 Endocrine
Endocrine
Taiwanese pathology site
Good place to go to practice
Presentation: The Patient with a Neck Mass
Title: Thyroid Disease and Testing
Date & Time: Thursday, February 4, 2010 at 10 AM
Lecturer: Ed Friedlander MD
QUIZBANK
Endocrine (It's impossible to separate pituitary, adrenal, thyroid, parathyroid, etc. Look at it all now.)
|
|
|
|
|
|
|
{11803} normal thyroid, gross
{00135} normal thyroid, histology {11755} normal thyroid, histology {00138} goiter {24613} goiter {39460} goiter |
|
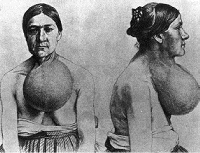 |
Mountaineers dew-lapped like bulls, whose throats had hanging at 'em wallets of flesh... |
 |
INTRODUCTION
This is an easy unit, but you have to do some thinking.
The thyroid begins as a patch on the back of the tongue (at the "foramen cecum"). It descends (down what may become the "thyroglossal duct") into the neck.
The former track may be filled with thyroid tissue, imparting a "pyramidal lobe" to the thyroid (40% or so of thyroids have at least a little one).
Occasionally some or all of the gland ends up in the mediastinum instead, explaining the occasional "retrosternal goiter".
The thyroid sits close to the four (or however many) parathyroid glands (and sometimes encases and thus hides one or more of them), and to the recurrent laryngeal nerves. These structures may be damaged during surgery.
The healthy adult thyroid weighs around 15-25 gm. If you don't remember its histology and physiology (follicles full of colloid, iodine traps, microvilli, parafollicular C-cells, thyroxine=T4, iodotyrosine precursor compounds, triiodothyronine=T3, calcitonin (remember it's from the parafollicular cells that are mostly in the upper lobes), synthesis and endocytosis of thyroglobulin, TRH, TSH=hTSH=thyrotropin, etc.), please review.
HINT: C-cell function is vestigial in humankind, completely dominated by parathyroid function. And don't expect to be able to distinguish the C-cells unless they are hyperplastic (i.e., MEN II, response to chronic hypercalcemia) or immunostained.
When thyroid is active (i.e., winter, puberty, pregnancy, stress, Graves's disease, Jod-Basedow) or just overstimulated (propylthiouracil or other thiourea that inhibits peroxidase, thiocyanate that inhibits the iodine pump), the cells will become taller and thyroglobulin will be reabsorbed. You may even see the overabundant cells piled up as little papillae (really "pseudopapillae", as they lack fibrovascular cores; why?)
{08959} propylthiouracil effect
{24718} propylthiouracil effect
When thyroid is inactive (i.e., no TSH or other stimulation, or there is excessive iodine that as you remember strongly inhibits lysis of thyroglobulin), the cells flatten down and the amount of colloid increases.
{24719} high-dose iodine effect
Most thyroids removed surgically have "palpation thyroiditis", a mix of fibrosis and granuloma typically inside follicles. It's a non-problem.
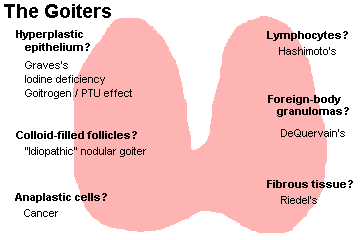
Any enlarged thyroid (i.e., over maybe 50 gm) is a GOITER (or STRUMA). Areas of thyroid that are mostly colloid (i.e., colloid-rich adenomas, colloid-rich nodules, glands poisoned by excess iodine) will look gelatinous. Areas of thyroid with active cells and colloid-poor follicles look like raw beef. Mitochondria-packed Hürthle cells in a thyroid (i.e., Hashimoto's, some multinodular goiters, some adenomas) impart a brown color (why?)
Lone colloid nodules -- easily diagnosable because their contents are too viscous to be aspirated by an 18-guage needle -- can be huge; they're now ablated by ethanol injection (AJR 191: 1730, 2008).
Nuclear medicine plays an important role in thyroid testing. Active glands (or active nodules in a less-active gland) appear "hot" on scintiscan. Inactive glands (or inactive nodules within a gland) appear "cold".
{09362} normal scan
{09363} cold nodule, right upper pole
Hopefully you remember what thyroid hormones do. Thyroid disease is common and easy to treat effectively, but its onset is insidious and it is often overlooked. "Idiopathic goiter" affects maybe one older adult in 20 and is of negligible significance. Serious thyroid disease mimics "psychiatric disease". This is unfortunate. Hopefully you won't fall into this trap.
Thyroid cancer is the most common endocrine cancer and causes around 1000 deaths per year (current textbooks give figures that are too high). Papillary carcinoma is the most common but the least deadly; most cases are never detected in life. Follicular carcinoma is aggressive. Medullary carcinoma is aggressive. Anaplastic carcinoma is the least common but ultra-aggressive. Many thyroid tumors, both benign and malignant, are incidental autopsy findings (Cancer 64: 1888, 1989).
* The non-disease "black thyroid" is deposition of a pigment (no one knows exactly what) in the thyroids of patients treated long-term with minocycline (Arch. Path. Lab. Med. 118: 79, 1994).
CRETINISM
{49456} cretin, age 4 months
Hypothyroidism, presenting first in infancy or childhood. It may be due
to hypothyroidism during pregnancy (permanent brain damage), or to
a problem with the child's thyroid gland.
Often there is an inborn error of metabolism (most often a mutation
in the thyroid peroxidase gene). Or the thyroid may simply fail to form -- an
inquiry into the epidemiology of "thyroid dysgenesis" revealed not a clue
as to why this happens.
These people remain like small children
both mentally and physically throughout their lives. Replacing thyroid hormone later in life helps,
but does not reverse the damage (J. Clin. End. Metab. 70: 336, 1990); for best results,
you must treat before the third week (J. Ped. 136: 292, 2000).
The severity of the disease varies. If a mother is severely iodine-deficient, the child will be
profoundly retarded, deaf and spastic ("neurologic cretinism"). Less-severely affected children, such
as those who cannot make their own thyroid hormone after birth, fail to thrive and remain stunted.
They are likely to show any or all of the problems of adult myxedema.
Unless the cause is absence of thyroid hormone receptors, cretinism should never, ever develop. In
the U.S., all babies are screened shortly after birth, and impending cretinism is treated. (Even the
most fiscally-conservative politicians understand this: Each test costs a few dollars, and treatment
is cheap and simple, but lifetime care of a cretin costs megabucks. Ditto for phenylketonuria.)
* The early screening will often miss iodotyrosine dehydrogenase deficiency,
which will produce a goiter and hypothyroidism with the danger of neurologic
damage if it is missed: NEJM 358: 1856, 2008.
EPIDEMIC CRETINISM is the result of endemic dietary deficiencies in iodine. I would conclude from this that iodine deficiency has been a limiting factor on human populations,
and the ability of people to function as they should, throughout much of the world throughout most
of history. I would also consider ready-available iodine to be one undeniable blessing of science.
SPORADIC CRETINISM is the result of some kink in development or metabolism.
Causes of sporadic cretinism:
You need to treat these kids aggressively with thyroid supplements; undertreating cretinism is
disastrous: J. Ped. 125: 147, 1994.
ACQUIRED HYPOTHYROIDISM (Lancet 363: 793, 2004 -- it's often missed even though this should never happen)
CATEGORIES
PRIMARY HYPOTHYROIDISM means the thyroid gland is under-functioning because of some problem
other than insufficient hTSH.
SECONDARY HYPOTHYROIDISM ("central hypothyroidism")
means the gland is hypo-functioning because it is being under-stimulated
by too little hTSH, reflecting a primary problem in the pituitary gland.
Please don't miss this.
TERTIARY HYPOTHYROIDISM (the other "central hypothyroidism") means there is too little hTSH because
there is too little TRH, i.e., a primary problem in the hypothalamus.
Uncommon but not ultra-rare (Pitutiary 11: 181, 2008); it will come up
most often in patients who actually have "euthyroid sick syndrome"
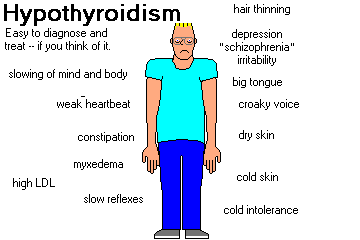
SIGNS AND SYMPTOMS OF HYPOTHYROIDISM
SLOWING OF MIND AND BODY is the prime problem. Mental slowness,
fatigue, irritability, and loss of interest
may be mistaken for, and treated as, "depression" (they should revoke somebody's
license, but it
happens every day), or there may be hallucinations and delusions ("myxedema madness"). This
progresses to profound disability, MYXEDEMA COMA and death.
NOTE: Down's syndrome (trisomy 21) folks often (at least 50% of the time) get at least a
chronic lymphocytic
thyroiditis, and they may end up hypothyroid. Don't overlook this, or assume the mental
slowness is just part of Down's. In fact, there is now a trend to supplement Down's children
with thyroxine while they are young; this seems to help growth and development
(J. Clin. Endo. Metab. 90: 3304, 2005).
MYXEDEMA properly refers to accumulation of hydrophilic ground substance throughout the
connective tissues of the body; this leads to coarsening of the facial features, enlargement of the
tongue, puffiness around the eyes, and deepening and croaking of the voice.
* Future pathologists: Mucoprotein in the ducts of sweat
glands is a tipoff to myxedema.
{24611} myxedema
LDL CHOLESTEROL increases strikingly, and this promotes atherosclerosis.
CARDIAC DYSFUNCTION ("hypothyroid cardiomyopathy") leads to low heart rate and loss of cardiac
strength. The end-stage myxedema patient's heart is a typical dilated cardiomyopathy. The
accelerated atherosclerosis doesn't help, either. This is another reason to treat hypothyroidism
gingerly.
CONSTIPATION is common.
WEIGHT GAIN is usual, and beware of sleep apnea.
DRY SKIN and COARSE, BRITTLE HAIR that may fall out in patches or all over.
YELLOWISH DISCOLORATION OF THE SKIN (for some reason, these people tend to get more carotene in the
bloodstream -- actually true * Int. J. Vit. Nutr. 69: 132, 1999)
COLD INTOLERANCE (poor perfusion of the extremities, sluggish mitochondria)
DELAYED DEEP TENDON REFLEXES ("hung reflexes") is a helpful physical sign.
CAUSES OF HYPOTHYROIDISM LATER IN LIFE
BIRTH DEFECTS
THYROGLOSSAL DUCT CYSTS are bits of the old thyroglossal duct. The cysts may be lined by thyroid
and/or squamous epithelium (why?), always with some lymphoid tissue (why?) Protruding the tongue
as far forward as possible will cause the cyst to rise. Savvy surgeons
treat these midline cysts by removing them along with the center of the hyoid bone to prevent
recurrence (why?)
{49471} thyroglossal duct cyst, patient
Bits and pieces (or all of) the thymus and/or parathyroids may lie within the thyroid capsule. Bits of
extra thyroid may be found elsewhere, notably on the tongue (the annoying "lingual thyroid").
{21529} lingual thyroid
In some folks, the thyroid gland just never develops. Unless the hormone is replaced, these people
will become cretins. Gene J. Clin. Endo. Metab. 86: 234, 2001.
HASHIMOTO'S THYROIDITIS ("chronic autoimmune thyroiditis": NEJM 335: 99, 1996)
{09241} Hashimoto's, gross
A common, chronic, progressive thyroid disease. There are
maybe 1,000,000 Hashimoto cases in
the U.S. Most patients are adults, and as with most autoimmune disease there is a female
preponderance, but no age or sex is immune. The autoantigen is thyroglobulin and/or
peroxidase in the microsomes.
Patients are likely to have a goiter. Most are euthyroid, many are hypothyroid, and a few are at least
temporarily hyperthyroid ("Hashitoxicosis", "Toximoto's disease").
If you biopsy it (and you usually don't), patients with Hashimoto's disease will exhibit (1) lots and
lots of lymphocytes in the thyroid gland; (2) germinal centers; (3) plasma cells; (4) Hürthle cells
(i.e., cells packed with mitochondria, also called "oncocytes"; they probably don't make thyroid
hormone).
The unusual "fibrosing variant" features more fibrosis, more scar contraction, and less of everything
else. Unlike Riedel's, it stays within the gland.
* Some physicians distinguish a non-Hashimoto "primary thyroid atrophy"
with a very small thyroid gland with most of the cells lost ("Ord's disease")
but this is probably just a Hashimoto's variant, as both feature
the same autoantibodies, and the size range isn't bimodal (J. Clin. Endo. Metab. 94: 833, 2009.)
We've already seen this disease as the prototype of antibody-dependent cell-mediated cytotoxicity.
More in keeping with some of
the newer work on Sjogren's, type I diabetes, etc., etc., we now know that Hashimoto thyroids
express HLA-DR antigens on their follicular cells, and this might get the process going.
These people have increased rates of autoimmune addisonism, pernicious anemia,
Sjogren's, vitiligo, and type I diabetes. We'll talk about the autoimmune
polyendocrine syndromes when we discuss
the adrenals.
PITFALL: You remember that many Hashimoto patients have SCHMIDT'S SYNDROME -- coexisting
autoimmune adrenalitis with addisonism. Further, if
there's a problem with the pituitary or hypothalamus causing the hypothyroidism, there's likely to be
concurrent secondary adrenal insufficiency. So... before you give that patient in myxedema coma a
nice booster of thyroid hormone, first administer glucocorticoid so as not to cause death from acute
adrenal insufficiency!
We will review Hashimoto's encephalopathy, a vasculitis involving the
subcortical white matter, under "CNS". Thankfully only about 1% of Hashimoto's
patients get this. Don't forget about it, or assume the patient has "MS" or "Alzeimer's"
or "idiopathic epilepsy". Autopsy findings Neurology 61: 1124, 2003.
NON-HASHIMOTO LYMPHOCYTIC THYROIDITIS
Abundant lymphocytes in the thyroid gland, but without germinal centers, plasma cells, or Hürthle
cells (Cancer 68: 1944, 1991). This is extremely common, especially in older
women.
In the very common "chronic lymphocytic thyroiditis",
there may be a small goiter, and there may be transient hyperthyroidism. Nobody really knows the
cause or the relationship to DeQuervain's, Hashimoto's, etc.
Postpartum thyroiditis, one variant of "subacute lymphocytic thyroiditis", has been studied well and has
increased expression of HLA-DR antigens on the surfaces of the follicular cells (no surprise; Am. J.
Clin. Path. 100: 200, 1993).
This pathologist suspects the histopathology covers several diagnostic entities, including the ill-defined
PRIMARY AUTOIMMUNE MYXEDEMA, often seen in Down's. To date, there is no international classification of thyoriditis, and
nowadays you'll probably just hear both Hashimoto's and non-Hashimoto's
called "chronic autoimmune thyroiditis" (NEJM 335: 99, 1996).
Be this as it may, lots of kids have goiters because of lymphocytic
infiltration, some will be euthyroid, some will be
hypothyroid, and you'll make these goiters shrink with thyroid hormone
therapy (J. Clin. Endo. Metab. 91: 1729, 2006; J. Clin. Endo. Metab. 92:
1647, 2007).
DEQUERVAIN'S SUBACUTE GRANULOMATOUS THYROIDITIS ("thyroid virus infection")
{09247} DeQuervain's
Thyroiditis review for the primary care physician: Am. Fam. Phys. 61: 1047, 2000;
Am. Fam. Phys. 73: 1769, 2006.
Despite "Big Robbins", infections involving the thyroid gland are extremely uncommon, with the
outstanding exception of DeQuervain's, a common, usually-missed, usually-mild disease.
In "DeQuervain's", the thyroid follicle cells die off in patches, almost certainly the result of some
virus or other. Known culprits include
mumps As you'd expect, the gland becomes large and painful. If you are foolish enough to biopsy the gland,
you will see a spectacular granulomatous response to the released colloid (probably
not "sequestered antigens"; it looks like a typical foreign-body reaction to glop).
Most patients are young adult women, but nobody is immune. The major problem is generally the
pain (neck, or referred to ear; "take two aspirins"), though sometimes the process is painless.
Occasionally, enough thyroglobulin may be broken down to produce transient hyperthyroidism, or
enough of the gland may be destroyed to produce hypothyroidism. The sed rate goes way up (why?)
In weeks to months, things settle down and the disease goes away by itself. Despite the impressive
histology during the illness itself, I've never seen what I thought was "old scarring from
DeQuervain's" at autopsy.
* DeQuervain's producing "acute mental illness": South. Med. J. 100: 837, 2007.
RIEDEL'S THYROIDITIS ("Riedel's struma"; review J. Clin. Endo. Metab. 87: 3545, 2002;
Am. J. Clin. Path. 121: 550, 2004)
{49460} Riedel's
A thankfully
rare process in which fibroblasts proliferate and lay down collagen, usually as broad, keloid-like bands. Most patients are older
women, who present with a rock-hard ("woody", etc.) neck mass.
Riedel's does not respect the thyroid capsule, or anything else. (This makes
it easy to tell from fibrosing Hashimoto's.)
It mimics an invasive sarcoma, but there is no anaplasia or necrosis.
Enough of the gland may be destroyed to produce hypothyroidism.
Surgical exploration may be
required to relieve pressure on the trachea. Fortunately, the disease generally stops before the
patient asphyxiates.
CATEGORIES
PRIMARY HYPERTHYROIDISM means the thyroid gland is over-functioning because of some problem
other than excess hTSH.
SECONDARY HYPERTHYROIDISM means the gland is hyper-functioning because it is being overstimulated
by too much hTSH, reflecting a primary problem in the hTSH-producing organ. (The most common
cause may be ectopic hTSH production by a choriocarcinoma).
TERTIARY HYPERTHYROIDISM means there is too much hTSH because there is too much TRH. It is almost
never mentioned in the literature and is probably very rare.
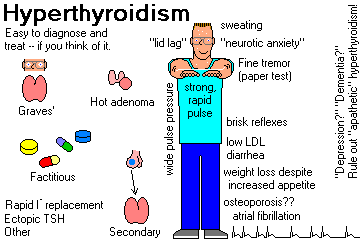
SYMPTOMS AND SIGNS OF HYPERTHYOIRIDISM
HYPERMETABOLISM is manifest by weight loss, muscle atrophy, heat intolerance, increased appetite.
Basic thermodynamics tells what's happening: Food is being burned for heat rather than for ATP
(i.e., oxidative phosphorylation is being uncoupled). Patients sweat (and their skin feels moist) and
develop hyperdynamic pulse.
INCREASED MENTATION may or may not make the person smarter, but it'll make them more anxious and
labile ("You're not sick, it's nerves.") In the very elderly, APATHETIC
HYPERTHYROIDISM may appear
instead, and be mistaken for Alzheimer's.
ENHANCED EPINEPHRINE EFFECT shows as tremulousness and "anxiety". (Try this: Take a sheet of paper
and lay it over the backs of the patient's outstretched hands. A very fine fluttering speaks for
hyperthyroidism). Blocking the epinephrine receptors with
propranolol is a big help while you're stabilizing a Graves's patient prior to
definitive treatment.
LID LAG is a delay in downward movement of the upper eyelid as the patient looks down. The
upper eyelid tends to be held too high anyway. (This "bug-eyed" appearance is common to all
hyperthyroid patients; it is enhanced by the ophthalmopathy of Graves's disease.)
ATRIAL FIBRILLATION (or other atrial arrhythmia) is particularly likely to result from hyperthyroidism.
(George Bush Sr.'s disease.) There is no consensus on the nature (or even the existence) of
HYPERTHYROID CARDIOMYOPATHY.
MILD DIARRHEA may be present.
OSTEOPOROSIS is a very serious long-term complication of hyperthyroidism.
LDL CHOLESTEROL goes down, which is nice as far as the arteries are concerned.
THYROID STORM ("thyrotoxic crisis") is the most dreaded problem in hyperthyroidism. This is
development of extreme hypermetabolism, leading to coma and death, when the hyperthyroid patient
is subjected to some other major physiologic stress.
THE CAUSES OF HYPERTHYROIDISM
GRAVES'S DISEASE (NEJM 358: 2704, 2008)
{09235} Graves's
This is a common problem caused by autoantibodies directed against the hTSH receptor. The
receptor mistakes them for TSH.
Nobody knows the cause of the autoantibody production.
The nature of the disease has been clarified by a good mouse model using either of two monoclonal antibodies
that produce somewhat different pictures
(J. Immuno. 176: 5084, 2006).
Patients also usually exhibit ophthalmopathy (the usual "lid lag", etc., of hyperthyroidism, plus
weak eye muscles plus excess collagen and ground substance behind the eyeball ("orbitopathy"), causing
PROPTOSIS-EXOPHTHALMOS).
There are usually antibodies against both eye muscles and against the fibroblasts
behind the eye and on the shin.
{09355} Graves's exophthalmos
To complete the triad, patients often exhibit myxedema-like nodules confined to the anterior aspects
of the lower extremities ("pretibial myxedema").
* Try a generous dose of a topical glucocorticoid for the pretibial myxedema
(J. Clin. Endo. Metab. 87: 438, 2002).
{09360} pretibial myxedema
Whether or not the complete triad is present, "Graves's" is the usual cause of
DIFFUSE TOXIC GOITER
(weight up to 100 gm, seldom more, since there's little colloid). You're likely to hear a bruit over
the gland (why?), and at surgery (oops), untreated Graves's will be beefy red.
If you examine an untreated Graves's thyroid gland under the microscope ("oops!"), you'll see scanty
colloid, typically being actively resorbed ("bite marks", "scalloping") around its edges.
{24717} Graves's with scalloping
If the patient has been pre-treated with a goitrogen, you'll less colloid and more papillary formations
(why?) If the patient has been treated with a huge dose of iodine to suppress thyroid hormone
formation, you'll see a colloid goiter (why?)
Today, most patients prefer to take a drink of I131, though they know this will eventually make them
hypothyroid. The ophthalmopathy may require an ophthalmologist's care.
NOTE: Sometimes antibodies merely block the effects of hTSH. This may be seen in both
Hashimoto's disease and in "primary idiopathic hypothyroidism". Not rare, and may self-cure.
NEJM 326: 513, 1992.
ATROPHY OF THE THYROID
{17447} burned-out thyroid; this could be anything from old I131 injury to old Hashimoto's to
Riedel's to a really gone patch in a nodular goiter.
Every so often, at autopsy of an adult, the thyroid is shrivelled to a miniature thyroid-shaped nubbin
of white scar tissue, weighing perhaps a gram. Trying to guess the cause is fun but usually
futile.
If you see giant nuclei and hyalinosis of small arteries, perhaps the patient forgot she had once taken
a drink of I131. Other cases may be burned-out Hashimoto's or DeQuervain's. Of course, if there's
no pituitary gland, the thyroid may have died of under-stimulation.
* Future pathologists: the rare AMYLOID GOITER
features amyloid AA and often extensive fatty ingrowth. It remains
a minor mystery of medicine. See Arch. Pathol. Lab Med. 124: 281, 2000.
{21053} colloid goiter
Diffuse enlargement of the thyroid gland was historically due to
EPIDEMIC GOITER, caused by lack of
iodine in the diet (i.e., any community far from the seashore). This was often exacerbated (or even
primarily caused by) goitrogens in the diet.
WARNING: The iodine-deficiency thyroid gland is under heavy TSH stimulation (why)? When an
iodine-deficient patient is treated with a large amount of iodine, acute hyperthyroidism and even
hyperthyroid crisis can supervene. This is the dread
JOD-BASEDOW phenomenon.
When iodized salt is introduced into a region that is significantly iodine-deficient,
the number of people being treated for hyperthyroidism seems to increase,
then drop to the usual within six years (the Danes: J. Clin. Endo. Metab. 94:
2400, 2009) as goitrous thyroids that have been in overdrive for years settle back down.
Beyond this, I am not aware of any reason to believe that the obscure WHO claim that too much iodine in the
diet cases hyperthyroidism is true.
* SPORADIC DIFFUSE GOITER, once mysterious,
is now known to be (at least in many cases)
the result of incomplete inborn errors
of metabolism. These include (1) partial inability of stomach or thyroid to take up
iodine; (2) partial lack of peroxidase to link iodine to tyrosine (fairly common... J. Clin. Endo. Metab. 93: 627, 2008); (3) partial inability to recycle iodine in the thyroid
gland; (4) partial inability to crunch the two iodotyrosine moieties together to make T4. Others are
described.
A small diffuse goiter is almost the rule rather than the exception around menarche.
Early in its development, the colloid goiter shows hyperplasia (i.e., tall cells, maybe piling-up) under
the influence of TSH. Later, the cells appear to give up, and the gland becomes a mass of oversized,
colloid-packed follicles. Of course, the process is never really uniform, and eventually the diffuse
nontoxic goiter turns into a MULTINODULAR GOITER. By the time the gland reaches over 100 gm, the
multinodular stage is usually well-underway.
In a multinodular goiter, there are many nodules, most composed of follicles more or filled with
colloid, others representing sites of old hemorrhage and fibrosis ("Feel my goiter!" "Oops, I bumped
my neck!") You can see squamous metaplasia, foam cells, masses of hemosiderin,
foreign-body granulomas,
and many other interesting things.
Rule: If the excised portion of thyroid contains two "adenomas", go ahead and call it a
nodular goiter.
A microscopic survey of a nodular goiter is enough to make anyone think about
selection of mutant clones in precancer seriously, and
this is supported by the finding that many genetically distinct clones of cells with various functional
problems. (Clonality in the nodular goiter revisited: Am. J. Path. 134: 141, 1989; hot-spot
ras
mutations in goiter nodules: Mol. End. 4: 1474, 1990). However,
the common genetic basis remains obscure. (J. Clin. Endo. Metab. 87:
4264, 2002).
Multinodular goiter often arises de novo,
either sporadically or in certain anti-oncogene deletion syndromes (notably Cowden's).
Usually there are no new functional problems with the thyroid gland in multinodular goiter, but
sometimes a clone of cells may turn "hot", causing hyperthyroidism. Fortunately, carcinoma very
seldom arises in multinodular goiter, and most "cold nodules" removed from thyroid glands turn out
simply to be sleepy nodules from multinodular goiters.
No one really knows how to manage cancer risk in a thyroid with several
nodules. Of course, if there are just a few, there will be a lot of fine-needling,
but when there are massive numbers, controversy remains (J. Clin. Endo. Metab. 91:
3411, 2006).
THYROID TESTING (see Lancet 357: 619, 2001) Serum T4 will give you the total bound plus unbound. Serum free T4 will give you the unbound,
but it is more expensive. Serum T3RU (T3 resin uptake) is an unfortunately-named test that gives
you a value inversely proportional to the number of unbound sites on the serum thyroid hormone
carrying proteins (remember them?) Multiply T4 and T3RU to get "free thyroxine index", a
measure of the biologically active hormone.
Quiz: Who remembers what proteins carry T4 and T3? Answer: Thyroxine-binding protein (TBG,
lion's share), transthyretin ("prealbumin"), and albumin. What's the best way to raise TBG? Take
estrogen. What does this do to total T4? T3RU? Free T4? TSH?
Serum T3 of course measures the active hormone. You can get a serum free T3 also. Some toxic
nodules make T3 instead of T4, so it's often worth checking (Am. J. Med. 96: 229, 1994).
Quiz: Suppose somebody took T4 to lose weight and got sick it ("factitious hyperthyroidism").
How would the tests be affected? Suppose the person took pure T3 instead?
The newer, super-sensitive TSH assays are a good way to screen for hyperthyroidism (TSH in
primary, in secondary or tertiary) and hypothyroidism ( in primary, in secondary or tertiary).
Some people say that patients may actually be suffering from symptomatic thyroid disease if hTSH
is abnormal but T7 is in the normal range (i.e., "not everybody has the same 'normal' thyroid
hormone levels".) hTSH has long been the best screen for cretinism. (There are now calls
for additional screening to detect congenital secondary hypothyroidism, which of course
looking for a high hTSH will miss: J. Clin. Endo. Metab. 90: 3350, 2005).
Nowadays, we talk about "subclinical thyroid disease" defined to be a hTSH
outside the normal range, free thyroxine and free triiodothyronine in the normal
range, and no symptoms or signs. It often declares itself as real thyroid
disease in a few years, but so far, no one knows what to do about it (Am. Fam. Phys.
72: 1517, 2005).
On thyroid scans, cold nodules are the ones most likely to be malignant (why?) Hot nodules are the
ones most likely to produce hyperthyroidism. You'll learn how to manage both on rotations. In
hyperthyroidism due to most causes, the gland will be hot, but in struma ovarii, DeQuervain's, or
factitious hyperthyroidism, it will be cold (why?)
Serum thyroglobulin will often be increased in thyroid cancers (papillary, follicular) or in
DeQuervain's (why?). For use of thyroglobulin in detecting the spread of well-differentiated
thyroid carcinoma, see the update from Mayo's at J. Clin.
Endo. Metab. 92: 4278, 2007; also J. Clin. Path. 62: 402, 2009 (the assay is a difficult and problematic one).
When you are monitoring thyroid hormone replacement in somebody who has been hypothyroid,
the conventional wisdom is to try to avoid their becoming even a little bit hyperthyroid, since this will supposedly lead to
osteoporosis in the long run. However, some people actually do not feel well until
the free T4 is somewhat above the upper limit of normal (Br. Med. J. 326:
295, 2003), and I'd trust the body's wisdom on this. Currently, clinicians
make sure that hTSH stays in the normal range. If, on the other hand, you are administering
thyroxine to suppress a hTSH-dependent thyroid cancer, be sure that you give enough so that hTSH
levels remain zero.
During serious
illness or injury, some people have diminished intracellular conversion of T4 to
T3 by the deiodinases.
EUTHYROID SICK SYNDROME ("low T3 syndrome"; "the non-thyroidal illness syndrome") is recognized, for research
purposes, in patients who are
seriously sick with something serious have low T3's and high rT3's (i.e.,
T4 is getting metabolized wrong). hTSH levels tend to stay in the okay range.
It is a real entity
(J. Clin. Endo. Metab. 90: 5613, 2005), is very common
in the very-sick and the malnourished if you look for it,
and (at least in ICU patients on the ventilator) somewhat ominous
overall (Chest 135: 1448, 2009). And it will confuse you
when you are caring for the very-sick. The conventional wisdom
is that you do not treat it (i.e., you do not administer
extra T4 or T3); not everybody agrees (Am. Heart. J. 135:
187, 1998; discussion is ongoing). There are so many proposed explanations
for "euthyroid sick syndrome" that I urge you not even to start trying to figure it out.
* Now, you are familiar with the selenium-dependent enzymes
that turn T4 into usable T3 in the tissues.
Deficiencies of course are known; these people seem to do okay
but of course have high rT3, low T3,
high FT4, and usually
normal hTSH (see for example J. Clin. Endo. Metab. 94: 4003, 2009.)
There are two schools of thought on managing thyroid replacement
therapy -- by the numbers or by how the patient feels.
I have often wondered whether (1) a "normal" serum T4 might still
be low for that person, and whether (2) a "normal" serum T4 might
not mean a normal T4 in the brain milieu.
Physicians who fear being sued decades later for "causing osteoporosis"
are reluctant to approve patients who feel best when they take a bit
more thyroxine than "the lab tests say they need". I'm not a clinician,
but we have a saying in pathology, "Listen to the patient, not
the numbers." I'm not alone (Br. Med. J. 320: 1332, 2000;
Br. Med. J. 326: 295, 2003)
* This brings us to
a late 1990's fad diagnosis, WILSON'S SYNDROME. Supposedly
this results from faulty metabolism of T4 into rT3
at the tissue level.
People interested in complementary medicine are invited
to take their body temperature repeatedly, and if it is "a few tenths of a degree
below 98.6" at any time of the day, and they have any of a huge list of
symptoms, then the diagnosis is considered established and the patient gets
a series of "complementary" remedies. Before you diagnose or treat yourself
or somebody else, please consider these facts: * Do you remember those deiodinases? Selenium takes the place
of sulfur in their cysteines!
In suspected Graves's disease and Hashimoto's disease, you can order a battery of anti-TSH receptor
autoantibodies ("thyroid stimulating antibody", "long-acting thyroid stimulator"=LATS), anti-thyroglobulin antibodies , and
anti-microsomal antibodies.) Interpretation is rather cloudy, though
very high titers of anti-microsomal antibodies (against the peroxidase autoantigen,
of course) is pretty specific for Hashimoto's.
If you've got a bump in your thyroid, a pathologist will be happy to FINE-NEEDLE ASPIRATE it, and look at the
cells on a slide.
Review of 4700 cases from Galveston: Cancer 111: 306, 2007 (it's accurate).
How to do it right: J. Cln. End. Metab. 79: 335, 1994;
Mayo Clin. Proc. 69: 44, 1994; some sub-subspecialty training
is advised for pathologists who want to do this (Cancer 107: 406, 2006). Using it with ultrasound to be sure you hit
the itty-bitty nodules: Otolar. 123: 700, 2000.
The procedure is not perfect, and there are still plenty of false-positives
and false negatives; the most common problem is the all-too-human attempt
to interpret an unsatisfactory specimen (Am. J. Clin. Path. 125: 873, 2006).
Patients may be concerned that the needling will spread the cancer;
this is very rare but does happen (J. Laryn. Otol. 121: 268, 2007.
This is really a screening technique to find out which bumps to cut
out, and it is the one instance in which a decision to perform
such serious surgery may be based on a few cells in a cytology smear.
The practice is now standard, and has greatly reduced the number
of people who need to be operated for diagnosis.
Update on this now-huge field: CA 59(2): 99, 2009
Please remember that we CANNOT tell benign from low-grade-malignant follicular
lesions of the thyroid using fine-needle aspiration.
A surgeon should remove the bump if the fine needle aspirate shows:
![]() Cretin
Cretin
Classic drawing
Adami & McCrae, 1914
These children may
get enough thyroid from Mom while in the womb, but after they are born, cannot make
their own. However, this is not always the case -- there may not be
sufficient thyroixine transferred across the placenta.
When a goiter is picked up on ultrasound before birth,
thyroxine may be administered by injection into the unborn child
(J. Clin. Endo. Metab. 94: 3731, 2009) to prevent developmental
defects and delivery problems due to the goiter itself.
It is scandalous that this
should exist anywhere in the world in the 21st century.
Yet it remains commonplace in the world's current goiter belts,
outstandingly western Mainland China ("the people's paradise"), Tibet
(NEJM 339: 1112, 1998), central Java, Sikkim (India), Afghanistan
(horrible problem through the 1990's: World Health Forum 17: 209, 1996),
Nepal,
central Africa (Am. J. Clin.
Nutr. 52: 1087, 1990), and some jungle tribes (J. Clin. End. Met. 77: 878, 1993).
Iodine deficiency in children remains rampant ("the new South Africa" Am. J. Clin. Nutr. 86:
1040, 2007).
The fault is NOT with the world's poor -- they simply are not given
access to iodine.
{25468} myxedema
{25469} myxedema
{09245} thyroglossal duct cyst, histology
{08960} Hashimoto's, histology
{08961} Hashimoto's, histology
{09242} Hashimoto's, histology
{37881} Dr. Hashimoto
{37882} Dr. Hashimoto "after 40 years of teaching"
![]() Hashimoto's Disease
Hashimoto's Disease
Text and photomicrographs. Nice.
Human Pathology Digital Image Gallery
![]() Hashimoto's thyroiditis
Hashimoto's thyroiditis
Germinal centers, damaged parenchyma
KU Collection
* This "cirrhosis of the thyroid"
was actually what Dr. Hashimoto's original
paper described.
* A classic rat model is based on an
immunogenic sequence within thyroglobulin (J. Immunol. 149: 1039, 1992); similar antibodies
may be seen in humans with Hashimoto's or "nonspecific" thyroid disease (Arthr. Rheum. 34: 1585,
1991).
{24721} DeQuervain's
![]() DeQuervain's
DeQuervain's
WebPath Photo
![]() ,
coxsackie B
,
coxsackie B![]() (most common),
EBV
(most common),
EBV![]() ,
ECHO, and
adenovirus
,
ECHO, and
adenovirus![]() . There are surely others. Epidemic DeQuervain's: J. Clin. End. Metab. 70: 396, 1990.
. There are surely others. Epidemic DeQuervain's: J. Clin. End. Metab. 70: 396, 1990.
HYPERTHYROIDISM (Lancet 362: 459, 2003; Am.
Fam. Phys. 72: 635, 2005)
* "Subclinical hyperthyroidism", with low hTSH but "normal range" thyroid
hormone levels, seems to put a lot of older folks at risk for atrial fibrillation
and overall mortality. Screening and treating might be wise. Lancet 373: 1930, 2009;
children and teens (especially pudgy ones) J. Clin. Endo. Metab. 94: 2414, 2009.
{09237} Graves's
{09356} Graves's exophthalmos
* There are autoantibodies against fibroblasts located here
(J. Clin. Endo. Metab. 80:
3427, 1999). For some reason, fibroblasts on the shins, and only on the shins,
evidently have TSH receptors (!) J. Endo. Inv. 19: 365, 1996.
{25470} pretibial myxedema
{25471} pretibial myxedema
{25472} pretibial myxedema
![]() Burned out thyroid
Burned out thyroid
No history -- surprise at autopsy
KCUMB Team
DIFFUSE NONTOXIC GOITER ("colloid goiter") / (MULTI)NODULAR GOITER
{21054} colloid goiter
{19502} colloid goiter, around 100 gm
{09354} colloid goiter, gross
{19505} colloid goiter, histology
{19511} colloid goiter, histology
{10825} nodular goiter
{12710} nodular goiter (this was billed as "Hashimoto's"; I doubt it)
{39052} nodular goiter (dominant nodule was called "adenoma", heh heh)
{09238} nodular goiter, gross
{49451} nodular goiter, gross
{09240} nodular goiter, histology
{49465} nodular goiter, they decided to operate
![]()
![]() Thyroid gland with diffuse hyperplasia
Thyroid gland with diffuse hyperplasia
What could this be?
Wikimedia Commons
![]() Big inactive follicles
Big inactive follicles
Nodular goiter / Could be other things too
WebPath Photo
* "Jod" is German for "iodine", and "Basedow's disease"
their term for any hyperthyroidism.
This is mediated by the cytokines of the acute phase
reaction, and to be usual, correlating with the drop in albumin
(Surgery 123: 560, 1998).
Nobody knows whether this is good (diminishing energy use during convalescence)
or bad, and replacement
Of course, labs can be normal or abnormal,
and the patients can feel well or ill.
Today's terminology:
![]() Oxalate crytsals in the thyroid
Oxalate crytsals in the thyroid
Curiosity of no significance
KCUMB Team