Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com
No texting or chat messages, please. Ordinary e-mails are welcome.

|

|
 |
 |
 |
 |
|
verify here. |
Cyberfriends: The help you're looking for is probably here.
This website collects no information. If you e-mail me, neither your e-mail address nor any other information will ever be passed on to any third party, unless required by law.
This page was last modified January 1, 2016.
I have no sponsors and do not host paid advertisements. All external links are provided freely to sites that I believe my visitors will find helpful.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected. No texting or chat messages, please. Ordinary e-mails are welcome.
 I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
I am active in HealthTap,
which provides free medical guidance from your cell phone.
There is also a fee site at
www.afraidtoask.com.
 If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |

|
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource.
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
pathology.org -- my cyberfriends, great for current news and browsing for the general public
EnjoyPath -- a great resource for everyone, from beginning medical students to pathologists with years of experience
Medmark Pathology -- massive listing of pathology sites
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm still handling dozens of requests for information weekly, all as a public service.
Pathology's modern founder, Rudolf Virchow M.D., left a legacy of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of all the make-believe and bunk that interfere with peoples' health, reasonable freedom, and happiness. I talk and write straight, and without apology.
Throughout these notes, I am speaking only for myself, and not for any employer, organization, or associate.
Special thanks to my friend and colleague, Charles Wheeler M.D., pathologist and former Kansas City mayor. Thanks also to the real Patch Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:

My home page
More of my notes
My medical students
Especially if you're looking for information on a disease with a name that you know, here are a couple of great places for you to go right now and use Medline, which will allow you to find every relevant current scientific publication. You owe it to yourself to learn to use this invaluable internet resource. Not only will you find some information immediately, but you'll have references to journal articles that you can obtain by interlibrary loan, plus the names of the world's foremost experts and their institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review. If you are interested in complementary medicine, then I would urge you to visit my new Alternative Medicine page. If you are looking for something on complementary medicine, please go first to the American Association of Naturopathic Physicians. And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I do not accept donations, though I appreciate those who have offered to help.
During the eighteen years my site has been online, it's proved to be one of the most popular of all internet sites for undergraduate physician and allied-health education. It is so well-known that I'm not worried about borrowers. I never refuse requests from colleagues for permission to adapt or duplicate it for their own courses... and many do. So, fellow-teachers, help yourselves. Don't sell it for a profit, don't use it for a bad purpose, and at some time in your course, mention me as author and William Carey as my institution. Drop me a note about your successes. And special thanks to everyone who's helped and encouraged me, and especially the people at William Carey for making it still possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
OBJECTIVES
Recognize patients who may have each of the following, and describe the anatomic pathology and what we know of the etiology and pathophysiology of each:
Describe the appropriate lab workups for:
![]() KCUMB Students
KCUMB Students
"Big Robbins" -- Endocrine
Lectures follow Textbook
QUIZBANK
Endocrine (It's impossible to separate pituitary, adrenal, thyroid, parathyroid, etc. Look at it all now.)
|
|
|
|
|
|
|
|
|
|
|
|
|
{11803} normal thyroid, gross
{00135} normal thyroid, histology {11755} normal thyroid, histology {00138} goiter {24613} goiter {39460} goiter |
|
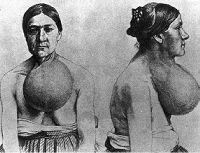 |
Mountaineers dew-lapped like bulls, whose throats had hanging at 'em wallets of flesh... |
 |
INTRODUCTION
This is an easy unit, but you have to do some thinking.
The thyroid begins as a patch on the back of the tongue (at the "foramen cecum"). It descends (down what may become the "thyroglossal duct") into the neck.
The former track may be filled with thyroid tissue, imparting a "pyramidal lobe" to the thyroid (40% or so of thyroids have at least a little one).
Occasionally some or all of the gland ends up in the mediastinum instead, explaining the occasional "retrosternal goiter". Surgeons see Am. J. Surg. 203: 442, 2012.
The thyroid sits close to the four (or however many) parathyroid glands (and sometimes encases and thus hides one or more of them), and to the recurrent laryngeal nerves. These structures may be damaged during surgery.
The healthy adult thyroid weighs around 15-25 gm. If you don't remember its histology and physiology -- follicles full of colloid, iodine traps, microvilli, parafollicular C-cells, thyroxine=T4, iodotyrosine precursor compounds, triiodothyronine=T3, calcitonin (remember it's from the parafollicular cells that are mostly in the upper lobes), synthesis and endocytosis of thyroglobulin, TRH, TSH=hTSH=thyrotropin, etc. -- please review.
HINT: C-cell function is vestigial in humankind, completely dominated by parathyroid function. And don't expect to be able to distinguish the C-cells unless they are hyperplastic (i.e., MEN II, response to chronic hypercalcemia) or immunostained.
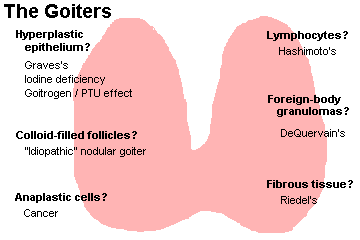
When thyroid is active (i.e., winter, puberty, pregnancy, stress, Graves's disease, Jod-Basedow) or just overstimulated (propylthiouracil or other thioureas that inhibit peroxidase, thiocyanate that inhibits the iodine pump, goitrogens like cabbage), the cells will become taller and thyroglobulin will be reabsorbed. You may even see the overabundant cells piled up as little papillae (really "pseudopapillae", as they lack fibrovascular cores; why?)
{08959} propylthiouracil effect
{24718} propylthiouracil effect
When thyroid epithelium is rendered inactive (i.e., no TSH or other stimulation, or there is excessive iodine that as you remember strongly inhibits lysis of thyroglobulin), the cells flatten down and the amount of colloid increases.
{24719} high-dose iodine effect
Most thyroids removed surgically have "palpation thyroiditis" from all the physical exams, a mix of fibrosis and granulomas typically inside follicles. It's a non-problem.
Any enlarged thyroid (i.e., over maybe 50 gm) is a GOITER (or STRUMA). Areas of thyroid that are mostly colloid (i.e., colloid-rich adenomas, colloid-rich nodules, glands poisoned by excess iodine) will look gelatinous. Areas of thyroid with active cells and colloid-poor follicles look like raw beef. Mitochondria-packed Hürthle cells in a thyroid (i.e., Hashimoto's, some multinodular goiters, some adenomas) impart a brown color (why?)
Lone colloid nodules -- easily diagnosable because their contents are too viscous to be aspirated by an 18-guage needle -- can be huge; they're now ablated by ethanol injection (AJR 191: 1730, 2008).
Nuclear medicine plays an important role in thyroid testing. Active glands (or active nodules in a less-active gland) appear "hot" on scintiscan. Inactive glands (or inactive nodules within a gland) appear "cold".
{09362} normal scan
{09363} cold nodule, right upper pole
Hopefully you remember what thyroid hormones do. Thyroid disease is common and easy to treat effectively, but its onset is insidious and it is often overlooked. "Idiopathic goiter" affects maybe one older adult in 20 and is of negligible significance. Serious thyroid disease mimics "psychiatric disease". This is unfortunate. Hopefully you won't fall into this trap.
Thyroid cancer is the most common endocrine cancer and causes around 1000 deaths per year (current textbooks give figures that are too high). Papillary carcinoma is the most common but the least deadly; most cases are never detected in life. Follicular carcinoma is fairly aggressive. Medullary carcinoma is aggressive. Anaplastic carcinoma is the least common but ultra-aggressive. Many thyroid tumors, both benign and malignant, are incidental autopsy findings (Cancer 64: 1888, 1989).
* The non-disease "black thyroid" is deposition of a pigment (no one knows exactly what) in the thyroids of patients treated long-term with minocycline (Arch. Path. Lab. Med. 118: 79, 1994).
CRETINISM
{49456} cretin, age 4 months
![]() Cretin
Cretin
Classic drawing
Adami & McCrae, 1914
Hypothyroidism, presenting first in infancy or childhood. It may be due to hypothyroidism during pregnancy (permanent brain damage), or to a problem with the child's thyroid gland.
Often there is an inborn error of metabolism (most often a mutation in the thyroid peroxidase gene or a TSH receptor stuck in the "off" position J. Clin. Endo. Metab. 96: E1340, 2011; there are several others known ). Or the thyroid may simply fail to form -- an inquiry into the epidemiology of "thyroid dysgenesis" revealed not a clue as to why this happens.
These people remain like small children both mentally and physically throughout their lives. Replacing thyroid hormone later in life helps, but does not reverse the damage (J. Clin. End. Metab. 70: 336, 1990); for best results, you must treat before the third week (J. Ped. 136: 292, 2000).
The severity of the disease varies. If a mother is severely iodine-deficient, the child will be profoundly retarded, deaf and spastic ("neurologic cretinism"). Less-severely affected children, such as those who cannot make their own thyroid hormone after birth, fail to thrive and remain stunted. They are likely to show any or all of the problems of adult myxedema.
Unless the cause is absence of tissue thyroid hormone receptors, cretinism should never, ever develop. In the U.S., all babies are screened shortly after birth, and impending cretinism is treated. (Even the most fiscally-conservative politicians understand this: Each test costs a few dollars, and treatment is cheap and simple, but lifetime care of a cretin costs megabucks. Ditto for phenylketonuria.)
* The early screening will often miss iodotyrosine dehydrogenase deficiency, which will produce a goiter and hypothyroidism with the danger of neurologic damage if it is missed: NEJM 358: 1856, 2008.
Today's screen always involves measuring Baby's TSH levels, and your lecturer favors the screens that measure both TSH and T4; these will pick up the hypopituitary kids that the TSH-only screen misses. No one is quite sure where to set the limit of normal TSH (J. Clin. Endo. Metab. 95: 4283, 2010; Arch. Dis. Child. 95: 169, 2010). It also infamously misses mutated TSH's that go on to cause congenital hypothyroidism.
EPIDEMIC CRETINISM is the result of endemic dietary deficiencies in iodine.
I would conclude from this that iodine deficiency has been a limiting factor on human populations, and the ability of people to function as they should, throughout much of the world throughout most of history. I would also consider ready-available iodine to be one undeniable blessing of science.
SPORADIC CRETINISM is the result of some kink in development or metabolism.
Causes of sporadic cretinism:
You need to treat these kids aggressively with thyroid supplements; undertreating cretinism is disastrous: J. Ped. 125: 147, 1994.
ACQUIRED HYPOTHYROIDISM (Lancet 363: 793, 2004 -- it's often missed even though this should never happen)
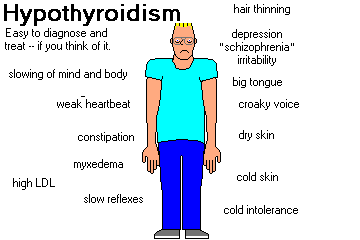
CATEGORIES
PRIMARY HYPOTHYROIDISM means the thyroid gland is under-functioning because of some problem other than insufficient hTSH.
SECONDARY HYPOTHYROIDISM ("central hypothyroidism") means the gland is hypo-functioning because it is being under-stimulated by too little hTSH, reflecting a primary problem in the pituitary gland. Please don't miss this.
TERTIARY HYPOTHYROIDISM (the other "central hypothyroidism") means there is too little hTSH because there is too little TRH, i.e., a primary problem in the hypothalamus. Uncommon but not ultra-rare (Pitutiary 11: 181, 2008); it will come up for discussion when the patient actually has "euthyroid sick syndrome".
SIGNS AND SYMPTOMS OF HYPOTHYROIDISM
SLOWING OF MIND AND BODY is the prime problem. Mental slowness, fatigue, irritability, and loss of interest may be mistaken for, and treated as, "depression" (they should revoke somebody's license, but it happens every day), or there may be hallucinations and delusions ("myxedema madness" -- people have been hospitalized long-term on psych wards for this). This progresses to profound disability, MYXEDEMA COMA and death.
NOTE: Down's syndrome (trisomy 21) folks often (at least 50% of the time) get at least a chronic lymphocytic thyroiditis, and they may end up hypothyroid. Don't overlook this, or assume the mental slowness is just part of Down's. In fact, there is now a trend to supplement Down's children with thyroxine while they are young; this seems to help growth and development (J. Clin. Endo. Metab. 90: 3304, 2005).
MYXEDEMA properly refers to accumulation of hydrophilic ground substance throughout the connective tissues of the body; this leads to coarsening of the facial features, enlargement of the tongue, puffiness around the eyes, and deepening and croaking of the voice.
* Future pathologists: Mucoprotein in the ducts of sweat glands is a tipoff to myxedema.
{24611} myxedema
{25468} myxedema
{25469} myxedema
LDL CHOLESTEROL increases strikingly, and this promotes atherosclerosis.
CARDIAC DYSFUNCTION ("hypothyroid cardiomyopathy") leads to low heart rate and loss of cardiac strength. The end-stage myxedema patient's heart is a typical dilated cardiomyopathy. The accelerated atherosclerosis doesn't help, either. This is another reason to treat hypothyroidism gingerly.
CONSTIPATION is common.
WEIGHT GAIN is usual, and beware of sleep apnea.
DRY SKIN and COARSE, BRITTLE HAIR that may fall out in patches or all over.
YELLOWISH DISCOLORATION OF THE SKIN (for some reason, these people tend to get more carotene in the bloodstream -- actually true Int. J. Vit. Nutr. 69: 132, 1999)
COLD INTOLERANCE (poor perfusion of the extremities, sluggish mitochondria)
DELAYED DEEP TENDON REFLEXES ("hung reflexes") is a helpful physical sign.
CAUSES OF HYPOTHYROIDISM LATER IN LIFE
BIRTH DEFECTS
|
|
THYROGLOSSAL DUCT CYSTS are bits of the old thyroglossal duct. The cysts may be lined by thyroid and/or squamous epithelium (why?), always with some lymphoid tissue (why?) and without C-cells (why?) Protruding the tongue as far forward as possible will cause the cyst to rise. Savvy surgeons treat these midline cysts by removing them along with the center of the hyoid bone to prevent recurrence (why?)
{49471} thyroglossal duct cyst, patient
{09245} thyroglossal duct cyst, histology
Bits and pieces (or all of) the thymus and/or parathyroids may lie within the thyroid capsule. Bits of extra thyroid may be found elsewhere, notably on the tongue (the annoying "lingual thyroid").
{21529} lingual thyroid
In some folks, the thyroid gland just never develops. Unless the hormone is replaced, these people will become cretins. Gene J. Clin. Endo. Metab. 86: 234, 2001.
HASHIMOTO'S THYROIDITIS ("chronic autoimmune thyroiditis": NEJM 335: 99, 1996)
{09241} Hashimoto's, gross
{08960} Hashimoto's, histology
{08961} Hashimoto's, histology
{09242} Hashimoto's, histology
{37881} Dr. Hashimoto
{37882} Dr. Hashimoto "after 40 years of teaching"
|
|
|
|
|
A common, chronic, progressive thyroid disease. There are maybe 1,000,000 Hashimoto cases in the U.S. Most patients are adults, and as with most autoimmune disease there is a female preponderance, but no age or sex is immune. The autoantigen is thyroglobulin and/or peroxidase in the microsomes.
Patients are likely to have a goiter. Most are euthyroid, many are hypothyroid, and a few are at least temporarily hyperthyroid ("Hashitoxicosis", "Toximoto's disease").
If you biopsy it (and you usually don't), patients with Hashimoto's disease will exhibit (1) lots and lots of lymphocytes in the thyroid gland; (2) germinal centers; (3) plasma cells; (4) Hürthle cells (i.e., cells packed with mitochondria, also called "oncocytes"; they probably don't make thyroid hormone).
The unusual "fibrosing variant" features more fibrosis, more scar contraction, and less of everything else. Unlike Riedel's, it stays within the gland.
* Some physicians distinguish a non-Hashimoto "primary thyroid atrophy" with a very small thyroid gland with most of the cells lost ("Ord's disease") but this is probably just a Hashimoto's variant, as both feature the same autoantibodies, and the size range isn't bimodal (J. Clin. Endo. Metab. 94: 833, 2009.)
We've already seen this disease as the prototype of antibody-dependent cell-mediated cytotoxicity. More in keeping with some of the newer work on Sjogren's, type I diabetes, etc., etc., we now know that Hashimoto thyroids express HLA-DR antigens on their follicular cells, and this might get the process going.
These people have increased rates of autoimmune addisonism, pernicious anemia, Sjogren's, vitiligo, and type I diabetes. We'll talk about the autoimmune polyendocrine syndromes when we discuss the adrenals.
PITFALL: You remember that many Hashimoto patients have SCHMIDT'S SYNDROME -- coexisting autoimmune adrenalitis with addisonism. Further, if there's a problem with the pituitary or hypothalamus causing the hypothyroidism, there's likely to be concurrent secondary adrenal insufficiency. So... before you give that patient in myxedema coma a nice booster of thyroid hormone, first administer glucocorticoid so as not to cause death from acute adrenal insufficiency!
We will review Hashimoto's encephalopathy, a vasculitis involving the subcortical white matter, under "CNS". Thankfully only about 1% of Hashimoto's patients get this. Don't forget about it, or assume the patient has "MS" or "Alzeimer's" or "idiopathic epilepsy". Autopsy findings Neurology 61: 1124, 2003.
NON-HASHIMOTO LYMPHOCYTIC THYROIDITIS
Abundant lymphocytes in the thyroid gland, but without germinal centers, plasma cells, or Hürthle cells (Cancer 68: 1944, 1991). This is extremely common, especially in older women.
In the very common "chronic lymphocytic thyroiditis", there may be a small goiter, and there may be transient hyperthyroidism. Nobody really knows the cause or the relationship to DeQuervain's, Hashimoto's, etc.
Postpartum thyroiditis, one variant of "subacute lymphocytic thyroiditis", has been studied well and has increased expression of HLA-DR antigens on the surfaces of the follicular cells (no surprise; Am. J. Clin. Path. 100: 200, 1993). It's extremely common (the Italians say 1 in 25 women -- and in this series, half of these women were hypothyroid a year later J. Clin. Endo. Metab. 96: 652, 2011.
This pathologist suspects the histopathology covers several diagnostic entities, including the ill-defined PRIMARY AUTOIMMUNE MYXEDEMA, often seen in Down's.
To date, there is no international classification of thyoriditis, and nowadays you'll probably just hear both Hashimoto's and non-Hashimoto's called "chronic autoimmune thyroiditis" (NEJM 335: 99, 1996).
Be this as it may, lots of kids have goiters because of lymphocytic infiltration, some will be euthyroid, some will be hypothyroid, and you'll make these goiters shrink with thyroid hormone therapy (J. Clin. Endo. Metab. 91: 1729, 2006; J. Clin. Endo. Metab. 92: 1647, 2007).
DEQUERVAIN'S SUBACUTE GRANULOMATOUS THYROIDITIS ("thyroid virus infection")
{09247} DeQuervain's
{24721} DeQuervain's
Thyroiditis review for the primary care physician: Am. Fam. Phys. 61: 1047, 2000; Am. Fam. Phys. 73: 1769, 2006.
Despite "Big Robbins", infections involving the thyroid gland are extremely uncommon, with the outstanding exception of DeQuervain's, a common, usually-missed, usually-mild disease.
In "DeQuervain's", the thyroid follicle cells die off in patches, almost certainly the result of some
virus or other. Known culprits include
mumps![]() ,
coxsackie B
,
coxsackie B![]() (most common),
EBV
(most common),
EBV![]() ,
ECHO, and
adenovirus
,
ECHO, and
adenovirus![]() . There are surely others. Epidemic DeQuervain's: J. Clin. End. Metab. 70: 396, 1990.
. There are surely others. Epidemic DeQuervain's: J. Clin. End. Metab. 70: 396, 1990.
As you'd expect, the gland becomes large and painful. If you are overzealous enough to biopsy the gland, you will see a spectacular granulomatous response to the released colloid (probably not "sequestered antigens"; it looks like a typical foreign-body reaction to glop).
Most patients are young adult women, but nobody is immune. The major problem is generally the pain (neck, or referred to ear; "take two aspirins"), though sometimes the process is painless. Occasionally, enough thyroglobulin may be broken down to produce transient hyperthyroidism, or enough of the gland may be destroyed to produce hypothyroidism. The sed rate goes way up (why?)
In weeks to months, things settle down and the disease goes away by itself. Despite the impressive histology during the illness itself, I've never seen what I thought was "old scarring from DeQuervain's" at autopsy.
* DeQuervain's producing "acute mental illness": South. Med. J. 100: 837, 2007.
RIEDEL'S THYROIDITIS ("Riedel's struma"; review J. Clin. Endo. Metab. 87: 3545, 2002; Am. J. Clin. Path. 121: 550, 2004)
{49460} Riedel's
A thankfully rare process in which fibroblasts proliferate and lay down collagen, usually as broad, keloid-like bands. Whether this even starts within the thyroid gland, or around it and invades, is uncertain -- it appears to be one of the IgG4 diseases. Most patients are older women, who present with a rock-hard ("woody", etc.) neck mass.
Riedel's does not respect the thyroid capsule, or anything else. (This makes it easy to tell from fibrosing Hashimoto's.) It mimics an invasive sarcoma, but there is no anaplasia or necrosis. Enough of the gland may be destroyed to produce hypothyroidism. Surgical exploration may be required to relieve pressure on the trachea. Fortunately, the disease generally stops before the patient asphyxiates.
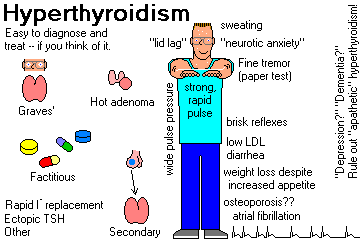
CATEGORIES
PRIMARY HYPERTHYROIDISM means the thyroid gland is over-functioning because of some problem other than excess hTSH.
SECONDARY HYPERTHYROIDISM means the gland is hyper-functioning because it is being overstimulated by too much hTSH, reflecting a primary problem in the hTSH-producing organ. (The most common cause may be ectopic hTSH production by a choriocarcinoma).
TERTIARY HYPERTHYROIDISM means there is too much hTSH because there is too much TRH. It is almost never mentioned in the literature and is probably very rare.
SYMPTOMS AND SIGNS OF HYPERTHYOIRIDISM
HYPERMETABOLISM is manifest by weight loss, muscle atrophy, heat intolerance, increased appetite. Basic thermodynamics tells what's happening: Food is being burned for heat rather than for ATP (i.e., oxidative phosphorylation is being uncoupled). Patients sweat (and their skin feels moist) and develop hyperdynamic pulse.
INCREASED MENTATION may or may not make the person smarter, but it'll make them more anxious and labile ("You're not sick, it's nerves.") In the very elderly, APATHETIC HYPERTHYROIDISM may appear instead, and be mistaken for Alzheimer's.
ENHANCED EPINEPHRINE EFFECT shows as tremulousness and "anxiety". (Try this: Take a sheet of paper and lay it over the backs of the patient's outstretched hands. A very fine fluttering speaks for hyperthyroidism). Blocking the epinephrine receptors with propranolol is a big help while you're stabilizing a Graves's patient prior to definitive treatment.
LID LAG is a delay in downward movement of the upper eyelid as the patient looks down. The upper eyelid tends to be held too high anyway. (This "bug-eyed" appearance is common to all hyperthyroid patients; it is enhanced by the ophthalmopathy of Graves's disease.)
ATRIAL FIBRILLATION (or other atrial rhythm disturbance) is particularly likely to result from hyperthyroidism. (George Bush Sr.'s disease.) There is no consensus on the nature (or even the existence) of HYPERTHYROID CARDIOMYOPATHY.
MILD DIARRHEA may be present.
OSTEOPOROSIS is a very serious long-term complication of hyperthyroidism.
LDL CHOLESTEROL goes down, which is nice as far as the arteries are concerned.
THYROID STORM ("thyrotoxic crisis") is the most dreaded problem in hyperthyroidism. This is development of extreme hypermetabolism, leading to coma and death, when the hyperthyroid patient is subjected to some other major physiologic stress. Untreated, it is usually fatal. Treated, the mortality drops to about 20%.
THE CAUSES OF HYPERTHYROIDISM
* And suppose the labs are all normal? Can a person be making too little thyroid for their personal needs? The rumor that about 25% of people with major depression and normal labs respond dramatically to a bit of thyroid supplementation suggests to me that it's best to "treat the protoplasm, not the numbers."
GRAVES'S DISEASE (NEJM 358: 2704, 2008)
{09235} Graves's
{09237} Graves's
This is a common problem caused by autoantibodies directed against the hTSH receptor. The receptor mistakes them for TSH.
Nobody knows the cause of the autoantibody production. The nature of the disease has been clarified by a good mouse model using either of two monoclonal antibodies that produce somewhat different pictures (J. Immuno. 176: 5084, 2006).
Patients also usually exhibit ophthalmopathy (the usual "lid lag", etc., of hyperthyroidism, plus weak eye muscles plus excess collagen and ground substance behind the eyeball ("orbitopathy"), causing PROPTOSIS-EXOPHTHALMOS). There are usually antibodies against both eye muscles and against selected fibroblasts (behind the eyes, on the shins).
{09355} Graves's exophthalmos
{09356} Graves's exophthalmos
To complete the triad, patients often exhibit myxedema-like nodules confined to the anterior aspects of the lower extremities ("pretibial myxedema").
* Try a generous dose of a topical glucocorticoid for the pretibial myxedema (J. Clin. Endo. Metab. 87: 438, 2002).
{09360} pretibial myxedema
{25470} pretibial myxedema
{25471} pretibial myxedema
{25472} pretibial myxedema
Whether or not the complete triad is present, "Graves's" is the usual cause of DIFFUSE TOXIC GOITER (weight up to 100 gm, seldom more, since there's little colloid). You're likely to hear a bruit over the gland (why?), and at surgery (oops), untreated Graves's will be beefy red.
If you examine an untreated Graves's thyroid gland under the microscope ("uh-oh!"), you'll see scanty colloid, typically being actively resorbed ("bite marks", "scalloping") around its edges.
{24717} Graves's with scalloping
If the patient has been pre-treated with a goitrogen, you'll less colloid and more papillary formations (why?) If the patient has been treated with a huge dose of iodine to suppress thyroid hormone formation, you'll see a colloid goiter (why?)
Today, most patients prefer to take a drink of I131, though they know this will eventually make them hypothyroid. The ophthalmopathy may require an ophthalmologist's care.
NOTE: Sometimes antibodies merely block the effects of hTSH. This may be seen in both Hashimoto's disease and in "primary idiopathic hypothyroidism". Not rare, and may self-cure. NEJM 326: 513, 1992.
ATROPHY OF THE THYROID
|
|
{17447} burned-out thyroid; this could be anything from old I131 injury to old Hashimoto's to Riedel's to a really gone patch in a nodular goiter.
|
Every so often, at autopsy of an adult, the thyroid is shrivelled to a miniature thyroid-shaped nubbin of white scar tissue, weighing perhaps a gram. Trying to guess the cause is fun but usually futile.
If you see giant nuclei and hyalinosis of small arteries, perhaps the patient forgot she had once taken a drink of I131. Other cases may be burned-out Hashimoto's or DeQuervain's. Of course, if there's no pituitary gland, the thyroid may have died of under-stimulation.
* Future pathologists: the rare AMYLOID GOITER features amyloid AA and often extensive fatty ingrowth. It remains a minor mystery of medicine. See Arch. Pathol. Lab Med. 124: 281, 2000.
|
DIFFUSE NONTOXIC GOITER ("colloid goiter") / (MULTI)NODULAR GOITER
{21053} colloid goiter
|
![]() Thyroid gland with diffuse hyperplasia
Thyroid gland with diffuse hyperplasia
What could this be?
Wikimedia Commons
![]() Big inactive follicles
Big inactive follicles
Nodular goiter / Could be other things too
WebPath Photo
Diffuse enlargement of the thyroid gland was historically due to EPIDEMIC GOITER, caused by lack of iodine in the diet (i.e., any community far from the seashore). This was often exacerbated (or even primarily caused by) goitrogens in the diet.
WARNING: The iodine-deficiency thyroid gland is under heavy TSH stimulation (why)? When an iodine-deficient patient is treated with a large amount of iodine, acute hyperthyroidism and even hyperthyroid crisis can supervene. This is the dread JOD-BASEDOW phenomenon.
When iodized salt is introduced into a region that is significantly iodine-deficient, the number of people being treated for hyperthyroidism seems to increase, then drop to the usual within six years (the Danes: J. Clin. Endo. Metab. 94: 2400, 2009) as goitrous thyroids that have been in overdrive for years settle back down. Beyond this, I am not aware of any reason to believe that the obscure WHO claim that too much iodine in the diet cases hyperthyroidism is true.
* SPORADIC DIFFUSE GOITER, once mysterious, is now known to be (at least in many cases) the result of incomplete inborn errors of metabolism. These include (1) partial inability of stomach or thyroid to take up iodine; (2) partial lack of peroxidase to link iodine to tyrosine (fairly common... J. Clin. Endo. Metab. 93: 627, 2008); (3) partial inability to recycle iodine in the thyroid gland; (4) partial inability to crunch the two iodotyrosine moieties together to make T4. Others are described.
A small diffuse goiter is almost the rule rather than the exception around menarche.
Early in its development, the colloid goiter shows hyperplasia (i.e., tall cells, maybe piling-up) under the influence of TSH. Later, the cells appear to give up, and the gland becomes a mass of oversized, colloid-packed follicles. Of course, the process is never really uniform, and eventually the diffuse nontoxic goiter turns into a MULTINODULAR GOITER. By the time the gland reaches over 100 gm, the multinodular stage is usually well-underway.
In a multinodular goiter, there are many nodules, most composed of follicles more or less filled with colloid ("adenomatous nodules"), others representing sites of old hemorrhage and fibrosis ("Feel my goiter!" "Oops, I bumped my neck!") You can see squamous metaplasia, foam cells, masses of hemosiderin, foreign-body granulomas, and many other interesting things.
Rule: If the excised portion of thyroid contains two "adenomas", go ahead and call it a nodular goiter.
A microscopic survey of a nodular goiter is enough to make anyone think about selection of mutant clones in precancer seriously, and this is supported by the finding that many genetically distinct clones of cells with various functional problems. (Clonality in the nodular goiter revisited: Am. J. Path. 134: 141, 1989; hot-spot ras mutations in goiter nodules: Mol. End. 4: 1474, 1990 -- there's been little attention since). Previous irradiation greatly increases the prevalence of nodular goiter (Surgery 150: 869, 2011). However, the common genetic basis remains obscure. (J. Clin. Endo. Metab. 87: 4264, 2002). One locus is known but it's uncommon (JAMA 305: 68, 2011). Multinodular goiter often arises de novo, either sporadically or in certain anti-oncogene deletion syndromes (notably Cowden's).
Usually there are no new functional problems with the thyroid gland in multinodular goiter, but sometimes a clone of cells may turn "hot", causing hyperthyroidism. Fortunately, carcinoma very seldom arises in multinodular goiter, and most "cold nodules" removed from thyroid glands turn out simply to be sleepy nodules from multinodular goiters.
No one really knows how to manage cancer risk in a thyroid with several nodules. Of course, if there are just a few, there will be a lot of fine-needling, but when there are massive numbers, controversy remains (J. Clin. Endo. Metab. 91: 3411, 2006).
|
|
|
|
|
THYROID ADENOMAS
{24724} thyroid adenoma, gross
{13363} thyroid adenoma, gross
{09248} thyroid adenoma, gross
{09250} thyroid adenoma, gross
{09777} thyroid adenoma, gross
{39965} thyroid adenoma, gross
{49453} thyroid adenoma (center has liquefied)
{49454} thyroid adenoma
{19523} thyroid adenoma, histology
{19529} thyroid adenoma, histology
Thyroid neoplasia is an area in pathology that is fraught with problems (review Arch. Path. Lab. Med. 132: 622, 2008). "Experts" still disagree about many lesions. The World Health Organization recently issued another histologic classification; don't worry about it.
In addition to radiation, diseases of the thyroid that cause proliferation of epithelial cells (as you'd expect -- iodine deficiency, nodular goiter, Hashimoto's, Graves') increase the risk for cancer (J. Clin. Endo. Metab. 97: 2661, 2012; papillary and follicular carcinomas arising in a background of Hashimoto's tend to be less aggressive: J. Clin. Endo. Metab. 98: 2409, 2013; if the background is Graves' it tends to be more aggressive J. Clin. Endo. Metab. 98: 1014, 2013).
It is certain that in the not-too-distant future, thyroid lesions will be classified largely by their genetic signatures, as leukemias and lymphomas are today (J. Clin. Endo. Metab. 93: 3286, 2008). Update Ann. Surg. 262: 519, 2015.
The vast majority of dominant thyroid nodules are either benign adenomas or just big nodules in a multinodular goiter. This is good, because thyroid nodules are very common (around 5,000,000 in the U.S.) You'll learn to manage these clinically. Most patients are adults, and there is a modest female preponderance.
As you would expect, thyroid adenomas are composed of thyroid follicles ("follicular adenomas"). The follicles may be tiny (* "fetal" / "microfollicular"), shelf-like ("trabecular" / "embryonal"), or solid. Don't worry about the useless subclassification given in "Big Robbins"; they all behave pretty much the same, i.e., they are harmless or might perhaps make excess T4 and/or T3.
* A lone patch of "adenomatous hyperplasia" of multinodular goiter can't really be told from follicular adenoma. If there's just a couple... hyperplastic nodules supposedly don't compress surrounding thyroid like adenomas do, and hyperplastic nodules often have fibrous bands crisscrossing them. It makes no real difference to the patient.
* The major pathologist-fooler is the "hyalinizing trabecular adenoma", with balls of cells embedded in shelves of basement membrane; it can include psammoma bodies and orphan-annie eye nuclei, and has an immunostaining profile similar to papillary carcinoma. Leave diagnosing it to us (stain Am. J. Clin. Path. 122: 506, 2004; there are metachromatic blobs). It has both a benign and malignant (i.e., capsular invasion) form -- or perhaps all of them are "malignant neoplasms of low metastatic potential" (Am. J. Surg. 193: 707, 2007). Ultra-hard-core pathologists recognize a unique membrane-and-cytoplasm distributin of MIB-1 antigen.
* Hyperfunctioning nodules, not surprisingly, often have (Nowell's law) gotten mutated TSH receptors stuck in the "on" position: J. Clin. End. Metab. 81: 1584, 1996; we can assume the ones that don't have something else wrong in the cAMP signal pathway.
T3 toxicosis usually means adenoma. Why? Hint: Think of Nowell's Law.
Less often, one gets unusually big, or causes pressure symptoms.
* Fine-needle aspiration and molecular profiling together have made frozen-section examination of thyroid nodules during surgery obsolete (Arch. Otol. 133: 874, 2007).
Fortunately, the genes that cause adenomas don't seem to be the same ones that produce thyroid carcinomas, and thyroid adenomas have virtually no tendency to turn malignant. (* You may see slight atypia in these tumors. Let the pathologist worry about it.)
You can remove adenomas surgically, or suppress them by using thyroxine to suppress TSH. (Ignore "Big Robbins" about how adenomas should "theoretically" be "autonomous"; the idea that "tumors are free of controls on their growth" is rank superstition.)
* Ask a pathologist whether he or she has ever seen a C-cell adenoma. No follicles, cells may spindle, and stain for calcitonin.
PAPILLARY ADENOCARCINOMA ("Orphan Annie's Tumor"; Arch. Path. Lab. Med. 130: 1057, 2006)
{24725} papillary carcinoma, gross
{24723} papillary carcinoma, histology
{26792} papillary carcinoma, histology
{26795} papillary carcinoma, histology
{26798} papillary carcinoma, histology
{20291} world's smallest papillary thyroid cancer
This is a common (the commonest endocrine cancer), often-multifocal (separate primaries NEJM 352: 2406, 2005) cancer, fairly common in adults with a female predominance (maybe 75%), and not unknown in children.
The harder you look for papillary carcinoma of the thyroid, the more you find. The "greatly increased rate" seen in autopsies of Hiroshima survivors was probably real, though these glands were meticulously sectioned in search of small cancers.
There's no question that irradiating the thyroid gland (for a good reason or for "big thymus", tonsils, acne, or what-have-you) gives an increased rate of papillary (and probably follicular) carcinoma; the increased risk from radioactive iodine therapy of Graves's is very small. The risk from external beam radiation continues for life (Endo. Metab. Clin. N.A. 19: 495, 1990), with cancers typically appearing decades later. In the past, radiation-induced cancers (as from thymic radiation) seemed to be tame (Arch. Ped. 148: 260, 1994). But don't expect them to remain dormant (Ann. Surg. 239: 536, 2004). Atom bomb survivors have many papillary carcinomas, mostly trivial (Cancer 116: 1464, 2010). Chernobyl's children and their papillary thyroid cancers: Cancer 74: 748, 1994. The fact that many children, but few adults, got papillary carcinomas after the incident suggests youngsters are more susceptible to radioactive iodine. Nowadays, they seem a bit more aggresive than the others (Arch. Otol. 135: 355, 2009). The cancers are continuing to develop, and a few are proving aggressive (Cancer 107: 2559, 2006).
It's finally been pretty well established that Hashimoto's disease, with ongoing destruction and regeneration of the epithelium, triples one's risk for well-differentiated thyroid cancer (J. Am. Coll. Surg. 204: 764, 2007).
The most-often-mutated known gene in papillary cancers turns out to be the serine-threonine kinase BRAF (Hum. Path. 36: 694, 2005; maintains malignancy J. Clin. Endo. Metab. 92: 2264, 2007); there is a signature mutation V600E / T1799A (notably in radiation-induced tumors -- J. Clin. Inv. 115: 94, 2005; stain Am. J. Surg. Path. 36: 844, 2012), and regardless of history, mutation imparts a much worse prognosis and probably the need for more aggressive early therapy (J. Clin. Endo. Metab. 90: 6373, 2005; Cancer 110: 38, 2007; Cancer 110: 1218, 2007; J. Clin. Endo. Metab. 95: 4197, 2010; JAMA 309: 1493, 2013). Update on Braf testing for fine-needle aspirates: J. Clin. Endo. Metab. 97: 2299, 2012; Annals Surg. 255: 986, 2012. In the near future, we will probably see BRAF-positive thyroid cancers treated with the new tyrosine-kinase inhibitors (Br. J. Cancer 96: 16, 2007).
In the 1990's, it was discovered that the cancer has its several distinctive oncogenes, PTC-1, -2, and -3, which turned out to be particular rearrangements of the tyrosine kinase receptor RET (Endocrinology 137: 375, 1996; J. Clin. End. Metab. 81: 3360, 1996; update Cancer 104: 943, 2005) with various other genes. Watch these also as therapeutic markers / targets.
* The less-well-known oncogene PTTG is also commonly mutated and imparts a worse prognosis in both papillary and follicular carcinoma; staining for the activated form is available (J. Clin. Endo. Metab. 91: 1404, 2006). Work is ongoing.
Fusion genes are better-known from sarcomas and lymphomas, but the CCDC6-RET fusion gene is seen in many papillary thyroid carcinomas (update J. Clin. Path. 63: 4, 2010).
In most cases of papillary thyroid carcinoma, the genome is not destabilized (Arch. Path. Lab. Med. 131: 65, 2007). We might reasonably think that in those unusual cases in which it does destabilize, anaplastic carcinoma results. See below.
In the thyroid, malignancy is based on nuclear changes, and ironically, the cell arrangement of a "papillary carcinoma" is not a factor in making the call. The usual histology is that of a papillary adenocarcinoma (i.e., inside-out glands growing like a tree, the stalk being the trunk and branches, the cells being the leaves.) A good rule: Any reasonably well-differentiated thyroid tumor with any papillary area will act like a papillary carcinoma of the thyroid. (Even if there are also follicles: Arch. Surg. 138: 1362, 2003; Cancer 97: 1181, 2003; and many more).
Pathologists usually (but not always) see the "Orphan Annie eye" nuclei, with the heterochromatin all pushed to the edge and the central areas of the nuclei optically clear. (Annie was, of course, a character in a comic strip where no one had irides or pupils.) These nuclei have marginated chromatin and optically clear centers. It's a fixation artifact. Another good rule: Any reasonably well-differentiated thyroid tumor with Orphan Annie nuclei (or the other features mentioned below) will act like a papillary carcinoma of the thyroid.
Other helpful features include cytoplasmic invagination into a nucleus ("intracytoplasmic pseudoinclusions", for cytopathologists). This is impressive, especially on fine needle aspirates and electron microscopy. This is another criterion for malignancy, though contrary to what you may hear, it is not the cause of "Orphan Annie Eyes". Yet another is several micro-nucleoli right underneath the nuclear membrane; still another is nuclear grooving ("coffee beans").
* Ask your local pathologist to show you other features. Future pathologists: Any cell (and notoriously, endocrine cells and healthy lymphocytes) that is poorly-fixed prior to tissue sectioning can exhibit an "orphan annie eye nucleus".
Another favorite finding is psammoma bodies. Again, these suggest the tumor will behave like papillary carcinoma.
* Future pathologists: You see these in normal chorioid plexus, normal pineal, papillary carcinoma of the thyroid, serous cystadenocarcinoma of the ovary, meningioma, and somatostatinoma.
Except for a few uncommon subtypes, these lesions are noted for being non-aggressive, especially in patients young than age 40. Even when first diagnosed as a metastasis in a cervical node, survival is likely (Surgery 143: 35, 2008). Like most carcinomas, it prefers the lymphatic route, and can ultimately spread by the bloodstream.
Despite its usually gentle nature, papillary carcinoma does occasionally kill people, typically by asphyxiation. It would be insane to "just watch" even a small one (Cancer 121: 1017, 2015). It is also the breeding ground for anaplastic carcinoma of the thyroid.
The diffuse sclerosing form presents as a goiter composed entirely of papillary cancer. The abundant psammoma bodies impart a remarkable gritty feel when cut. It's more likely to be in the lymph nodes at presentation than other forms of papillary cancer, but the prognosis is still generally good (Eur. J. Surg. Onc. 29: 446, 2003).
The tall-cell variant (around 10% of tumors) features very tall pink cells, oncogenic met, and a greater metastatic potential (Cancer 98: 1386, 2003). Most are BRAF V600E positive.
* The columnar-cell variant is also aggressive. It's seen in older folks and unlike the other variants doesn't have the classic orphan-annie nuclei; instead the cells look like those of colon adenomatous polyps. About half of these light up for CDX2, unlike other thyroid cancers (Am. J. Clin. Path. 137: 722, 2012).
* The solid variant (rare, but with obviously infiltrating borders) is also more somewhat aggressive but has the same genes (Am. J. Surg. Path. 25: 1478, 2001).
* Future pathologists only: The picturesque cribriform-morular variant of papillary carcinoma warns that the patient likely has familial polyposis coli / Gardner's (Am. J. Path. 115: 486, 2001; Am. J. Clin. Path. 128: 994, 2007); it is mutant-BRAF negative (Arch. Path. Lab. Med. 133: 803, 2009).
* Sclerosing variant: Cancer 66: 2306, 1990. Other variants that probably have no prognostic significance include clear-cell, Hurthle-cell, and Warthin-like. Keratin 19 as marker for papillary carcinoma (Am. J. Clin. Path. 92: 654, 1989) and histologic grading (aggressive vs. non-aggressive): Am. J. Clin. Path. 101: 651, 1994) have given way to molecular markers.
* There is a familial syndrome; the gene has still not been found (World Surg. J. 24: 1409, 2000; J. Clin. Endo. Metab. 90: 5747, 2005; Surg. 145: 100, 2009), but contrary to older reports the familial variant isn't more aggressive than the sporadic. in any case having a family member affected increases your own risk by about a factor of ten J. Clin. Endo. Metab. 90: 5747, 2005). Several classic anti-oncogene deletion syndromes supposedly place one at increased risk, but these account for only a very small minority of cases.
|  |
* Watch for Tc99-sestamibi as a new way to detect metastatic papillary thyroid carcinoma (also breast, oat cell, and of course parathyroid).
Relative frequency of detected thyroid carcinomas (older data):
Papillary... 65-80% of primary thyroid carcinomas; the large majority (90+%) will not die of it
Follicular... 10-25% of primary thyroid carcinomas; maybe 50% will eventually die of it if it is "frankly invasive" at diagnosis, though it may be much later than 5 years
Medullary... 5% of primary thyroid carcinomas; 50% 5-year mortality if sporadic (probably less nowadays), much better if you picked it up early as part of workup of a family
Anaplastic... 5% of primary thyroid carcinomas; almost all will die of it in a few months
* A reputed increase in thyroid cancer in the United States over the past 30 years seems to be due to increased detection of small papillary carcinomas that probably wouldn't have killed the person anyway. The percentage of all deaths that are deaths due to thyroid cancer remains the same (JAMA 295: 2164, 2006 -- remember that we're probably curing more thyroid cancers and people are surviving other once-fatal diseases as well, so things balance.)
* Older work: It's claimed that dipeptidyl aminopeptidase IP stain of cytology preparations distinguishes benign follicular cells (negative) from malignant ones (positive): Am. J. Clin. Path. 96: 306, 1991; Diag. Cyto. 19: 4, 1998; still holding up Arch. Surg. 139: 83, 2004. this seems to work but isn't in widespread use. However, there's a consensus that CK19 (cytokerain 19) positivity is sensitive for malignancy, and that HBME-1 positivity is specific, but not particularly sensitive, for carcinoma when staining thyroid lesions; galectin-3 (GAL3) (Am. J. Clin. Path. 126: 700, 2006) is in-between. They also work for fine needle aspirates (Cancer Cytopath. 105: 87, 2005). Well, maybe.
FOLLICULAR ADENOCARCINOMA (pathologists see Cancer 100: 1123, 2004)
This is a more aggressive thyroid carcinoma that generally makes follicles. Iodine deficiency is a well-established risk factor for follicular carcinoma (the hyperplasia allows overgrowth of mutated clones), and it remains rampant in Africa's goiter belt (Am. J. Surg. 200: 462, 2010).
* Watch the newly-discovered tumor-suppressor gene HABP2 -- its G534E mutation in the germline produces a familial non-medullary thyroid cancer syndrome (NEJM 373: 448, 2015).
Grossly, it may be obviously malignant, or there may be metastases. More often, malignancy is established by demonstrating that a thyroid nodule contains groups of cells invading BLOOD VESSELS (not lymphatics) in the capsule or just beyond; for some reason, this particular cancer prefers the vascular route of invasion. The rules also specify that the invaded blood vessel be within or just outside the capsule.
Since the surgeon will take one lobe for a follicular adenoma (common), and probably do a total thyroidectomy for a follicular carcinoma (much less common), there's been much discussion of "the best way to tell at surgery".
The genetics are being worked out; the fusion gene known from follicular carcinomas is PAX8/PPAR-gamma (J. Clin. Path. 63: 4, 2010; adenomas don't have it; the other common mutated gene in follicular carcinomas is ras and the two mutations do not occur together).
Unlike papillary carcinoma of the thyroid, with its distinctive weird nuclei, the nuclei of a follicular carcinoma tend to be bland-looking. The distinction between benign and malignant is made on the apparent pattern of growth (i.e., invasiveness), and is notoriously difficult.
If the tumor invades through (not just into) its "capsule", this is also a criterion for malignancy, though it is far less ominous than vascular invasion.
There are no good fibrovascular papillae, Orphan Annie nuclei, or psammoma bodies. The tumor cells often take up radioactive iodine, which is useful both in scanning for metastases and for treating them (clinical review Cancer 95: 488, 2002; especially in the young, radio-iodine therapy is often curative even in metastatic disease J. Clin. Endo. Metab. 91: 2892, 2006). This tumor (and papillary carcinoma) may be modestly hTSH dependent, and thyroid hormone administration may suppress them temporarily.
* The Hürthle-cell variant isn't much different from the more common form (Cancer 106: 1669, 2006). However, telling benign from malignant can be tricky; one group suggests that those with the ret/PTC gene rearrangements specific to papillary carcinoma of the thyroid be treated by full thyroidectomy regardless of histology (Arch. Otol. 132: 54, 2006).
Of course, pathologists hate this lesion, as it's difficult to tell from one of the much-more-common follicular adenomas / hyperplastic nodules (or for that matter, medullary carcinoma with a follicular growth pattern). There is a "minimally invasive subtype", detected by its pushing all the way (or part-way, there's disagreement) through a very thick capsule; it has a very good prognosis (Cancer 91: 505, 2001) that the Chernobyl group proposes calling "well-differentiated thyroid tumor of uncertain malignant potential" (Int. J. Surg. Path. 8: 181, 2000). Again, if the nuclei say "papillary carcinoma", that's what you diagnose. Criteria for handling follicular lesions Am. J. Clin. Path. 117: 143, 2002. The ongoing difficulty diagnosing the follicular lesion of the thyroid: Arch. Path. Lab. Med. 130: 984, 2006.
The prognosis for any lesion that you think might be follicular carcinoma is always guarded. This tumor tends to metastasize to lungs (via veins, of course) and bone.
{09255} follicular carcinoma of thyroid, histology. Trust me, this was invading a vessel
{39838} follicular carcinoma of thyroid, histology. Trust me, this was invading a vessel
MEDULLARY ADENOCARCINOMA (Surg. Clin. N.A. 75: 405, 1995; Am. J. Med. 103: 60, 1997).
This is cancer of the C-cells (or at least differentiating as C-cells; see Cancer 74: 928, 1994). Its stroma is usually (* not always) laced liberally with calcitonin pleated into amyloid.
As you remember, this cancer is caused, at least in part, by loss of both copies of the MEN-II anti-oncogene on chromosome 10. As you'd expect, in MEN-II it is very common and often multifocal, and occurs at any age.
Sporadic cases (older folks; at least 80% of medullary carcinomas are sporadic despite the famous link to MEN-II) also lack the protective genes. With the cloning of the RET gene (the MEN-II gene), we've discovered different alleles producing different complexes (J. Clin. End. Met. 79: 590, 1994; J. Clin. End. Metab. 81: 1780, 1996), some families get only medullary carcinoma (Nature 367: 319, 1994; J. Clin. Endo. Metab. 87: 1674, 2002). We can test people for the gene (Surgery 116: 124, 1994) and prophylactic thyroidectomy is now routine (J. Am. Coll. Surg. 195: 159, 2002). Pathologists enjoy looking at the hyperplastic C-cells, and the patients do extremely well after removal (Arch. Path. Lab. Med. 132: 1767, 2008).
* Does liraglutide, the glucagon-like peptide I analog used in the treatment of diabetes, put a person at increased risk for medullary carcinoma of the thyroid. I don't know. Neither does anybody else. Ask a lawyer.
Medullary carcinoma tend to be a slow-grower, with stage at surgery and calcitonin levels shortly after surgery the only prognosticators: Cancer 77: 1556, 1996. Nowadays, we determine at the time of surgery whether we got the entire tumor by a rapid determination of serum calcitonin 30 minutes after surgery (J. Clin. Endo. Metab. 95: e32, 2010).
* Medullary thyroid microcarcinoma, a tiny cancer found at a fancy medical center on the basis of discovering an elevated serum calcitonin -- perhaps in someone with known MEN-II -- is very much worth finding and removing (Cancer 118: 620l 2012; J. Clin. Endo. Metab. 97: 1547, 2012).
* Don't worry about the rare "medullary adenoma", seen only in MEN-II.
As befits cancer of the C-cells, the tumor often makes calcitonin. In extreme cases, tetany may result.
Today's diagnosticians typically rely on seeing how high the serum calcitonin can be made to go following pentagastrin administration ("stimulation test"): Surgery 142: 1003, 2007.
Medullary carcinoma patient may also get production of ACTH (Cushingism), VIP (diarrhea), serotonin (instant carcinoid syndrome), and a variety of other things.
{49355} medullary carcinoma of thyroid, gross
{49356} medullary carcinoma of thyroid, gross
{49366} medullary carcinoma of thyroid, gross. Of course, you couldn't diagnose any of these four
without histology.
{09265} medullary carcinoma of thyroid, histology
{09266} medullary carcinoma of thyroid, histology
{37160} medullary carcinoma of thyroid, histology; Congo Red stain
{37163} medullary carcinoma of thyroid, histology; crystal violet stain (amyloid is scarlet, all else is
Navy Blue)
Future endocrinologists: Anybody you suspect of harboring MEN-II gene (i.e., they have a personal or family history of hyperparathyroidism, pheochromocytoma, mucosal neuromas, and/or medullary carcinoma of the thyroid) needs a check. The old technique was to infuse calcium and/or pentagastrin; a brisk rise in blood calcitonin means pre-malignant hyperplasia of C-cells, and you need to do something about it. All about provocative calcitonin testing: Am. J. Hum. Genet. 52: 335, 1993; nowadays of course we check for the mutated RET gene.
* People with C-cell hyperplasia are likely to have elevated serum calcitonin (usually asymptomatic). The RET mutation is the usual cause; mutated succinic dehydrogenase can also do this but does not seem to lead to actual neoplasia (J. Clin. Endo. Metab. 88: 4932, 2003)
Nowadays, anyone found to be at risk because of a mutated RET gets a total thyroidectomy, and removal of the regional lymph nodes if the calcitonin stays up (Surgery 146: 906, 2009). This seems to be the right approach.
POORLY DIFFERENTIATED THYROID CANCER is a new category convincingly defined in 2006 (Cancer 106: 1286, 2006).
The best known type is "insular thyroid carcinoma", composed of cancer cells with prominent nucleoli, surrounded by fibrous tissue (update Cancer 118: 3260, 2012).
There's also a trabecular variant.
* Hurthle cell carcinoma as possibly a genetically distinct thyroid cancer with a poor prognosis: J. Clin. Endo. Metab. 98: E962, 2013.
ANAPLASTIC ADENOCARCINOMA ("undifferentiated carcinoma")
Very, very ugly, both histologically and clinically. We believe that most of these tumors arise in a previous papillary or follicular thyroid carcinoma (Nowell's law triumphant); this has been confirmed by genetic studies (Cancer 103: 2261, 2005).
Thyrotoxicosis (from overproduction of thyroid hormone by the cancer) is uncommon but does happen (J. Lar. Ot. 121: 695, 2007).
Even a tiny focus of anaplastic carcinoma in a papillary thyroid cancer is ominous (Surgery 154: 106, 2013).
* Ignore the subclassification of the old WHO system. The "small cell anaplastic carcinomas" were really lymphomas; only of the "large cell anaplastic carcinomas" were actually carcinomas.
Today, we distinguish "spindle cell" (looks like sarcoma but still lights up with keratin), "giant cell", and and "squamoid". All are obviously malignant. There are many variations of the theme of anaplasia (Arch. Path. Lab. Med. 111: 1169, 1987; these tumors generally light up with both keratin and vimentin). Fibrotic anaplastic carcinoma mimicking Riedel's: Am. J. Clin. Path. 105: 388, 1996.
* Even the oncologists are talking about offering these patients hospice rather than chemotherapy at diagnosis (J. Clin. Endo. Metab. 97: 2566, 2012).
{09264} anaplastic carcinoma of thyroid, histology
{37004} anaplastic carcinoma of thyroid, cytology
![]() Anaplastic carcinoma of the thyroid
Anaplastic carcinoma of the thyroid
Clear vascular invasion
Pittsburgh Pathology Cases
PRIMARY THYROID LYMPHOMA (J. Clin. Endo. Metab. 98: 3131, 2013) is an uncommon B-cell neoplasm, usually of the MALToma family, arising usually in Hashimoto's (molecular precursor lesions in the Hashimoto lymphocytes: J. Clin. Path. 61: 438, 2008). Look for malignant lymphocytes inside the follicles. Hashimoto's often has clones of lymphocytes, and these tend to be the ones that give rise to lymphoma (no surprise: J. Clin. Path. 61: 48, 2008).
{10934} lymphoma of the thyroid
{10937} lymphoma of the thyroid
THYROID TESTING (see Lancet 357: 619, 2001)
Serum T4 will give you the total bound plus unbound (the unbound fraction is of course the active fraction). Serum free T4 will give you the unbound, but it is more expensive. Serum T3RU (T3 resin uptake) is an unfortunately-named test that gives you a value inversely proportional to the number of unbound sites on the serum thyroid hormone carrying proteins (remember them?) Multiply T4 and T3RU to get "free thyroxine index", a measure of the biologically active hormone.
Quiz: Who remembers what proteins carry T4 and T3? Answer: Thyroxine-binding protein (TBG, lion's share), transthyretin ("prealbumin"), and albumin. What's the best way to raise TBG? Take estrogen. What does this do to total T4? T3RU? Free T4? TSH? Genetic TBG deficiencies exist -- J. Clin. Endo. Metab. 100: E173, 2015.
Serum T3 of course measures the active hormone. You can get a serum free T3 also. Some toxic nodules make T3 instead of T4, so it's often worth checking (Am. J. Med. 96: 229, 1994).
Quiz: Suppose somebody took T4 to lose weight and got sick it ("factitious hyperthyroidism"). How would the tests be affected? Suppose the person took pure T3 instead?
The newer, super-sensitive TSH assays are a good way to screen for hyperthyroidism (TSH in primary, in secondary or tertiary) and hypothyroidism ( in primary, in secondary or tertiary). Some people say that patients may actually be suffering from symptomatic thyroid disease if hTSH is abnormal but T7 is in the normal range (i.e., "not everybody has the same 'normal' thyroid hormone levels".) hTSH has long been the best screen for congenital hypothyroidism. (There are now calls for additional screening to detect congenital secondary hypothyroidism, which of course looking for a high hTSH will miss: J. Clin. Endo. Metab. 90: 3350, 2005; and as we've seen hTSH misses a few birth defects). After treating hypothyroidism, give the TSH 4-8 weeks to settle back into its new equilibrium.
Nowadays, we talk about "subclinical thyroid disease" defined to be a hTSH outside the normal range, free thyroxine and free triiodothyronine in the normal range, and no symptoms or signs. It often declares itself as real thyroid disease in a few years, but so far, no one knows what to do about it (Am. Fam. Phys. 72: 1517, 2005).
* Future pathologists only: People still die of thyroid storm, especially if they don't know they have Graves's and get some other kind of stress. T3 and T4 often de-iodinate rapidly after death, but TSH levels are pretty steady for at least the first 48 hours.
On thyroid scans, cold nodules are the ones most likely to be malignant (why?) Hot nodules are the ones most likely to produce hyperthyroidism. You'll learn how to manage both on rotations. In hyperthyroidism due to most causes, the gland will be hot, but in struma ovarii -- overactive thyroid in an ovarian teratoma --, DeQuervain's, or factitious hyperthyroidism, it will be cold (why?)
Serum thyroglobulin will often be increased in thyroid cancers (papillary, follicular) or in DeQuervain's (why?). For use of thyroglobulin in detecting the spread of well-differentiated thyroid carcinoma, see the update from Mayo's at J. Clin. Endo. Metab. 92: 4278, 2007; also J. Clin. Path. 62: 402, 2009 (the assay is a difficult and problematic one). It's common to give radio-iodine to ablate well-differentiated thyroid cancer; if afterwards the serum thyroglobulin is lowish, the prognosis is good (J. Clin. Endo. Metab. 97: 2754, 2012).
When you are monitoring thyroid hormone replacement in somebody who has been hypothyroid, the conventional wisdom is to try to avoid their becoming even a little bit hyperthyroid, since this will supposedly lead to osteoporosis in the long run. However, some people actually do not feel well until the free T4 is somewhat above the upper limit of normal (Br. Med. J. 326: 295, 2003), and I'd trust the body's wisdom on this. Currently, clinicians make sure that hTSH stays in the normal range. If, on the other hand, you are administering thyroxine to suppress a hTSH-dependent thyroid cancer, be sure that you give enough so that hTSH levels remain zero.
During serious illness or injury, some people have diminished intracellular conversion of T4 to T3 by the deiodinases.
EUTHYROID SICK SYNDROME ("low T3 syndrome"; "the non-thyroidal illness syndrome") is recognized, for research purposes, in patients who are seriously sick with something serious have low T3's and high rT3's (i.e., T4 is getting metabolized wrong). hTSH levels tend to stay in the okay range. It is a real entity (J. Clin. Endo. Metab. 90: 5613, 2005), is very common in the very-sick and the malnourished if you look for it, is seen if you look hard in maybe 1/3 of really sick psych patients (Am. J. Psych. 169: 127, 2012). and (at least in ICU patients on the ventilator) somewhat ominous overall (Chest 135: 1448, 2009). And it will confuse you when you are caring for the very-sick. The conventional wisdom is that you do not treat it (i.e., you do not administer extra T4 or T3); not everybody agrees (Am. Heart. J. 135: 187, 1998; discussion is ongoing). There are so many proposed explanations for "euthyroid sick syndrome" that I urge you not even to start trying to figure it out.
* One more pitfall -- a few people have an antibody against TSH that causes the lab to measure very high levels despite the person being euthyroid (macro-TSH; J. Clin. Endo. Metab. 97: 1823, 2012). The pathologist can help figure this out.
* Now, you are familiar with the selenium-dependent enzymes that turn T4 into usable T3 in the tissues. Deficiencies of course are known; these people seem to do okay but of course have high rT3, low T3, high FT4, and usually normal hTSH (see for example J. Clin. Endo. Metab. 94: 4003, 2009.)
There are two schools of thought on managing thyroid replacement therapy -- by the numbers or by how the patient feels. I have often wondered whether (1) a "normal" serum T4 might still be low for that person, and whether (2) a "normal" serum T4 might not mean a normal T4 in the brain milieu. Physicians who fear being sued decades later for "causing osteoporosis" are reluctant to approve patients who feel best when they take a bit more thyroxine than "the lab tests say they need". I'm not a clinician, but we have a saying in pathology, "Listen to the patient, not the numbers." I'm not alone (Br. Med. J. 320: 1332, 2000; Br. Med. J. 326: 295, 2003)
* This brings us to a late 1990's fad diagnosis, WILSON'S SYNDROME. Supposedly this results from faulty metabolism of T4 into rT3 at the tissue level. People interested in complementary medicine are invited to take their body temperature repeatedly, and if it is "a few tenths of a degree below 98.6" at any time of the day, and they have any of a huge list of symptoms, then the diagnosis is considered established and the patient gets a series of "complementary" remedies. Before you diagnose or treat yourself or somebody else, please consider these facts:
* Do you remember those deiodinases? Selenium takes the place of sulfur in their cysteines!
In suspected Graves's disease and Hashimoto's disease, you can order a battery of anti-TSH receptor autoantibodies. The first is "thyroid stimulating antibody" / "long-acting thyroid stimulator" / "LATS" / "TSH receptor antibody" / now TRAb. The second is "anti-thyroglobulin antibodies" / now TgAb. The third is "anti-microsomal antibodies" / anti-peroxidase antibodies" / now TPOAb. Interpretation is rather cloudy, though TRAb causes Graves's, and very high titers of anti-microsomal antibodies is pretty specific for Hashimoto's.
* And for some reason that no one understands, up to 10% of women turn positive for at least one of these duing pregnancy. Thyroid hormone levels in pregnancy may drop; you'll learn when and when not to treat on rotations.
If you've got a bump in your thyroid, a pathologist will be happy to FINE-NEEDLE ASPIRATE it, and look at the cells on a slide. Unless the nodule is under 4 cm AND is free of calcifications AND has a perfectly smooth border, you'll probably want to get tissue (Surgery 150: 436, 2011). Review of 4700 cases from Galveston: Cancer 111: 306, 2007 (it's accurate). How to do it right: J. Cln. End. Metab. 79: 335, 1994; Mayo Clin. Proc. 69: 44, 1994; some sub-subspecialty training is advised for pathologists who want to do this (Cancer 107: 406, 2006). Using it with ultrasound to be sure you hit the itty-bitty nodules: Otolar. 123: 700, 2000. The procedure is not perfect, and there are still plenty of false-positives and false negatives; the most common problem is the all-too-human attempt to interpret an unsatisfactory specimen (Am. J. Clin. Path. 125: 873, 2006). Nowadays, we generally operate the tough calls, and this is a good thing as a lot of them are cancer (J. Am. College. Surg. 213: 188, 2011). Bethesda (2007) offered a six-category sytem that was a baffler for me; the feeling afterwards seems to have been to send anybody with a follicular thyroid lesion that wasn't obviously just a nodular goiter to see a surgeon. The Royal College of Pathologists's system seems to be the most popular and reproducible among observers (Thy1, nondiagnostic; Thy2 nonneoplastic; Thy3a atypia probably benign, Thy3f follicular lesion infamously difficult to tell benign from malignant; Thy4 suspicious for cancer; Thy5 cancer.) See Am. J. Clin. Path. 135: 852, 2011; two "nondiagnostic" needlings means "almost certainly no cancer": Am. J. Clin. Path. 135: 750, 2011. In the meantime, molecular diagnostics are now being applied to thyroid fine needle aspirates (BRAF, RAS, RET/PTC, PAX8/PPAR gammma) and this seems to help greatly (Arch. Path. Lab. Med. 135: 569, 2011.) Patients may be concerned that the needling will spread the cancer; this is very rare but does happen (J. Laryn. Otol. 121: 268, 2007.) This is really a screening technique to find out which bumps to cut out, and it is the one instance in which a decision to perform such serious surgery may be based on a few cells in a cytology smear. The practice is now standard, and has greatly reduced the number of people who need to be operated for diagnosis. Update on this now-huge field: CA 59(2): 99, 2009. "The Bethesda System for Reporting Thyroid Cytopathology": Am. J. Clin. Path. 132: 658, 2009; Am. J. Clin. Path. 134: 45, 2010.
Please remember that we CANNOT tell benign from low-grade-malignant follicular lesions of the thyroid using fine-needle aspiration.
Once a thyroid needle biopsy shows something worrisome, there's no reason to "repeat the biopsy" -- the mass comes out (Am. J. Clin. Path. 134: 788, 2010). And if the pathologists are "uncertain", the best rule seems to be, "When in doubt, cut the lobe out" (Surgery 148: 516, 2010 -- today there is very little morbidity from this surgery, which is now done on outpatients.) A surgeon should remove the bump if the fine needle aspirate shows:
|
|
|
BIBLIOGRAPHY / FURTHER READING
I urge anyone interested in learning more about thyroid pathology to consult these standard textbooks.
In my notes, the most helpful current journal references are embedded in the text. Students using these during lecture strongly prefer this. And because the site is constantly being updated, numbered endnotes would be unmanageable. What's available online, and for whom, is always changing. Most public libraries will be happy to help you get an article that you need. Good luck on your own searches, and again, if there is any way in which I can help you, please contact me at scalpel_blade@yahoo.com. No texting or chat messages, please. Ordinary e-mails are welcome. Health and friendship!
Ed says, "This world would be a sorry place if people like me who call ourselves Christians didn't try to act as good as other good people ." Prayer Request

| If you have a Second Life account, please visit my teammates and me at the Medical Examiner's office. |
Teaching Pathology
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |
 |
Click here to
see the author prove you can have fun skydiving without being world-class. Click here to see the author's friend, Dr. Ken Savage, do it right. |
