a hallmark of DIC. Pitfall: They are often present whenever there are significant thrombi within the body. Later, you'll learn about other tests for DIC, inclding d-dimer and 21st-century techniques such as thromboelastography (which is much more helping in telling where there's a real clinical problem than the old-fashioned "fibrin split products" assay: Am. J. Clin. Path. 134: 97, 2010).
In DIC, look for fragmented red cells ("schistocytes") that were broken by contact with fibrin strands ("like tomatoes pushed through chicken wire" works). Anemia may result.
{12308} schistocytes
Even if the microthrombi do not cause organ failure / gangrene, the patient becomes depleted of clotting factors.
When the clotting factors and platelets are consumed, the patient will begin bleeding from previous needle-stick sites ("clinical oozing", as plasmin tears up the clots that hold these wound together), and then from every orifice.
This is truly a clinician's nightmare -- the physician must consider anticoagulating, and withholding clotting factors from, a bleeding patient. (Heparin may save the patient's life, while administration of more clotting factors will lead to more microthrombi.) Get help.
"The best treatment for DIC is treatment of the underlying cause."
At autopsy, we see little fibrin-platelet thrombi in small vessels (look especially in the renal glomeruli -- DIC is bad for the kidneys).
{21028} DIC: little thrombus in a glomerulus
|
|
THROMBOEMBOLI
|
|
EMBOLUS: Any solid, liquid, or gaseous thing other than liquid blood and its solutes that travels along the bloodstream. It will impact and lodge somewhere.
EMBOLISM is the clinical syndrome / situation of having one or more emboli. "Embolus" is to "embolism" as "alcohol" is to "alcoholism". Please don't point to the thromboembolus and call it "an embolism".
![]() "Embolus" comes from the Greek for "bottle stopper".
"Embolus" comes from the Greek for "bottle stopper".
* "Emboli...
You're driving me crazy...
You're making my mentation hazy...
You're going to my head....
Despite the above, embolization is no laughing matter when it causes infarction of a major organ such as the brain ("embolic stroke"), or when a pulmonary embolus causes unexpected death.
Most emboli are dislodged or fragmented thrombi ("THROMBOEMBOLI").
Used without qualification, EMBOLUS means THROMBOEMBOLUS.
{10682} embolus, celiac trunk
You will learn more about PULMONARY THROMBOEMBOLI in the respiratory disease section. Worth knowing now:
The large majority of pulmonary emboli come from the deep leg veins.
Pulmonary embolization is one of the great killers of hospitalized patients, and that ante-mortem diagnosis is notoriously unsatisfactory even today.
Year I's: Please remember that systemic venous thrombi end up the pulmonary arteries, the only arteries in the body that carry unoxygenated blood. Don't mistakenly call them "veins".
Patients die of saddle embolization (occlusion of both main pulmonary arteries, lethal), acute right heart failure (this may result from occlusion of as little as 60% of a normal person's pulmonary arterial bed), rhythm disturbances in the strained right ventricle, bronchoconstriction produced as the clot's platelets release serotonin, or vagal reflexes triggered by the bad thing arriving in the pulmonary arteries.
Or patients may have several episodes of embolization, leading to permanent high pulmonary vascular resistance and thence a very poor quality of life.
{03182} saddle embolus
{10799} saddle embolus
{10802} saddle embolus
{11133} saddle embolus
{06311} pulmonary emboli
{20221} small pulmonary embolus
{20992} pulmonary embolus
These emboli seldom produce infarction (especially if they do not occlude the arteries to entire lobes). This is because the lung has a dual blood supply via the bronchial arteries. In systemic hypotension, when the bronchial arteries are poorly perfused, infarction may result. Patients with infarcts develop hemoptysis (blood flowing into dead tissue, through dead vessel walls, and into the airways).
The majority of pulmonary emboli go unrecognized during life.
A PARADOXICAL EMBOLUS (* crossed embolus) is one from the systemic veins that passes through a right-to-left intracardiac shunt (i.e., a birth defect), to occlude a systemic artery.
A common way to develop a right-to-left shunt is to have some previous pulmonary emboli that have caused right atrial pressure to exceed left atrial pressure, so that the foramen ovale (potentially patent in 25% of individuals) opens up. Review of paradoxical emboli: Chest 108: 549, 1995.
Pulmonary emboli seldom lyse fully. Usually, a little fibrous band remains where they have landed.
SYSEMIC EMBOLIZATION is embolization down a systemic artery.
Most emboli that actually occlude a named artery come from the heart. Origins:
60%... mural thrombi from myocardial infarcts
10%... atrial thrombi (valve disease, fibrillation)
5%... cardiomyopathies
25%... others: aortic aneurysms, left-sided endocarditis, prosthetics, paradoxical emboli, ulcerated atherosclerotic plaques, "origin unknown"
___
100%
Rule: In contrast to pulmonary emboli, systemic emboli almost always produce infarcts. No artery is immune, though the majority probably go to the lower extremities.
Note that the emboli of bacterial endocarditis are laden with micro-organisms, and that abscess formation is likely.
AMNIOTIC FLUID EMBOLI ("amniotic fluid infusion")
This very serious event occurs in 1 out of 50,000 deliveries (hasn't changed recently: Ob. Gyn. 115: 910, 2010). Amniotic fluid, which is full of baby's debris, enters the systemic circulation. Respiratory difficulty and shock are followed by DIC.
The pathologist finds squamous cells and other debris in the pulmonary vasculature. The molecular biology of the clinical syndrome is poorly understood. Many victims die even today.
{11663} amniotic fluid embolus
AIR EMBOLI ("gas emboli", etc.): Gas in the circulation. Bubbles coalesce and produce a mass of air that the pulse pressure just compresses, preventing the blood from being pushed. Recalls "vapor lock" in automobiles.
CAUSES OF GASEOUS EMBOLI
Ruptured uterine veins
Delivery
Abortion
Certain unwise sexual practices (Ob. Gyn. 61: 653, 1983; Am. J. Med. 78: 333, 1985; Crit. Care Med. 15: 703, 1987; Postgrad. Med. J. 74: 612, 1998; even starting again too soon after childbirth Am. J. For. Med. Path. 31: 247, 2010).
A rock singer inhales helium under too much pressure and blows up his mediastinum with resulting air embolization: Crit. Care Med. 30: 1156, 2002.
Ruptured chest veins
Chest trauma
Iatrogenic (common) or homicidal
Secondary to a slashing involving any large vein (uncommon)
Air entering the dural sinuses during neurosurgery
Transbronchial lung biopsy (Br. J. Rad. 83: e83, 2010; AJR 193: W430, 2009).
Cutting the victim's jugular vein (air embolization will occur when the victim inhales)
Scuba diving
* Future pathologists: Anyone dying during or just after a typical scuba dive will have bubbles in the bloodstream as the nitrogen comes slowly out of solution, and their presence proves nothing (J. Clin. Path. 59: 489, 2006).
IATROGENIC CAUSES range from problems with central venous pressure lines (famous; South. Med. J. 80: 96, 1987, many others) to a host of surgical procedures, notably on the head and neck (Arch. Path. Lab. Med. 113: 498, 1989) or during C-section. Forceful artificial ventilation is an important cause: Chest 93: 874, 1988; Ann. Int. Med. 110: 694, 1989. So is angioplasty (Am. Heart J. 119: 1374, 1990, from St. Luke's, K.C.) Gas embolization from "minimally-invasive vein harvesting", in which tissues surrounding a leg vein are blown up with carbon dioxide: Ann. Thoracic Surg. 73: 296, 2002. A "complementary alternative medical" practice involves giving hydrogen peroxide by vein; it is bad for you (Neurology 49: 1477, 1997; also Am. J. For. Med. Path. 21: 144, 2000). Ozone quack: Am. J. For. Med. Path. 21: 144, 2000. Freak dental surgery mishap: Anesth. Analg. 106: 249, 2008. A phlebotomist I know tells me he saw a patient die of air embolization after he disconnected his IV line from the bag to make his bathroom visit more convenient. Another guy decided to connect his central venous line to his oxygen tube for some reason; it was the last thing he ever did (Am. J. For. Med. Path. 20: 256, 1999).
Of course, you'll see bubbles from time to time in the intravenous lines. They are probably harmless. Serious injury will happen only when there's enough air in the heart all at once to make compression ineffective.
DECOMPRESSION SICKNESS results when a pressurized underwater "caisson" worker or scuba diver surfaces too fast, or when a high-flying plane's cabin depressurizes. The nitrogen (mostly) in the tissues comes out of solution and enters the tissue and circulation into the circulation as bubbles. It's rapid in our watery tissues, slower in our lipid-rich tissues. The acute form ("the bends", "the chokes") causes agonizing pain and brain damage -- the latter because nitrogen is very soluble in myelin. The chronic form ("caisson disease") causes ischemic necrosis of parts of the skeleton -- the mechanism is poorly understood.
Wherever the gas lodges, it interferes with blood flow. Large amounts of gas in the heart render pumping ineffective -- it merely compresses the gas.
The few bubbles introduced into the blood during intravenous therapy seem to be harmless. It takes maybe 100 mL of gas to harm a grown-up.
In suspected air embolism, the pathologist opens the heart, pulmonary artery, and thoracic aorta under water. The gas will emerge as several large bubbles or as froth.
Clinicians listen for the "water wheel murmur", etc., etc., to diagnose air embolism.
If you think your patient has an acute air embolus, standard advice is to roll him onto his left side, so that the gas will pool safely in his right atrium.
|
|
|
|
FAT EMBOLI
After fractures of bones, globules of fat are released into the circulation. Usually this is trivial, but sometimes people get sick.
* As you know, the fat from inside bones is also called "yellow marrow" when it lacks abundant hematopoietic elements. Of course this is on a continuum with "bone marrow emboli" which we define to be rich in hematopoietic elements. My impression is that bone marrow emboli are likely to stay in the lungs because many of the red-marrow cells naturally adhere to endothelium, while fat globules are likely to travel through to the brain because fat cells lack these adhesion molecules and/or were disrupted. So far as I know, and understandably, no one's studied this.
The FAT EMBOLIZATION SYNDROME occurs 1-3 days after injury with heavy fat embolization.
It is clear that fat can pass through normal lung and proceed to the brain (Anesth. Analg. 97: 1789, 2003.)
The molecular biology is still poorly understood. Some authors cite pure physical chemistry, others cite putative products released from the fat, while still others cite DIC and claim the microthrombi disappear between death and autopsy.
In "the mouse model", the fat somehow liberates nitric oxide in the lung, damaging it (J. Trauma 64: 462, 2008); the authors suspect several other molecules are involved as well, and acknowledge that even today, the clinical syndrome remains a mystery.
Regardless of what is really happening, patients die of pulmonary edema and generalized lung damage. Look for petechiae throughout the skin, eyes, and CNS white matter.
Future pathologists: Use frozen sections and fat stains to find globules of fat in the lungs, brain, and kidneys.
{29056} fat embolus in lung, oil red O stain
{29057} fat embolus in lung, oil red O stain
Fat embolization from other causes is fortunately rare. Remember severe pancreatitis and getting nasogastric feeding formula into the IV line by mistake.
OTHER EMBOLI
ATHEROEMBOLI (Lancet 338: 1365, 1991) are bits of grumous debris from inside atherosclerotic plaques. These embolize, notably to the kidneys, toes, and male genitals.
{10889} atherosclerotic embolus
{25651} atheroembolus
{25652} atheroembolus
BONE MARROW EMBOLI are a routine autopsy finding following vigorous cardiopulmonary resuscitation, which fractures ribs.
|
|
TUMOR EMBOLI are bits of cancer that invaded a vein and then broke off. Renal cell carcinoma is famous for this.
THERAPEUTIC EMBOLIZATION of bad body parts by clinicians may use gelatin foam ("Gel-foam"), silicones (especially a current illegal practice for cut-rate breast augmentation: Chest 127: 2276, 2005), or other substances.
And most anything else can embolize. Trophoblast in eclampsia is probably under-recognized (Am. J. For. Med. Path. 21: 354, 2000. Brain in a child with severe head injury (Am. J. For. Med. Path. 34: 9, 2013). Catheters: J. Emerg. Med.6: 1, 17, 1988; NEJM 352: e3, 2005. Bullets: Review For. Sci. Int. 139: 27, 2004; Heart 90: 1298, 2004; Am. J. Surg. 179: 189, 2000. Shotgun pellets: J. Trauma 67: E202, 2009. Needles: Ann. Thor. Surg. 77: 1102, 2004. Acupuncture needle (self-treating): J. Card. Surg. 25: 654, 2010). Bee-bees J. Trauma 49: 774, 2000. Silicone from a black-market butt-job (NEJM 354: 211, 2006). Quack corn oil ("French polymer") injection: Am. J. For. Med. Path. 30: 398, 2009. Vena cava filters: Radiology 174: 445, 1990. Review of foreign bodies in the heart: N.Y. State J. Med. 90: 347, 1990. Emboli in junkies' lungs (pill fillers, talcum powder, and much more): Hum. Path. 113: 113, 1980; Br. J. Addict. 84: 103, 1989. In the 1960's, I knew an enterprising hippie who injected peanut butter "to see what would happen" -- nothing did.
|
|
![]() Cancer embolus to pulmonary artery
Cancer embolus to pulmonary artery
AFIP
Wikimedia Commons
CRYOGLOBULINS, worth mentioning now, are marginally soluble plasma proteins that precipitate in the cold and/or when the plasma is concentrated (i.e., in the glomeruli, do you know why?) They are generally IgM antibodies, often directed against hepatitis B or C (NEJM 330: 751, 1994) or IgG ("rheumatoid factor"). They are more likely to cause ischemia or inflammation (complement-fixers) than infarction. The test for cryoglobulins, which involves putting a sample in the refrigerator, gets overlooked too often.
INFARCTION
An INFARCT is a localized area of necrosis due to ischemia. ("Death is a total body infarct", etc.; again "infarction" is the clinical syndrome rather than the lesion)
Note that all vascular occlusion need not produce an infarct, especially in organs with good collateral circulation (brain, lung, liver, bowels, extremities, the athlete's heart).
By contrast, occlusion in an organ without collateral arteries (spleen, kidney), expect an infarct whenever an arteriole shuts down. To produce an infarct in an older couch potato's heart, all that is required is occlusion of a medium-sized coronary artery.
|
|
If the blood supply is partially compromised, the organ is more likely to atrophy or have death of only some cells (renal cortical tubules, brain's neurons).
Conversely, infarction can occur in the absence of vascular occlusion, when there is narrowing of an artery (i.e., usually from atherosclerosis) and/or arteriole (i.e., from hypertension, from diabetes, etc.) and systemic circulation then drops for some reason.
REPERFUSION INJURY is tissue damage that occurs when already-damaged tissue gets its circulation back.
Problems include (1) calcium, which will enter damaged cells, stiffen sarcomeres, and precipitate with phosphates; (2) oxygen, which will generate free radicals; (3) free radicals (still some talk about this); (4) fresh blood components meeting damaged biomolecules resulting in neutrophil entry, complement activation, and so forth (update Microsurgery 24: 468, 2004).
ARTERIAL INFARCTS usually result from thromboemboli or in-situ thrombus formation. The next most common cause is spasm (Prinzmetal's angina, migraine leading to stroke, ergotism or Raynaud's phenomenon leading to loss of digits).
Much less common are extrinsic compression from adhesions or tumors.
{24501} infarct of hand following embolus to brachial artery
You'll seldom hear this, but menstruation is due, in part, to infraction of the endometrium.
VENOUS INFARCTS result when veins are compressed and deoxygenated blood cannot leave the organ. The classic examples involve the bowel (strangulated hernias, torsion of the testis, fibrous adhesions), compartment syndromes (i.e., edema deep within a limb interferes with venous drainage of closed anatomic compartment, resulting in muscle necrosis), and even tumors or extrinsic pressure (pressure neuropathies) can impinge on outflow. The mechanism of death in many suicidal hangings is venous ischemia of the brain (nasty).
WHITE INFARCTS ("anemic infarcts", from "an-", not, and "-eme", blood) are usual when arteries are occluded in solid organs. If there are collaterals, blood may seep in, but typically bleeding is minimal, cloudy swelling of cells pushes blood back out, and the red cells lyse and disperse their hemoglobin.
RED INFARCTS ("hemorrhagic infarcts", sounds like an oxymoron but isn't) result when veins are occluded, or when arteries are occluded in loose tissues (bowel) or with a dual blood supply, or when the organ was already very congested. Infarcts of the lung and small bowel from any cause tend to be hemorrhagic, and many brain infarcts (especially the embolic ones, where collateral circulation is good) are hemorrhagic from reperfusion.
|
|
Australian Pathology Museum High-tech gross photos
|
{17390} hemorrhagic lung infarct
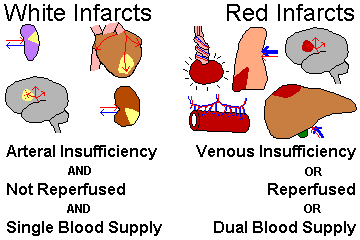
SEPTIC INFARCTS result when bacteria find the dead area. This is likely to happen if they were already present (i.e., the patient had an infection at the site of the infarct, or was "septic" with infected blood), or if the infarct was due to an infected embolus (from a heart valve infection or elsewhere). BLAND INFARCTS do not become infected.
Morphology of infarcts is stereotyped.
"Big Robbins" (and many other authorities) have claimed that "all infarcts tend to be wedge-shaped" (actually, pyramidal), with the apex pointed at the focus of arterial occlusion.
This doesn't really apply for venous infarcts, watershed infarcts, cerebral infarcts, or myocardial infarcts.
The "wedge-shaped infarcts" rule works for lung, spleen, and kidney infarcts.
"Zahn infarcts" of the liver, variably-shaped areas of atrophy (not necrosis) in the distribution of an occluded branch of the portal vein, are another famous autopsy finding. They may appear red, since the hepatocytes atrophy and blood from the hepatic arteries and veins tends to engorge the widened sinusoids.
{17384} schematic infarct
{17385} schematic infarct
{17388} Zahn infarct of liver
{46489} real necrotic infarcts of the liver
Over the following days, the infarct becomes pale or hemorrhagic.
The microscopist sees
coagulation necrosis![]() (unless there is bacterial infection, or the infarct has caused
necrosis of all the cells in a portion of the brain). Inflammatory cells enter the infarct by the first day,
and become plentiful over the next several days.
(unless there is bacterial infection, or the infarct has caused
necrosis of all the cells in a portion of the brain). Inflammatory cells enter the infarct by the first day,
and become plentiful over the next several days.
"Big Robbins" lists several observations about infarcts that are worth reviewing. Although they may seem obvious, they are important to remember in clinical medicine.
(1) The effects of vascular narrowing or occlusion will probably be worse if the blood already lacks oxygen-carrying capacity (i.e., the patient is anemic) or the heart isn't pumping well (heart failure, shock).
(2) Slowly-developing occlusion of an artery (i.e., over months or years) is well-tolerated in organs with collateral circulation, since it allows for development of more and bigger collaterals
(3) Remember that different cells tolerate ischemia for different lengths of time.
Because of their importance, it's worth mentioning DECUBITUS ULCERS here once again. Body weight always prevents blood from flowing evenly over pressure points, but in a person who cannot moved, prolonged ischemia to a single point causes these lesions. Don't get me started on "access to care" and "quality of care" issues here.
Worth mentioning here: CYANOSIS, i.e., bluish discoloration, results when more than 5 gm/dL of hemoglobin is unoxygenated. The reason your hands turn blue in the cold is easy to understand if you think about it. The body decides that relatively less blood will go to cold extremities, to conserve body heat. As a result, the tissues extract almost all the oxygen from what little blood does end up there, and capillary and venous oxygen content drops greatly. Hence the blue color.
SHOCK ("circulatory collapse"): Widespread hypoperfusion of the tissues
CAUSES OF SHOCK
Cardiogenic (cardiac) shock (i.e., abrupt-onset pump failure)
Massive myocardial infarct
Rupture (ventricle, valve)
Diphtheria
Bad rhythm disturbances ("arrhythmias", a misnomer)
Certain poisons (remember massive nicotine ingestion)
Extrinsic compression (i.e., tamponade)
Hypovolemic shock
Heavy bleeding
Externally
Internally (remember GI bleeds, hemoperitoneum)
Other fluid loss
Sweating
Vomiting
Diarrhea
Burns
Third-space losses (i.e., into effusions or ileus)
Loss of vascular tone (i.e., all vessels opening, thus no blood able to return to the heart)
Septic shock (i.e., from bacterial breakdown products and especially cytokine production by way of nitric oxides: NEJM 351: 159, 2004)
Anaphylaxis (generalized mast-cell degranulation)
Neurogenic
Certain poisons (notably war gases)
Profound anaesthesia
Spinal cord injury
Vasovagal (i.e., extreme pain, emotion)
"Total body inflammation" in the very sick -- more about this soon
Dengue shock syndrome (JAMA 299: 324, 2008 -- as I predicted in 2001, dengue has now reached the US thanks to global warming)
Pulmonary emboli (when bad)
Regardless of etiology, hypoperfusion of the whole body produces common problems.
With widespread anaerobiosis, LACTIC ACIDOSIS is likely to develop, and pH goes way down. This is itself unhealthy. (Not surprisingly, it's a better predictor of mortality than blood pressure. See J. Am. Coll. Surg. 210: 861, 2010).
A variety of other SECONDARY MEDIATORS OF SHOCK are produced by hypoperfused tissues to further exacerbate the problem.
Histamine, serotonin, leukotrienes, cachectin, interleukin 1, C3a, C5a, and many other substances dilate vessels, inviting blood to pool in venules (rightly called "congestion"), and/or make small vessels permeable, causing blood to leak out. Some people even blame endorphins.
When endothelial cells are damaged or thromboplastin enters the circulation, DIC may result.
As you can see, shock is a downward spiral.
In COMPENSATED SHOCK, blood is shunted away from the kidneys, salivary glands, gut, skin, and muscles in order to perfuse the brain and heart. Blood pressure is maintained.
Patients may be oliguric from reduced blood flow to the kidneys ("prerenal azotemia"), and have dry mouth and skin from reduced blood flow to these organs.
The "shock index" is the heart rate divided by the systolic blood pressure. If it's above 0.7 (different folks use different units), maybe your patient "who looks okay" is in compensated shock. You've been warned: J. Trauma 67: 1426, 2009.
In PROGRESSIVE SHOCK ("decompensated shock"), blood pressure and cardiac output decline.
All these patients have the lactic acidosis noted above. Now you must treat the patient or death will result.
After a few hours in shock, the kidney tubules die. They'll grow back after a few days if the patient surives, but until they do, patients are oliguric, and accumulate toxic products that are ordinarily excreted in the urine. This is not a lethal problem with today's fluid management. Tough cases can be dialyzed.
In worse cases, the lungs are damaged, and after a few weeks, patients die of pulmonary exudates, fibrin deposition ("hyaline membranes") and perhaps then fibrosis. This state of affairs is called "shock lung" or "adult respiratory distress syndrome".
{06359} shock lung
{06362} shock liver
{06365} shock liver; histology; note central necrosis
As "Big Robbins" put it, "shock not only stops the machine, but wrecks the machinery." IRREVERSIBLE SHOCK has occurred when correction of the deficient cardiac output and volume deficit by any means fail to reverse shock. Blood pressure and pH continue to drop, and the organs die one by one.
If the person is still bleeding for whatever reason when they become hypothermic and acidotic from their shock, survival is very unlikely (Am. J. Clin. Path. 137: 566, 2012).
Common anatomic findings in patients who have spent some hours in profound shock include:
Apart from simple pulmonary edema, lung changes seldom supervene until a few days have passed.
We use the term "watershed" infarcts for those that follow shock, when the portions of organs that are farthest from the main arterial supply (subendocardium of the heart, watershed areas of the brain, splenic flexure and rectosigmoid junction in the large intestine) undergo necrosis.
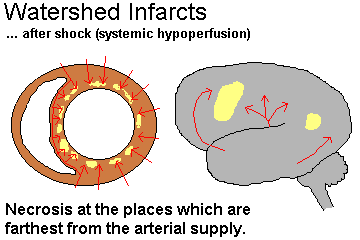
Note that the object of treating shock is to improve the perfusion of the tissues (cardiac output, blood volume), not just to "raise blood pressure". Failure to note this led to deaths in the 1950's from promiscuous use of vasoconstrictors (notably norepinephrine, under the trade name of Levophed, known to pathologists as "Leave-'em-dead"), which raised the measured blood pressure by diminishing tissue perfusion.
We'll talk more about SEPTIC SHOCK later in the course. We think the major problem is that vessels dilate, so that blood pools in the venous circulation rather than returning to the heart. We blame bacterial breakdown products ("lipid A", "peptidoglycans") and molecules produced by the body to fight infection; both injure vessels.
ORTHOSTATIC HYPOTENSION, "orthostasis", i.e., an unusually marked drop in systemic blood pressure upon standing up, has a short differential:
Low circulating volume
Dehydration
Fresh hemorrhage
Autonomic failure
Shy-Drager (multiple systems atrophy, a brain disease)
Neuropathy
Amyloid
Diabetes
Certain drugs
GENERAL REACTIONS TO SHOCK AND TRAUMA
A great deal has been written about "the generalized response to illness", "the syndrome of just being sick", etc., etc. You will have to sort the useful information from the junk (and there's plenty of the latter).
The "stress of illness" tends to produce a few stereotyped responses of questionable clinical significance:
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about the fundamental processes of pathology to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
| New visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
